-
脓毒症是指因感染引起的宿主反应失调导致的危及生命的器官功能障碍,如果控制不及时,可能会发展为脓毒症性休克和多器官功能障碍综合征(MODS),病情进展急速且凶险[1]。脓毒症病人的死亡率文献报道不太一致,最高可达20%~80%,是造成急诊科和ICU病人死亡的常见疾病之一[2]。脓毒症性休克会造成病人多脏器的损伤,肾脏是其中最容易损伤的靶器官之一,因此,早期复苏成功和多器官功能支持对脓毒症病人的后续治疗及多脏器功能维护非常重要[3]。参附注射液是来源于中医古方“参附汤”,其具有扩张冠状血管、降低心肌耗氧量、减轻心肌缺血再灌注损伤以及抑制致炎因子的损伤等作用。尽管参附注射液已在临床广泛应用,但其是否有保护脓毒症病人的肾脏、肝脏及其他脏器功能的作用尚不明确。本文通过研究参附注射液对脓毒症病人急性肾损伤的治疗效果及对肝脏、心脏及脑钠肽的影响,为临床治疗脓毒症提供一定的依据。现作报道。
-
收集2014-2016年于我院明确诊断且治疗的脓毒症病人72例为研究对象,采用随机数字法将所有病人分为观察组和对照组各36例。观察组男25例,女11例;年龄17~86岁;原发感染部位:肺部感染26例,其他部位感染10例;休克指数: < 2.0者28例,≥2.0者8例。对照组男25例,女11例;年龄19~90岁;原发感染部位:肺部感染24例,其他部位感染12例;休克指数: < 2.0者27例,≥2.0者9例。2组病人的年龄、性别、原发感染部位和休克指数构成等一般资料均具有可比性。诊断和纳入标准参照2012年国际脓毒症学会定义的脓毒症诊断标准进行[4]。排除标准:年龄 < 20岁者;孕妇及哺乳期妇女;有慢性肾功能不全者;合并其他药物中毒者;合并有恶性肿瘤者。病人全部签订书面知情同意书,并配合治疗。本研究经我院伦理委员会批准后实行。所有病人均有随访,截止至病人死亡或30 d内仍然存活。
-
2组均采用液体复苏、抗生素的合理使用和使用血管活性药物等综合治疗措施。治疗组将参附注射液(雅安三九药业)80 mL加入5%葡萄糖氯化钠溶液250 mL静脉滴注,对照组使用等量的5%葡萄糖氯化钠溶液(如果有糖尿病病史,均加入胰岛素),均每天1次,连续治疗7 d。
-
2组病人血清中肌酐(Cr)、血尿素氮(BUN)、胱抑素C(Cys C)、丙氨酸氨基转移酶(ALT)、天门冬氨酸氨基转移酶(AST)、乳酸脱氢酶(LDH)、心肌激酶(CK)、脑钠肽(BNP)等水平检测均按照试剂盒中的说明书要求操作。
-
观察2组病人治疗前后血清中Cr、血BUN和Cys C的水平变化情况,其他脏器损伤相关指标ALT、AST、LDH、CK和BNP等水平变化情况;观察2组病人治疗后生存时间及死亡情况,计算死亡率。
-
采用t(或t′)检验、χ2检验和生存分析(Kaplan-Meier法和log-rank法检验)。
-
治疗前2组病人血清中Cr、BUN和Cys C水平差异均无统计学意义(P>0.05);治疗后,2组病人血清中Cr、BUN和Cys C水平均较治疗前均显著降低(P < 0.01),且观察组病人降低程度(改善)明显优于对照组(P < 0.01)(见表 1)。
分组 n Cr/(μmol/L) BUN/(mmol/L) Cys C/(mg/L) 治疗前 观察组 36 114.2±67.8 11.8±5.1 2.1±1.2 对照组 36 112.6±42.7 12.6±9.0 2.3±1.1 t — 0.12* 0.46* 0.74 P — > 0.05 > 0.05 > 0.05 治疗后 观察组 36 70.5±39.6△△ 5.6±0.9△△ 1.1±0.4△△ 对照组 36 91.0±43.4△△ 6.8±1.5△△ 1.4±0.4△△ t — 2.09 4.12* 3.18 P — < 0.05 < 0.01 < 0.01 *示t′值;组内配对t检验:△△P < 0.01 表 1 2组病人治疗前后Cr、BUN和Cys C的水平变化比较(x±s)
-
治疗前2组病人ALT、AST、LDH、CK和BNP的水平差异均无统计学意义(P>0.05);治疗后,2组病人血清中ALT、AST、LDH、CK和BNP的水平均较治疗前明显降低(P < 0.01);且观察组病人降低程度(改善)明显优于对照组(P < 0.01)(见表 2)。
分组 n ALT/(U/L) AST/(U/L) LDH/(U/L) CK/(U/L) BNP/(pg/mL) 治疗前 观察组 36 95.3±24.8 96.4±25.4 730.3±110.3 400.1±101.8 419.1±75.7 对照组 36 96.3±50.2 93.6±47.2 731.1±213.2 407.4±84.8 413.9±103.5 t — 0.11* 0.31* 0.02* 0.33 0.24 P — > 0.05 > 0.05 > 0.05 > 0.05 > 0.05 治疗后 观察组 36 51.4±12.2△△ 49.9±11.3△△ 514.2±86.9△△ 228.0±93.4△△ 134.9±84.6△△ 对照组 36 72.0±25.9△△ 70.9±45.9△△ 630.3±209.2△△ 323.4±37.7△△ 244.8±80.3△△ t — 4.32* 2.67 3.08* 5.68* 5.65 P — < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 *示t′值;组内配对t检验:△△P < 0.01 表 2 2组病人治疗前后脏器损伤指标变化比较(x±s)
-
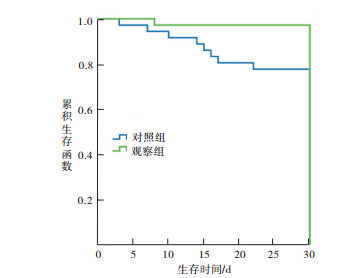
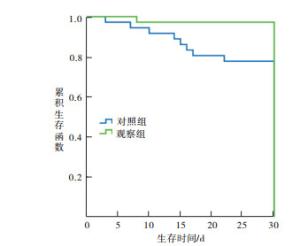
观察组病人治疗后死亡1人,存活35人,死亡率2.8%;对照组病人治疗后死亡8例,存活28例,死亡率22.2%;对照组病人的死亡率明显高于观察组(χ2=4.57, P < 0.05)。Kaplan-Meier生存分析提示观察组病人治疗后的生存时间明显长于对照组病人(log-rank=6.038,P < 0.05)(见图 1)。
-
感染、创伤和休克等应激情况下造成人体过度激活免疫系统引起的脓毒症,是炎症介质分子通过级联免疫反应、瀑布式释放引起的、无法控制的全身性炎症反应综合征,严重威胁着病人的身体健康[5-6]。进入新世纪以来,各种新技术、新方法不断涌现,但脓毒症病人的总体治愈率并没有显著提高[7]。因此,寻找有效的脓毒症治疗方案仍然是急诊医学治疗的热点问题之一。
脓毒症的发病机制目前仍然是急诊内科的研究热点问题之一,经典的理论认为其主要与机体炎症反应、内分泌调节紊乱、神经-体液异常调节等密切相关。近年来,有学者认为凝血功能紊乱也是导致病人脓毒症的关键因素,且充分参与脓毒症发生、发展的全过程[8]。脓毒症病人合并急性肾损伤后的预后明显更差,美国的一项研究[9]表明,当脓毒症病人发生病情加重后引起的严重脓毒症和脓毒症性休克后,其急性肾功能衰竭发生的概率分别增加了4%和32%。其他学者的研究[10]也表明急性肾损伤是脓毒症发生的独立危险因素。
临床上对脓毒症的治疗方法有很多种,主流方法包括液体复苏、合理使用抗生素和血管活性药物等一系列治疗措施。2014年中国严重脓毒症/脓毒性休克治疗指南中将中医药治疗也列入其治疗方案之一[11]。附片和红参等是中药参附注射液中的主要成分,其中红参中含有人参皂苷成分,可以有效扩张病人的冠状动脉。附片和红参相配,具有回阳救逆、益气固脱等功效。临床上判断肾功能常用的生化指标有血清Cr、BUN和Cys C等,当脓毒症引起急性肾损伤后,肾脏对蛋白代谢产物的排出能力降低,引起血液中Cr和BUN的含量升高[12]。当肾功能降低后,会导致肾小管的重吸收和降解小分子代谢产物的功能降低,从而引起血液中Cys C的含量增高。在本研究中,我们发现治疗后2组病人血液中的Cr、BUN和Cys C的水平均较治疗前显著降低;且观察组病人降低水平(改善)明显优于对照组。因此,上述结果表明常规治疗能够改善脓毒症病人的急性肾损伤,而添加参附注射液较单纯的常规治疗更能够改善脓毒症病人的肾功能。
参附注射液还可以抑制脓毒症对其他脏器功能的损伤。脓毒症过强时会引起机体自稳态失调,导致组织灌注不足,微循环障碍,促进了MODS的发生。现有研究[13-14]表明:(1)参附注射液能够增强心肌收缩力,降低心肌耗氧、扩张血管以及降低血液黏稠度和清除氧自由基,从而有效地改善休克引起的血压下降和组织灌注;(2)参附注射液能够抑制炎症介质肿瘤坏死因子-α、白细胞介素-1和白细胞介素-10的产生,使炎症介质释放和抗炎因子之间达到一个动态平衡,防止过度炎症反应和免疫抑制,从而减轻由于炎症反应所造成的病理损伤[13];(3)参附注射液还具有抗脂质过氧化、保护血管内皮以及血流变学指标等。
ALT和AST通常是用来反映肝细胞损伤的标志物;LDH、CK和BNP通常是用来反映心肌损伤的主要标志物。在本研究中,2组病人血液中的ALT、AST、LDH、CK和BNP水平均较治疗前显著降低,且观察组病人降低水平(改善)明显优于对照组,提示使用参附注射液治疗,能够更好地保护脓毒症病人的肝脏、心脏和肾脏功能,减少MODS的发生。生存率分析显示使用参附注射液能够降低脓毒症病人的死亡率。生存分析也表明观察组病人能够获得更长的生存时间。
综上所述,在脓毒症病人的基础治疗同时使用参附注射液,具有明显疗效,病死率低,并能够有效地保护肾脏、肝脏和心脏功能,减轻脓毒症对这些脏器造成的损伤。
参附注射液对脓毒症病人急性肾损伤的效果
Effect of Shenfu injection on acute renal injury induced by sepsis
-
摘要:
目的分析参附注射液对脓毒症病人急性肾损伤及其他脏器损伤的治疗效果。 方法将72例脓毒症病人随机分成对照组和观察组各36例,对照组病人按照指南给予标准治疗,观察组病人在标准治疗的基础上添加参附注射液。比较2组病人治疗前后血清肌酐、血尿素氮、胱抑素C水平的变化情况、其他脏器损伤以及死亡情况。 结果治疗前2组病人血清肌酐、血尿素氮、胱抑素C水平差异均无统计学意义(P>0.05),治疗后均比治疗前明显降低(P < 0.01),且观察组明显低于对照组(P < 0.01);治疗前2组病人丙氨酸氨基转移酶、天门冬氨酸氨基转移酶、乳酸脱氢酶、肌酸激酶及脑钠肽水平差异均无统计学意义(P>0.05),治疗后水平均明显降低(P < 0.01),且观察组低于对照组(P < 0.01);观察组病人的死亡率(2.8%)明显低于对照组(22.2%)(P < 0.05),且生存时间也长于对照组(P < 0.05)。 结论参附注射液可有效减轻脓毒症病人急性肾损伤及其他脏器损伤,降低死亡率。 Abstract:ObjectiveTo investigate the therapeutic effects of Shenfu injection in the acute renal injury and other organs injury induced by sepsis. MethodsSeventy-two patients with sepsis were randomly divided into the control group and observation group (36 cases each group).The control group was treated with routine method, and the observation group was treated with Shenfu injection combined with conventional method.The changes of the serum levels of creatinine, blood urea nitrogen and cystatin C in two groups between before and after treatment, and other organ damage and death between two groups were compared. ResultsThe differences of the levels of serum creatinine, blood urea nitrogen and cystatin C between two groups before treatment were not statistically significant (P>0.05), which were significantly higher than those after treatment, and the levels of serum creatinine, blood urea nitrogen and cystatin C in observation group after treatment were significantly lower than those in control group (P < 0.01).The differences the levels of serum alanine aminotransferase, aspartate aminotransferase, lactate dehydrogenase, creatine kinase and brain natriuretic peptide between two groups before treatment were not statistically significant (P>0.05), which in two groups significantly decreased after treatment, and the levels of serum alanine aminotransferase, aspartate aminotransferase, lactate dehydrogenase, creatine kinase and brain natriuretic peptide in observation group were lower than those in control group (P < 0.01).The death rate in observation group (2.8%) was significantly lower than that in control group (22.2%) (P < 0.05), and the survival time in observation group was longer than that in control group (P < 0.05). ConclusionsShenfu injection can effectively alleviate the acute kidney injury and other organs injury, and reduce the mortality in sepsis patients. -
Key words:
- sepsis /
- acute renal injury /
- Shenfu injection /
- creatinine /
- urea nitrogen /
- cystatin C
-
表 1 2组病人治疗前后Cr、BUN和Cys C的水平变化比较(x±s)
分组 n Cr/(μmol/L) BUN/(mmol/L) Cys C/(mg/L) 治疗前 观察组 36 114.2±67.8 11.8±5.1 2.1±1.2 对照组 36 112.6±42.7 12.6±9.0 2.3±1.1 t — 0.12* 0.46* 0.74 P — > 0.05 > 0.05 > 0.05 治疗后 观察组 36 70.5±39.6△△ 5.6±0.9△△ 1.1±0.4△△ 对照组 36 91.0±43.4△△ 6.8±1.5△△ 1.4±0.4△△ t — 2.09 4.12* 3.18 P — < 0.05 < 0.01 < 0.01 *示t′值;组内配对t检验:△△P < 0.01 表 2 2组病人治疗前后脏器损伤指标变化比较(x±s)
分组 n ALT/(U/L) AST/(U/L) LDH/(U/L) CK/(U/L) BNP/(pg/mL) 治疗前 观察组 36 95.3±24.8 96.4±25.4 730.3±110.3 400.1±101.8 419.1±75.7 对照组 36 96.3±50.2 93.6±47.2 731.1±213.2 407.4±84.8 413.9±103.5 t — 0.11* 0.31* 0.02* 0.33 0.24 P — > 0.05 > 0.05 > 0.05 > 0.05 > 0.05 治疗后 观察组 36 51.4±12.2△△ 49.9±11.3△△ 514.2±86.9△△ 228.0±93.4△△ 134.9±84.6△△ 对照组 36 72.0±25.9△△ 70.9±45.9△△ 630.3±209.2△△ 323.4±37.7△△ 244.8±80.3△△ t — 4.32* 2.67 3.08* 5.68* 5.65 P — < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 *示t′值;组内配对t检验:△△P < 0.01 -
[1] 张文喜, 段达荣, 张震宇, 等.参附注射液联合低分子肝素对小儿脓毒血症血浆NT-ProBNP、Cys、凝血功能和预后的影响[J].中国现代医学杂志, 2017, 27(2):61. doi: 10.3969/j.issn.1005-8982.2017.02.011 [2] 卢中秋, 卢才教, 洪广亮, 等.34例创伤弧菌脓毒症患者的流行病学特点及临床诊治[J].中华急诊医学杂志, 2009, 18(7):732. doi: 10.3760/cma.j.issn.1671-0282.2009.07.017 [3] 常瑜, 郝正玮, 郭霞, 等.参附注射液治疗脓毒血症的效果及影响因素的Logistic回归分析[J].实用药物与临床, 2015, 18(9):1055. [4] DELLINGER RP, LEVY MM, RHODES A, et al.Surviving Sepsis Campaign:international guidelines for management of severe sepsis and septic shock, 2012[J].Intensive Care Med, 2013, 39(2):165. doi: 10.1007/s00134-012-2769-8 [5] 陈佳顺, 姚盛.参附注射液治疗难治性脓毒血症并休克的临床观察[J].中国实用医药, 2016, 11(19):161. [6] 张国刚.参附注射液治疗30例脓毒症患者的临床观察[J].中国中医急症, 2015, 24(7):1268. doi: 10.3969/j.issn.1004-745X.2015.07.056 [7] 陈勉, 胡志华, 陈伟, 等.持续血液净化疗法治疗外伤继发性脓毒症临床效果及对高迁移率族蛋白1、肿瘤坏死因子-α和促血管生成素2的影响[J].中国现代医学杂志, 2014, 24(34):61. doi: 10.3969/j.issn.1005-8982.2014.34.015 [8] 田虹, 王洪霞.老年脓毒症患者凝血功能紊乱及与预后的关系[J].中国急救医学, 2014, 34(11):966. doi: 10.3969/j.issn.1002-1949.2014.11.03 [9] MAKI DG, ROSENTHAL VD, SALOMAO R, et al.Impact of switching from an open a closed infusion system on rates of central line-associated bloodstream infection:a meta-analysis of time-sequence cohort studies in 4 countries[J].Infect Control Hosp Epidemiol, 2011, 32(1):50. doi: 10.1086/657632 [10] LAI TS, WANG CY, PAN SC, et al.Risk of developing severe sepsis after acute kidney injury:a population-based cohort study[J].Crit Care, 2013, 17(5):R231. doi: 10.1186/cc13054 [11] 中华医学会重症医学分会.中国严重脓毒症/脓毒性休克治疗指南(2014)[J].中华内科杂志, 2015, 54(6):557. [12] SAFAEI ASL A, DADASHZADEH P.Acute kidney injury in patients with paraquat intoxication; a case report and review of the literature[J].J Renal Inj Prev, 2016, 5(4):203. doi: 10.15171/jrip.2016.43 [13] 罗苑苑, 林新峰, 岳金芳, 等.从p38MAPK途径探讨参附注射液对脓毒症大鼠心功能的影响[J].广州中医药大学学报, 2017, 34(3):394. [14] HEMANDEZ G, BRUHN A, CASTRO R, et al.The holistic view on perfusion monitoring in septic shock[J].Curt Opin Crit Care, 2012, 18(3):280. doi: 10.1097/MCC.0b013e3283532c08 -




 下载:
下载: