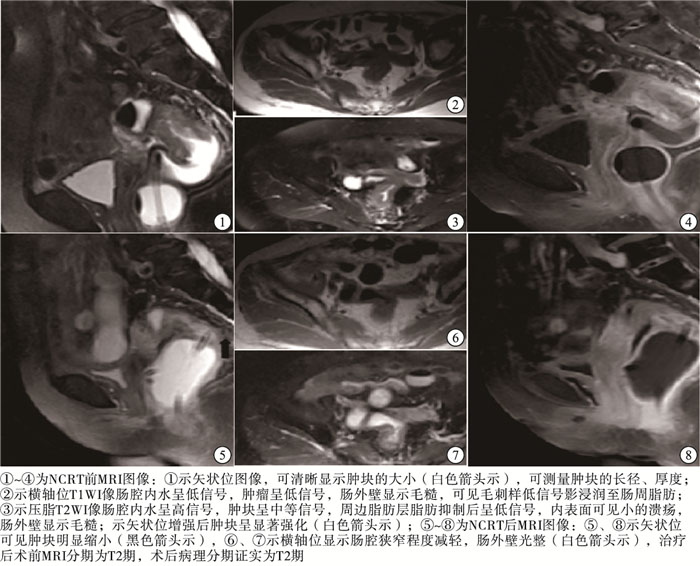
-
直肠癌是当今社会最常见的消化道恶性肿瘤之一,严重威胁人类健康。直肠癌的发病率呈逐年上升趋势[1],其发病率在女性中居第三位,在男性中居第五位[2]。为降低术后复发率、增加保肛率和延长生存寿命,临床开始对低位直肠癌以及T3、T4进展期直肠癌术前进行新辅助治疗(neoadjuvant chemoradiotherapy,NCRT)[3]。相对于传统的诊断手段,影像诊断直肠癌NCRT后T分期的准确性被看成是提升结直肠癌疗效的关键。MRI具有多方位、多参数、软组织分辨率高等特点,可以清晰显示结直肠癌癌肿及周边组织浸润情况。辅以直肠内充水,能更好地分析肿瘤的大小及T分期。本研究通过回顾分析病人NCRT前、后MRI T分期的改变及肿瘤大小的变化,评估直肠癌NCRT的疗效。
-
选择我院2013年6月至2017年6月确诊为直肠癌病人39例,均进行NCRT,术前经直肠充水后MRI扫描。男26例,女13例;年龄34~76岁;临床表现包括便血、脓血便、大便习惯改变及下腹痛等症状;均获得治疗前活检病理证实。
-
受检病人检查前空腹12 h,予以10~12 h口服导泻剂或检查前2~3 h清洁灌肠,使肠道清洁,避免肠道内粪便污染。扫描前肠道内插入双腔气囊导尿管,先充气或充水使导尿管固定,避免脱落。将150~500 mL温水注入肠腔内,使肠道适度充盈。病人平卧于扫描床,使用Siemens Novous 1.5T/philip3.0T超导磁共振扫描仪进行扫描,常规压脂T2WI矢状位扫描,确定病灶的位置,然后在此基础上进行常规横轴位T2WI及T1WI进行扫描,并注射钆喷酸葡胺进行增强扫描,剂量为0.1 mmol/kg。
-
所有确诊直肠癌病人均进行NCRT前、手术前MRI分期并与术后病理分期进行比较,依据RECIST1.1标准对肿瘤进行NCRT后疗效的评价。T分期根据直肠壁及周边受侵情况,参照美国癌症联合会第七版直肠癌T分期标准[4]:T1,肿瘤穿透黏膜至黏膜下层;T2,肿瘤穿透黏膜层侵及固有肌层;T3,肿瘤侵及直肠周围脂肪层及(或)直肠系膜;T4,肿瘤侵及邻近器官或邻近腹膜。肿瘤疗效评价参考国际抗癌联盟提出的实体肿瘤的疗效评价标准(response evaluation criteria in solid tumors,RECIST)[5],测量瘤体的长径及厚度。将NCRT疗效分4个级别:(1)完全缓解(complete response,CR),所有病灶均消失;(2)部分缓解(partial response,PR),所有病灶最长径之和缩短30%以上或截面积缩小50%以上;(3)无变化(stable disease,SD),介于PR与PD之间;(4)进展(progressive disease,PD),所有病灶最长径之和增加25%以上或截面积增大25%以上,以及出现新病灶。NCRT评估总有效率(overall response rate,ORR)=(CR例数+PR例数)/总病例数×100%。由两名高年资影像诊断医生共同读片以做出MRI T分期,并与术后病理分期进行比较,评价NCRT后术前MRI分期与术后病理分期的准确性、敏感性及特异性。将NCRT前、后的肿块长径及厚度进行分析,观察肿瘤的退缩情况,依据RECIST标准评价直肠癌NCRT的疗效。
-
采用t检验和χ2检验。
-
NCRT前MRI分期为T2期4例、T3期31例、T4期4例;治疗后T1期4例、T2期25例、T3期10例;其中NCRT前、后的MRI分期降期数为29例,降期率为74.4%。NCRT前、后的MRI分期差异有统计学意义(χ2=33.96,P < 0.01)。
-
术前MRI分期:T1~2期29例,T3期10例;病理分期:T0~2期31例、T3期8例(见表 1)。39例中有5例病人病理分期为CR,但在MRI T分期中4例为T1期,1例为T2期,2例病人MRI T分期为T2和T3期,病理分期均为T1期,MRI分期为高估,3例病人MRI T分期为T3期,但病理分期为T2期,MRI分期为高估;2例病人MRI T分期为T2期,病理分期为T3期,MRI分期为低估。NCRT后术前MRI T分期符合术后病理分期为27例,MRI T分期准确率69.2%(27/39)。
NCRT后的MRI分期 病理T分期 T0 T1 T2 T3 合计 T0 — — — — — T1 4 0 0 0 4 T2 1 1 21 2 25 T3 0 1 3 6 10 合计 5 2 24 8 39 表 1 39例病人术前MRI分期与术后病理T分期的比较(n)
-
NCRT治疗后肿瘤长径和厚度均较治疗前明显降低(P < 0.01)(见图 1、表 2)。根据RECIST1.1标准,依据长径判断PR 21例及SD 18例,ORR为53.8%(21/39);依据厚度判断PR 21例、SD 17例及PD 1例,ORR为53.8%(21/39);2组病人疗效差异无统计学意义(χ2=1.03,P>0.05)。
分组 长径/cm 厚度/cm 治疗前 4.38±2.70 2.94±2.30 治疗后 2.34±1.44 1.54±0.94 t 8.06 6.12 P < 0.01 < 0.01 表 2 NCRT前、后直肠癌肿瘤长径与厚度的变化情况比较(x±s)
-
直肠癌病人术前检查主要有CT、直肠腔内超声、MRI及PET-CT等辅助检查。随着直肠癌NCRT的发展,应用可靠、有效的影像学检查方法评价NCRT的疗效成为当下影像科医师及临床医师关注的焦点。MRI具有对软组织高分辨、多方位及无电离辐射等优点,在直肠癌检查中应用广泛,对直肠癌的术前分期及经NCRT后术前再分期中的应用能满足临床对直肠癌病人分期的需求。准确合理的术前MRI T分期的准确性是判定直肠癌病人合理制定治疗方案的关键。常规的盆腔MRI检查可以观察肿瘤、肠壁及邻近组织,但由于肠道在自然状态下常常处于萎陷或不完全扩张等状态,常规检查效果往往欠佳[6]。汤永祥等[6-8]认为结直肠癌病人灌肠后经直肠充入温水或水囊后行MRI检查,可以清除肠腔内粪便等肠道内容物干扰,使肠腔扩张,肠腔内水可以与肠壁及周围组织形成天然对比,提高人工对比度,从而可提高结直肠癌病人术前分期的准确性及敏感性,有利于直肠癌的准确分期。本研究所有病人均行直肠充水后MRI检查,大部分可以清晰显示肿块的长径及厚度,肛门达肿块下缘的距离。笔者认为直肠下端及肛管区结构复杂,病变区域容易与肛周肌肉等软组织及血管相混淆,应用双腔导尿管注入水后下段病灶易被固定囊挤压变形,因此对MRI分期产生一定的影响,造成肿瘤测量及分期的困难。
-
准确的术前影像分期对临床治疗有重要指导价值。有报道[9]表明进展期直肠癌病人进行术前NCRT,能提高直肠癌病人的存活率,降低病人直肠癌术后复发及转移,部分病人可以达到CR。高分辨MRI检查因具备良好的软组织对比度,以及多功能和多方位成像能力,被推荐为直肠癌术前分期的标准成像方法[10]。研究[11]表明直肠癌MRI T分期准确性较其他影像学分期高。NCRT后的MRI检查不仅可以通过测量肿瘤的大小变化评估放化疗的效果,还可以分析肿瘤的降期预测肿瘤放化疗的疗效,所以NCRT后MRI再分期非常重要。
本研究结果显示,39例病人在NCRT后的MRI T分期中的诊断准确性为69.2%。NCRT后部分病人在MRI T分期中出现分期的高估或低估现象。直肠癌NCRT后分期准确性[12-13]较未经NCRT后准确性[14](可达90%)低,主要是由于经NCRT后肿瘤组织可出现坏死、纤维化等,病灶所在肠壁会变薄、形成溃疡、黏液湖及肠壁炎性水肿等病理改变。MEMON等[15]认为纤维化是NCRT后最常见的病理学变化,几乎见于所有病人。直肠癌经NCRT后导致肠壁水肿、肿瘤坏死及黏液湖的形成在T2WI像呈高信号影,不易与正常的肿瘤组织及肠壁组织相鉴别,经验不足者容易将水肿的肠壁误认为肿瘤。为了给临床提供可靠的个体化治疗依据,最大化地让病人在术前放化疗中获益,放射科医师需熟知结直肠癌治疗后病理变化,以提高NCRT后再分期的准确性。
-
直肠癌经NCRT后肿瘤大小大部分可呈不同程度缩小,部分病人对治疗不敏感,病灶可有一定的进展。本组数据测量病人NCRT前、后的肿块的长径及厚度,差异有统计学意义;结合RECIST1.1标准依据长径判断PR 21例,SD 18例;依据厚度判断PR 21例、SD 17例、PD 1例,其中1例病人显示厚度增加>25%,体积有所增大,2组数据均显示疗效的ORR均为53.8%。NCRT前、后MRI分期对比,降期率达74.4%(29/39)。近年来有学者提出了肿瘤退缩分级(TRG)[16]及依据RECIST1.1标准评价NCRT的疗效,任胜等[17]研究表示降期有效率为71.1%(27/38),与本研究降期率74.4%大致相符。本研究病理资料显示CR5例(12.8%),而MRI分期中并没有CR病例,与NRCT后直肠壁水肿、纤维化等治疗后病理改变等因素有关。本研究2组结果显示直肠癌经NCRT后肿瘤的退缩及降期上均有一定的预测价值,据此可以评估肿瘤的疗效。
虽然本研究无法判断治疗前的T分期的准确性,但是有学者[14]对未经NCRT直接手术的病人进行术前T分期与术后病理分期进行比较,准确率高达90%左右,MRI对直肠癌分期准确性高。借此判定本研究直肠癌治疗前的T分期,对比治疗后T分期的改变。并依据RECIST1.1标准,判定肿瘤退缩程度,从而有效评估疗效。因此,本研究在一定程度上可以作为动态观察及判断NCRT疗效的依据,还可有效判定NCRT后T分期,为手术治疗提供依据。
直肠充水后MRI检查对直肠癌新辅助治疗疗效的评估价值
Assessment value of MRI with rectal water filling in the efficacy of neoadjuvant chemoradiotherapy in rectal cancer
-
摘要:
目的探讨直肠充水后MRI检查对直肠癌新辅助治疗(neoadjuvant chemoradiotherapy,NCRT)后MRI T分期再分期的评估价值,并判断NCRT后的疗效。 方法回顾性分析2013年6月至2017年6月确诊为直肠癌病人39例,均进行NCRT,NCRT前、后均进行直肠充水后MRI检查,并将NCRT后的MRI T分期与术后病理分期进行对比分析,判断治疗后MRI检查结果的准确性。依据实体肿瘤评价的RECIST1.1标准评价直肠癌NCRT后的肿瘤退缩程度及疗效。 结果39例接受NCRT病人,其中29例病人均见不同程度降期,其降期率为74.4%;治疗后术前MRI T分期符合术后病理分期27例,其MRI诊断的总准确率为69.2%。NCRT前、后的MRI分期差异有统计学意义(P < 0.01)。治疗后肿瘤长径和厚度均明显降低(P < 0.01),根据RECIST1.1标准判断治疗的总有效率为53.8%。 结论直肠充水后MRI不仅能动态评估直肠癌NCRT前、后T分期的改变和肿瘤大小的变化,从而有效评估疗效,还可有效判定NCRT后T分期,为手术治疗提供依据。 Abstract:ObjectiveTo evaluate the value of MRI with rectal water filling in the MRI T restaging following neoadjuvant chemoradiotherapy(NCRT) in rectal cancer, and determine the efficacy of NCRT. MethodsRetrospective analysis was conducted in 39 patients with rectal cancer who were clinically diagnosed from June 2013 to June 2017, and treated with NCRT.Both before and after NCRT, MRI examination was performed after rectal water filling.The MRI stages after NCRT were compared with the postoperative pathological stages to determine the accuracy of the MRI results after treatment.Evaluation of tumor withdrawal degree and therapeutic effect after NCRT of rectal cancer based on the RECIST 1.1 standard of solid tumor evaluation. ResultsThirty-nine patients were treated with NCRT, and compared the MRI stages before and after treatment.Of these, Twenty-nine patients had different descending stages, and their descending rate was 74.4%.There were 27 cases of postoperative pathological staging with MRI staging before and after the treatment, and the overall accuracy of MRI diagnosis was 69.2%.The MRI staging before and after NCRT was statistically significant(P < 0.01).After treatment, the tumor length and thickness were significantly reduced(P < 0.01) The overall response rate for judging the therapeutic effect of tumors according to the RECIST 1.1 standard was 53.8%. ConclusionsMRI with rectal water filling can not only dynamically evaluate the changes of T staging before and after NCRT of rectal cancer and the changes of tumor size to effectively evaluate the efficacy, but also effectively determine the NCRT T staging, which can provide basis for surgical treatment. -
表 1 39例病人术前MRI分期与术后病理T分期的比较(n)
NCRT后的MRI分期 病理T分期 T0 T1 T2 T3 合计 T0 — — — — — T1 4 0 0 0 4 T2 1 1 21 2 25 T3 0 1 3 6 10 合计 5 2 24 8 39 表 2 NCRT前、后直肠癌肿瘤长径与厚度的变化情况比较(x±s)
分组 长径/cm 厚度/cm 治疗前 4.38±2.70 2.94±2.30 治疗后 2.34±1.44 1.54±0.94 t 8.06 6.12 P < 0.01 < 0.01 -
[1] 周总光, 王自强.欧美与日本中低位直肠癌诊治指南解读[J].中国实用外科杂志, 2009, 29(4):291. doi: 10.3321/j.issn:1005-2208.2009.04.004 [2] 陈万青, 张思维, 曾红梅, 等.中国2010年恶性肿瘤发病与死亡[J].中国肿瘤, 2014, 23(1):1. [3] PARK IJ, KIM JY, YU CS, et al.Preoperotive chemoradiotherapy for clinically diagnosed T3N0 rectal cancer[J].Surg Today, 2016, 46(1):90. doi: 10.1007/s00595-015-1136-0 [4] EDGE SB, COMPTON CC.The American joint committee on cancer:The 7th edition of the ajcc cancer staging manual and the future of T[J].Annals Surgi Oncol, 2010, 17(6):1471. doi: 10.1245/s10434-010-0985-4 [5] EISENHAUER EA, THERASSE P, BOGAERTS J, et al.New response evaluation criteria in solid tumours:Revised RECIST guideline (version 1.1)[J].Eur J Cancer, 2009, 45(2):228. doi: 10.1016/j.ejca.2008.10.026 [6] 李正军, 陈井亚, 祝新, 等.直肠腔内置入水囊后MRI检查对直肠癌术前分期的诊断价值[J].中国CT和MRI杂志, 2017, 15(2):102. doi: 10.3969/j.issn.1672-5131.2017.02.032 [7] 汤永祥, 张金平.直肠充水磁共振成像在直肠癌诊断及术前分期中的应用[J].蚌埠医学院学报, 2013, 38(4):461. doi: 10.3969/j.issn.1000-2200.2013.04.031 [8] ACAY MB, BAYRAMOGLU S, ACAY A.The sensitivity of mr colonography using dark lumen technique for detection of colonic lesions[J].Turk J Gastroenterol, 2014, 25(3):271. doi: 10.5152/tjg.2014.4850 [9] 梁承友, 李平, 罗毅, 等.新辅助化疗在结直肠癌中的应用(附62例报告)[J].现代肿瘤医学, 2014, 22(6):1381. doi: 10.3969/j.issn.1672-4992.2014.06.46 [10] TAPAN U, OZBAYRAK M, TATLI S.MRI in local staging of rectal cancer:an update[J].Diagn Interv Radiol, 2014, 20(5):390. doi: 10.5152/dir.2014.13265 [11] 唐娜, 尚乃舰, 张红霞.3.0T高分辨率MRI在直肠癌术前T分期中的价值[J].中国临床医学影像杂志, 2016, 27(8):562. [12] VAN DER PAARDT MP, ZAGERS MB, BEETS-TAN RG, et al.Patients who undergo preoperative chemoradiotherapy for locally advanced rectal cancer restaged by using diagnostic MR imaging:a systematic review and meta-analysis[J].Radiology, 2013, 269(1):101. doi: 10.1148/radiol.13122833 [13] LEE JH, JANG HS, KIM J, et al.Prediction of pathologic staging with magnetic resonance imaging after preoperative chemoradiotherapy in rectal cancer:pooled analysis of KROG 10-01 and 11-02[J].RT Oncol, 2014, 113(1):18. [14] ZHANG G, CAI YZ, XU GH.Diagnostic accuracy of MRI for assessment of T category and circumferential resection margin involvement in patients with rectal cancer:a meta-analysis[J].Dis Colon Rectum, 2016, 59(8):789. doi: 10.1097/DCR.0000000000000611 [15] MEMON S, LYNCH AC, BRESSEL M, et al.Systematic review and meta-analysis of the accuracy of MRI and ERUS in the restaging and response assessment of rectal cancer following neoadjuvant therapy[J].Colorectal Dis, 2015, 17(9):748. doi: 10.1111/codi.12976 [16] RYAN R, GIBBONS D, HYLAND JMP, et al.Pathological response following long-course neoadjuvant chemoradiotherapy for locally advanced rectal cancer[J].Histopathology, 2005, 47(2):141. doi: 10.1111/j.1365-2559.2005.02176.x [17] 任胜, 孙振强, 王海江.MRI和MSCT对进展期直肠癌新辅助疗效评估价值对比研究[J].中华肿瘤防治杂志, 2017, 24(5):337. -




 下载:
下载: