-
Pilon骨折定义为胫骨远端1/3并且累及干骺端和胫距关节面的骨折,发病率约占下肢骨折的1%,胫骨远端骨折的7%。Pilon骨折多为高能量损伤,且因胫骨远端软组织覆盖较少,术后容易发生如切口坏死感染、内固定物外露等严重并发症[1],故如何更好的治疗Pilon骨折得到了外科医生的广泛关注。Pilon骨折的治疗方法多种多样,包括保守治疗和手术治疗等,手术治疗方法包括外固定架、髓内钉、接骨板等,均各有其优缺点,因此对于Pilon骨折,哪种治疗方法更好,并未达成共识。关于Pilon骨折的手术入路的选择,传统的内外侧双切口仍然是主流,但随着对Pilon骨折的进一步的研究认识和胫骨前外侧钢板的研究应用,胫前外侧入路逐渐被广大学者认识和研究[2],胫前外侧入路的优势在于:(1)可以很好的暴露胫骨的下关节面,特别是下胫腓联合、前踝及关节面的前外侧的Chaput骨块,能够在直视下复位关节面,利于骨折的复位;(2)前外侧入路可更好的保护软组织,减少软组织剥离,同时降低腓浅神经损伤的可能性[3];(3)单一切口同时处理胫骨和腓骨骨折,简化了手术流程。但目前Pilon骨折前外侧入路的研究仍相对较少。基于此优势,我们连续对28例Pilon骨折病人分别采用前外侧入路及内外侧入路治疗,对比分析胫前外侧入路与内外侧入路治疗Pilon骨折的手术相关指标、疗效及安全性等。
-
选取2015年1月至2018年10月我科收治的Pilon骨折病人共28例,其中男18例,女10例,年龄24~63岁。纳入标准:(1)根据其受伤机制和关节面的主要损伤部位为外翻型的Pilon骨折;(2)年龄18~65岁。排除标准:(1)合并精神障碍、严重心脑血管疾病等;(2)Gustilo ⅢA以上严重开放性骨折、骨筋膜室综合征或合并其他部位骨折者;(3)病理性骨折或二次骨折者;(4)关节面内侧严重粉碎塌陷的Pilon骨折。
将28例病人随机分为胫前外侧入路组(A组)与传统内外侧入路(B组),各14例。A组中男8例,女6例,年龄30~62岁;其中交通伤10例,高处坠落伤3例,运动相关损伤1例;3例为开放性骨折,余为闭合性骨折,但均存在不同程度软组织损伤;开放性骨折中,2例为Gustilo Ⅱ型,1例为Gustilo ⅢA型,均入院后急诊予以清创缝合术;骨折AO分型:AO/OTA43-C2型4例,AO/OTA43-C3型10例;Ruedi-Allgower分型:Ⅱ型5例,Ⅲ型9例。B组中男10例,女4例,年龄24~63岁;其中交通伤8例,高处坠落伤4例,运动相关损伤2例;2例为开放性骨折,余为闭合性骨折,但均存在不同程度软组织损伤;开放性骨折中,1例为Gustilo Ⅱ型,1例为Gustilo ⅢA型,均入院后急诊予以清创缝合术;骨折AO分型:AO/OTA43-C2型3例,AO/OTA43-C3型11例;Ruedi-Allgower分型:Ⅱ型4例,Ⅲ型10例。2组病人年龄、性别、受伤机制及分型等一般资料差异均无统计学意义(P>0.05),具有可比性。
28例病人中26例均及时行跟骨牵引以尽可能恢复患肢长度[3]、促进骨折稳定以早期消肿,2例开放性骨折行跨关节外固定架固定。受伤至就诊入院时间为1~18 h,入院至手术治疗时间为7~15 d。
-
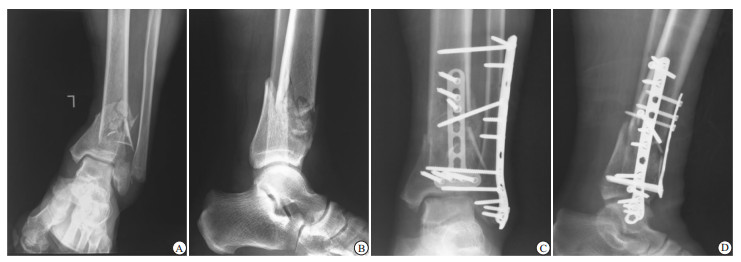
2组病人均由同一组医生所完成。A组:麻醉方法选择腰硬联合麻醉或全麻,取仰卧位,予以适度垫高患肢。切口选择时,平行于腓骨前缘,远端走向第4跖骨基底,近端根据胫骨干骺端的骨折受累长度,呈类“L”的弧形。合并腓骨骨折者首先行腓骨远端骨折的复位与固定,向后沿深筋膜暴露骨折端,通过手法牵引及钳夹复位骨折,根据骨折位置及粉碎程度选择锁定解剖接骨板或重建接骨板固定。恢复腓骨正常的力线与长度后,予以复位胫骨远端骨折。予腓骨上缘切开伸肌上支持带,使用Hoffman拉钩将胫前软组织包括血管、神经等向内牵开,显露胫骨远端前及前外侧面,游离时应保存全层皮瓣再分离皮下组织,注意保护骨膜。暴露充分后予以复位胫骨骨折块,注意内踝、后踝及前外侧骨块,内踝、后踝骨块必要时可予以克氏针辅助闭合复位、加压螺钉或克氏针固定。予以“L”形胫骨远端前外侧锁定解剖接骨板固定。若干骺端缺损严重,必要时可予以植骨,可采用自体髂骨或同种异体骨。本研究中共6例病人术中取髂骨植骨。注意相关软组织的修复,如伸肌上支持带、下胫腓前韧带等,通过C臂机透视以确认骨折复位及内固定物位置满意后,大量0.9%氯化钠溶液冲洗,置负压引流管后关闭伤口。典型病例术前及术后X-Ray见图 1。
B组:合并腓骨骨折者首先行腓骨远端骨折的复位与固定,取后外侧切口,复位骨折后采用锁定解剖接骨板或重建接骨板固定。再与外侧切口间距>7 cm,于踝关节前内侧作长4~5 cm弧形切口,暴露关节面。复位骨折,采用克氏针辅助复位及临时固定后,经皮插入合适长度的LCP接骨板,再予接骨板近端切口拧入锁钉,远近端各拧入3~4枚双皮质螺钉固定。余步骤同A组。
-
术后根据骨折端稳定情况予以1~3周的支具外固定。外固定期间嘱其加强足趾及余关节功能锻炼。抬高患肢,予以抗凝、消肿等对症支持治疗。拆除外固定后,嘱其加强踝关节的主被动功能锻炼。术后第1、2、3、4、6、12个月进行随访,此后必要时每年随访1次。行X线检查及指导病人康复锻炼。要求病人至少3个月内避免负重,3个月后根据X线片及查体情况决定患肢负重时间。
-
详细记录病人切口长度、手术时间、术中出血量、术后引流量,骨折复位情况应用Burwell-Charnley影像学评估标准评定。随访时记录病人骨折愈合时间,疗效评估以末次随访踝关节功能情况为准,踝关节功能采用Tornetta提出的Pilon骨折临床疗效评价标准及Barid-Jackson评分法进行功能评价:Pilon骨折临床疗效评价标准包括关节疼痛情况、屈伸角度及内外翻角度,分为优、良、可、差;Barid-Jackson评分法总分为95分,分数越高表示踝关节功能越好。并对比2组病人术后并发症发生情况。
-
采用t(或t′)检验和χ2检验。
-
2组病人解剖复位率、手术时间、骨折愈合时间差异均无统计学意义(P>0.05)。A组切口长度明显短于B组,术中出血量、术后引流量均明显低于B组,(P < 0.01)(见表 1、2)。
分组 n 解剖复位 复位一般 复位差 解剖复位率/% χ2 P A组 14 9 5 0 64.3 B组 14 6 7 1 42.9 1.29 >0.05 合计 28 15 12 1 53.6 表 1 2组病人骨折复位情况比较
分组 n 切口长度/cm 手术时间/min 术中出血/mL 术后引流量/mL 骨折愈合时间/周 A组 14 11.2±1.5 70.5±19.3 82.1±15.5 130.1±15.4 15.5±1.8 B组 14 20.6±4.6 74.4±21.4 105.3±16.8 180.3±20.6 16.2±2.0 t — 7.27* 0.51 3.80 7.30 0.97 P — <0.01 >0.05 <0.01 <0.01 >0.05 *示t′值 表 2 2组病人手术情况及骨折愈合情况比较(x±s)
-
28例病人随诊4~18(7.5±1.7)个月,骨折均获得愈合,其中A组发生术后切口感染1例,关节强直1例;B组发生切口感染5例,创伤性关节炎1例。2组病人关节功能优良率及并发症发生率差异均无统计学意义(P>0.05)。A组病人Barid-Jackson评分明显高于B组,差异有统计学意义(P < 0.01)(见表 3)。
分组 n 关节功能 Barid-Jackson评分(x±s) 术后并发症[n(%)] 优 良 可 差 优良率/% A组 14 7 5 2 0 85.7 91.64±1.10 2(14.2) B组 14 6 4 3 1 71.4 85.59±2.24 6(42.8) χ2 — — — — — 0.85 9.07* 1.58 P — — — — — >0.05 <0.01 >0.05 *示t′值 表 3 2组病人临床疗效及并发症发生情况比较
-
胫前外侧入路与内外侧联合入路相比,因其仅为单切口治疗Pilon骨折,故其切口长度、术中出血、术后引流量均明显低于内外侧联合入路。我们采用Tornetta提出的Pilon骨折临床疗效评价标准进行随访过程中的踝关节功能评价。此评价标准主要从疼痛、踝关节活动范围和成角畸形等三方面来评估疗效[4]。胫前外侧入路组关节功能优良率为85.7%,高于内外侧联合入路组,说明胫前外侧入路组治疗Pilon骨折有助于病人术后踝关节功能的恢复。Pilon骨折治疗并发症较多,前内侧和后外侧联合入路操作时需要广泛的剥离骨膜[5],因此会增加骨折端血运的破坏,影响骨折周围软组织的修复和骨折的愈合,再加上内固定物的使用,更容易导致术后伤口的感染坏死、内固定物的暴露等[6]。众多学者均报道了与Pilon骨折手术治疗相关的较高的软组织并发症发生。BEAR等[7]评估了Pilon骨折手术治疗软组织并发症的发生率较高,其中包括伤口破裂、深部软组织感染、骨髓炎及浅表伤口感染等。而胫骨远端的前外侧区域具有更好的软组织覆盖,且能够直接暴露前外侧关节面,可有效减少术后并发症的发生。本研究中,14例病人予以胫前外侧入路治疗后,所有病人骨折均获愈合,术后无严重的骨髓炎等并发症发生,仅发生术后切口感染1例,关节强直1例,较联合入路明显减少,说明了胫前外侧入路在减少术后并发症上的优势。
然而,本研究中经胫前外侧入路也有术中并发症发生,包括腓浅神经损伤、胫前血管损伤等。胫前外侧切口容易损伤发自腓肠神经及腓浅神经的踝支,腓浅神经于小腿下端分为2支,且时有变异,故有损伤腓浅神经的可能,损伤后病人感觉、运动差异较大。故行此切口时,首先要明确腓浅神经解剖层次,若术中发现腓浅神经横跨外踝,予以游离神经,橡皮条牵引保护,切勿过度或暴力牵拉,在神经周边应尽量少用电刀及电凝,在充分保护神经的前提下复位固定骨折。若发现有神经损伤,应立即予以修复神经。
胫前外侧入路被称为是踝关节的万能入路,指其可较大范围显露踝关节。胫骨远端皮肤血运主要分为三区,包括胫前、胫后和腓动脉区,胫前外侧入路切口位于胫骨嵴与腓骨之间,故位于胫前动脉与腓动脉供养区之间,其皮瓣坏死概率较低。入路走行于腓骨肌与第3腓骨肌之间,其向外剥离可有效显露腓骨远端,进而易于复位、固定腓骨骨折,向内剥离可有效显露胫骨远端,由于该部位伸肌支持带已近于止点,故暴露时掀起支持带止点部位即可,术后无需刻意重建。为保证更好的治疗Pilon骨折,我们要注重正确的判断手术时机。在软组织水肿高峰期时行手术治疗会使伤口张力较高,缝合困难,导致坏死率和感染率大为增加[8]。为预防软组织并发症,我们建议骨折首先予以外固定促进消肿,待软组织条件允许内固定后再行手术治疗,条件包括肿胀基本消退,皮肤出现皱折等[9]。外固定方法包括跟骨骨牵引或者跨关节外固定架[10]。本研究中28例病人的平均消肿时间为7~15 d。
单一的前外侧入路对内侧关节面的显露存在弊端,故现有多数学者认为前外侧入路应严格掌握其适应证,不适用于关节面内侧严重粉碎塌陷的Pilon骨折,对于外翻型C型Pilon骨折及累及前外侧关节面的B型Pilon骨折尤为适用[11]。对于内翻型的Pilon骨折,传统的手术入路为内侧入路切开复位内固定,YENNA等[12]报道,无论Pilon骨折表现为内翻还是外翻,从生物力学角度,使用前外侧入路并固定与内侧相比没有明显差异,故前外侧入路并固定的适应症较广泛,适用于多种类型的Pilon骨折。前外侧入路可向远近端延伸,配合良好的复位技巧可使整个远端关节面获得精确复位,极内侧关节面严重粉碎除外,使用前外侧入路,配合撑开器、术中透视及闭合复位技术可以解决后方关节面骨折的问题。因此前外侧手术入路虽不能适用于全部类型的Pilon骨折,但它确实是治疗绝大多数Pilon骨折的良好选择。
总之,胫前外侧入路治疗关节面内侧严重粉碎塌陷以外类型的Pilon骨折,能很好地减少皮肤坏死及感染发生概率, 其软组织覆盖以及血供均好于传统内外侧切口并能取得满意的疗效,有效的降低了相关并发症的发生,促进了病人的康复。
经胫前外侧入路切口在治疗Pilon骨折中的应用
Application value of the anterolateral tibial approach in the treatment of Pilon fracture
-
摘要:
目的探讨经胫前外侧入路治疗Pilon骨折的临床疗效。 方法将Pilon骨折病人28例随机分为胫前外侧入路组(A组)与传统内外侧入路组(B组),每组14例。随访并分析比较病人切口长度、手术时间、术中出血量、术后引流量、骨折愈合时间、骨折复位情况、术后并发症情况、术后踝关节功能等指标以评价疗效。 结果2组病人解剖复位率、手术时间、骨折愈合时间差异均无统计学意义(P>0.05);但A组切口长度明显短于B组,术中出血、术后引流量均明显低于B组(P < 0.01)。2组病人关节功能优良率及并发症发生率差异均无统计学意义(P>0.05);但A组病人Barid-Jackson评分明显高于B组(P < 0.01)。 结论经胫前外侧入路治疗关节面内侧严重粉碎塌陷以外类型的Pilon骨折,能取得满意的疗效,优于传统内外侧入路,可促进病人尽快康复。 Abstract:ObjectiveTo evaluate the clinical effects of the anterolateral tibial approach in the treatment of Pilon fracture. MethodsA total of 28 patients with Pilon fracture were randomly divided into the anterior lateral approach group(group A) and traditional medial approach group(group B)(14 cases each group).The incision length, operation time, intraoperative blood loss, postoperative drainage, fracture healing time, fracture reduction, postoperative complications and postoperative ankle function between two groups were compared. ResultsThe differences of the anatomical reduction rate, operation time and fracture healing time between two groups were not statistically significant(P>0.05).The incision length in group A was significantly shorter than that in group B, and the intraoperative bleeding and postoperative drainage volume in group A were significantly lower than those in group B(P < 0.01).The differences of the excellent rate of joint function and incidence rate of complications between two groups were not statistically significant(P>0.05).The Barid-Jackson score in group A was significantly higher than that in group B(P < 0.01). ConclusionsThe anterolateral tibial approach in the treatment of Pilon fracture except to severe crushing and collapse of the inner side of the articular surface can achieve satisfactory efficacy and promote the patients to recover as soon as possible, which is superior to the traditional medial and lateral approach. -
Key words:
- Pilon fracture /
- approach /
- anterolateral approach /
- internal and external approach
-
表 1 2组病人骨折复位情况比较
分组 n 解剖复位 复位一般 复位差 解剖复位率/% χ2 P A组 14 9 5 0 64.3 B组 14 6 7 1 42.9 1.29 >0.05 合计 28 15 12 1 53.6 表 2 2组病人手术情况及骨折愈合情况比较(x±s)
分组 n 切口长度/cm 手术时间/min 术中出血/mL 术后引流量/mL 骨折愈合时间/周 A组 14 11.2±1.5 70.5±19.3 82.1±15.5 130.1±15.4 15.5±1.8 B组 14 20.6±4.6 74.4±21.4 105.3±16.8 180.3±20.6 16.2±2.0 t — 7.27* 0.51 3.80 7.30 0.97 P — <0.01 >0.05 <0.01 <0.01 >0.05 *示t′值 表 3 2组病人临床疗效及并发症发生情况比较
分组 n 关节功能 Barid-Jackson评分(x±s) 术后并发症[n(%)] 优 良 可 差 优良率/% A组 14 7 5 2 0 85.7 91.64±1.10 2(14.2) B组 14 6 4 3 1 71.4 85.59±2.24 6(42.8) χ2 — — — — — 0.85 9.07* 1.58 P — — — — — >0.05 <0.01 >0.05 *示t′值 -
[1] 宋哲, 张堃.胫骨pilon骨折手术治疗并发症的防治进展[J].中华创伤杂志, 2014, 30(7):658. doi: 10.3760/cma.j.issn.1001-8050.2014.07.007 [2] ANEJA A, LUO TD, LIU B, et al.Anterolateral distal tibia locking plate osteosynthesis and their ability to capture OTAC3 pilon fragments[J].Injury, 2018, 49(2):409. doi: 10.1016/j.injury.2017.12.015 [3] CHEN H, CUI X, MA B, et al.Staged procedure protocol based on the four-column concept in the treatment of AO/OTA type 43-C3.3 pilonfractures[J].J Int Med Res, 2019:0300060519836512. [4] 唐盛辉, 孙永建, 赵汉民, 等.3D打印技术辅助治疗高能量Pilon骨折的临床应用[J].中国矫形外科杂志, 2015, 23(22):2042. [5] 王朝亮, 黄素芳, 孙雪生, 等.根据受伤机制分型采用不同手术策略治疗Pilon骨折[J].足踝外科电子杂志, 2017, 4(2):12. doi: 10.3969/j.issn.2095-7793.2017.02.003 [6] LAKHOTIA D, SHARMA G, KHATRI K, et al.Minimally invasive osteosynthesis of distal tibial fractures using anterolateral locking plate:Evaluation of results and complications[J].Chin J Traumatol, 2016, 19(1):39. doi: 10.1016/j.cjtee.2015.07.010 [7] BEAR J, ROLLICK N, HELFET D.Evolution in Management of TibialPilonFractures[J].Current reviews in musculoskeletal medicine, 2018, 11(4):537. doi: 10.1007/s12178-018-9519-7 [8] 龚晓峰, 许毅博, 吕艳伟, 等.Pilon骨折手术疗效的相关因素分析[J].中华骨科杂志, 2016, 36(21):1380. doi: 10.3760/cma.j.issn.0253-2352.2016.21.007 [9] 贾光辉, 王天旭, 李兴华, 等.急诊与择期手术治疗Pilon骨折的比较[J].蚌埠医学院学报, 2013, 38(4):418. doi: 10.3969/j.issn.1000-2200.2013.04.013 [10] 钟振锋, 杜梅, 曹任胜.严重pilon骨折的手术治疗[J].中华创伤骨科杂志, 2018, 20(6):545. doi: 10.3760/cma.j.issn.1671-7600.2018.06.016 [11] 陈鹏, 赵凯, 计飞, 等.单切口钢板支撑在Pilon骨折临床运用[J].浙江创伤外科, 2017, 22(1):122. doi: 10.3969/j.issn.1009-7147.2017.01.056 [12] YENNA ZC, BHADRA AK, OJIKE NI, et al.Anterolateral and medial locking plate stiffness in distal tibial fracture model[J].Foot Ankle Int, 2011, 32(6):630. doi: 10.3113/FAI.2011.0630 -




 下载:
下载: