-
腰椎管狭窄症通常是指各种原因引起椎管、侧隐窝及椎间孔狭窄,压迫硬膜囊及神经根,从而导致相应神经功能障碍的一类疾病[1]。高位腰椎管狭窄的诊断目前没有国际统一标准,大多学者通常将T12~L1、L1~2、L2~3节段狭窄定义为高位腰椎管狭窄[2]。高位腰椎管狭窄症的发病率低,临床表现常混有股神经、坐骨神经症状及不典型腰痛,症状不典型,较容易漏诊和误诊[3]。高位腰椎管内容物多,椎管容积相对狭小,手术难度大,易误伤神经根及硬膜囊,一度被认为属于椎间孔镜手术的禁区。随着对椎间孔局部精细解剖的深入理解及内镜手术技术的不断提高,微创内镜治疗高位腰椎管狭窄症得以临床应用,逐步突破禁区,惠及病人[4]。我们应用经皮内镜椎间孔扩大成形术治疗高位腰椎管狭窄症病人8例,取得较满意效果。现作报道。
-
选取2017年3-6月我院收治的高位腰椎管狭窄症病人8例,男5例,女3例,年龄38~80岁,病程3个月至15年,均表现为不同程度腰痛伴行走后臀部及大腿疼痛,股神经支配区皮肤感觉减退,2例病人疼痛可至小腿,2例病人为急性股神经支配区疼痛,股神经牵拉试验阳性或阴性,均无马尾神经症状,单侧症状较重。经临床和影像学检查确诊为单节段高位腰椎管狭窄症,病变节段:T12~L1例、L1~2 3例、L2~3 3例。经保守治疗均无效,既往无腰椎手术史。
-
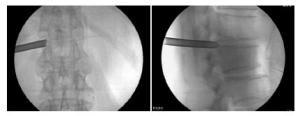
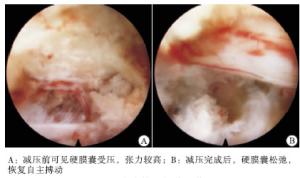
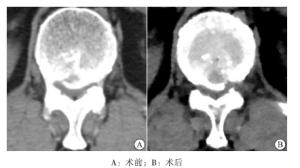
手术取俯卧位,采用0.25%利多卡因局部麻醉。高位穿刺时,易误伤肾脏及后腹膜,术前须行CT或MRI测量出最远安全皮肤进针穿刺点距离。高位节段穿刺,皮肤进针点距离中线较近,一般为6~8 cm,不超过术前所测量的最远安全距离。选择临床症状重及影像学表现压迫较重一侧穿刺,进针方向平行于间隙平面。正位透视下针尖位于椎弓根中点连线,侧位透视下针尖抵达纤维环后侧。透视无误后取约0.7 cm皮肤切口,用逐级铰刀扩大工作通道,置入工作套管。工作套管斜口方向朝向黄韧带,正位透视下斜口尖端位于椎弓根内缘连线,侧位透视下尖端位于纤维环后侧区域。放入内镜,手术完全在内窥镜直视并在持续0.9%氯化钠溶液灌注下进行。清理镜下视野,清晰暴露镜下各组织结构。稍退工作套管并尽量腹推,应用镜下动力磨钻磨除部分上关节突腹侧骨质,范围为关节突尖端至根部,直至可见硬膜囊神经根自椎间孔区膨出。再稍进工作套管,于硬膜囊神经根腹侧减压,磨除上下椎体后缘致压骨质,摘除突出间盘,减压范围起自神经根出行处,止于下椎体椎弓根上缘。减压完成后,镜下可见硬膜囊神经根松弛,并恢复自主搏动。于镜下插入一根导丝,尖端抵至硬膜囊腹侧减压最深处,确定减压范围,正位透视见导丝尖端达椎管中央。手术结束,切口缝合1针,无菌辅料包扎。
-
术后常规给予脱水剂及激素等对症治疗,术后3 d逐渐减量停用。卧床24 h后,可在腰围保护下离床活动,并持续佩戴腰围6周。所有病人于术前和出院时及术后3、6个月采用腰痛和下肢痛视觉模拟评分(VAS)、日本骨科协会评分(JOA)及腰椎Oswestry功能障碍指数(ODI)进行评价,并于末次随访时采用MacNad功能评分评价病人治疗效果。
-
采用方差分析和q检验。
-
8例病人均在局麻下顺利完成手术,术中出血量少,未予评估,无神经根及硬膜囊损伤及术后出血等并发症,手术时间90~130 min,住院时间5~9 d,切口均一期愈合。7例病人术后根性症状即消失,1例术后出现一过性腰臀部疼痛加重,经保守治疗后缓解。典型病人手术示例见图 1~3。术后随访半年,无复发病例,病人术后各时点VAS评分和ODI指数均低于术前(P<0.05~P<0.01),JOA评分均高于术前(P<0.05)(见表 1)。末次随访时按照MacNad功能评分评价8例病人疗效,优6例,良1例,可1例,优良率达87.50%。
时间 VAS评分 JOA评分 ODI指数 术前 6.86±2.80 12.13±6.89 2.88±1.25 出院时 2.25±1.16** 22.00±6.89* 1.38±0.74* 术后3个月 2.50±1.60** 20.88±6.81* 1.63±0.74* 术后6个月 3.25±1.04** 23.75±6.14* 1.75±0.71* F 11.42 4.79 4.47 P <0.01 <0.01 <0.05 MS组内 3.207 44.755 0.791 q检验:与术前比较*P<0.05,**P<0.01 表 1 病人手术前后不同时点VAS评分、JOA评分和ODI指数比较(n=8;x±s;分)
-
高位腰椎管容积相对狭小,且椎管内容物较多,部分病人脊髓圆锥可达L2水平,硬膜外脂肪很少,硬膜外间隙很小,故缓冲空间很小。而神经根临近或处于腰骶膨大,椎管内稍有致压因素,即可对硬膜囊形成明显压迫[5]。而椎管内神经结构多且复杂,高位腰椎管狭窄对组织压迫较多,出现的神经损害较重,且定位体征不明确,多为有严重的腰痛症状,范围较大。即使病人病变范围为同一节段,但病人可表现出完全不同的临床症状。多数病人于病变节段棘突间隙旁侧有局限性压痛,部分病人疼痛范围较大或无明显压痛。此外可有下腹部、腹股沟区、大腿前内侧及小腿前侧疼痛。感觉减退的范围可累及下腹部、大腿内侧或整个下肢[6]。故术前明确责任节段尤为重要。
传统开放术式须剥离脊柱后方肌肉组织并辅以内固定装置,对原有生理结构影响较大,术野内出血多,误伤硬膜囊、神经及脊髓概率高,损伤影响大,术后恢复时间长[7]。随着腰椎低位节段手术经验的积累,以及椎间孔镜手术设备及镜下器械的改进,腰椎高位节段的孔镜下减压已逐渐开展起来。
与下腰椎不同,高位腰椎管呈半圆形或近三角形,无侧隐窝结构,椎间孔区与椎管无明显分界,椎间孔可以看作是椎管结构的延续[8],椎间孔扩大成形可有效缓解椎管内压迫,释放椎管压力。磨除上关节突腹侧骨质,即可为一侧硬膜囊打开背侧部分避让空间,减低硬膜囊压力,且硬膜囊腹侧减压时可有效扩大视野,加之内镜的放大作用,可显著降低误伤硬膜囊风险[9]。相比低位腰椎,高位节段椎间孔结构上下径及前后径较大,而左右径较小,椎管与椎间孔分界不甚明显,单侧椎间孔区扩大成形后,即可有效扩大椎管容积,甚至为对侧硬膜囊打开部分避让空间。腰椎高位节段水平无行走神经根发出,但于硬膜内走行的下位出口神经根,因即将走行出椎管,活动范围小,对压迫的避让及代偿能力差,故发生椎管狭窄后,下位出口神经根首先受累,且受累程度最高[10]。下位出口神经根位于硬膜囊内最外侧,椎间孔区扩大成形后,可有效松解下位出口神经根,并缓解病人临床症状。如病人双侧症状均较重,必要时可行双侧椎间孔区扩大成形术。
此外,经皮内镜椎间孔扩大成形术在局部麻醉下进行,病人始终清醒,术中可与病人流畅沟通,进一步避免损伤硬膜囊及神经。在局部麻醉下进行手术,也为老年、心肺功能差、基础病等难以耐受全身麻醉病人提供了手术机会。该技术通过椎间孔入路途径,在内窥镜监视下操作,比通常的后路手术创伤小,对脊柱稳定性结构无破坏,无需置入内固定装置,且镜下持续灌注冲洗,术野清晰,提高了安全性。镜下直视硬膜囊,减压明确,手术疗效确切,且为微创手术,病人损伤小,恢复快。本研究结果显示,病人术后各时点VAS评分和ODI指数均低于术前,JOA评分均高于术前,末次随访时按照MacNad功能评分评价8例病人疗效,优良率达87.50%。
综上,经皮椎间孔镜下椎间孔区扩大成形术治疗高位腰椎管狭窄症具安全、有效、微创的优点。但本研究仅作半年随访观察,其长期疗效以及对病人术后腰椎活动度、稳定性、临近节段椎间盘退变是否有潜在影响,尚需循证医学的大样本研究和长时间观察。
经皮内镜椎间孔扩大成形术治疗高位腰椎管狭窄症的疗效
Effect of the expanded percutaneous endoscopic foraminal plasty in the treatment of high lumbar spinal stenosis
-
摘要:
目的探讨经皮内镜椎间孔扩大成形术治疗高位腰椎管狭窄症的临床疗效。 方法高位腰椎管狭窄症病人8例,均明确诊断为单节段高位腰椎管狭窄症,均采用经皮内镜椎间孔扩大成形术进行治疗。于术前和出院时及术后3、6个月对病人症状及腰部功能进行评价,术后6个月末次随访时采用MacNad功能评分评价病人治疗效果。 结果8例病人均在局部麻醉下顺利完成手术。病人术后各时间点的疼痛视觉模拟评分和腰椎Oswestry功能障碍指数均低于术前(P<0.05~P<0.01),日本骨科协会评分均高于术前(P<0.05)。术后随访6个月,无复发病例,末次随访时按照MacNad功能评分评价病人疗效,优6例,良1例,可1例,优良率达87.50%。 结论经皮椎间孔镜椎间孔区扩大成形术治疗高位腰椎管狭窄症安全、有效。 Abstract:ObjectiveTo evaluate the effects of the expanded percutaneous endoscopic foraminal plasty in the treatment of high lumbar spinal stenosis. MethodsEight patients with high lumbar spinal stenosis were treated with expanded percutaneous endoscopic foraminal plasty.The symptoms and waist function of the patients were evaluated before operation and after 3 and 6 months of operation.The therapeutic effects of patients was evaluated using MacNad function score at the end of 6 months after operation. ResultsEight patients were successfully operated under local anesthesia.At each time point after surgery, the visual analog score of pain and lumbar Oswestry dysfunction index(ODI) in all cases were lower than those before surgery(P<0.05 to P<0.01), and the Japanese orthopaedic association score was higher than that before surgery(P<0.05).No recurrence case was found during 6 months of following up.At the last following-up, the results of MacNad evaluation showed that the excellent in 6 cases, good 1 case and fair in 1 case were identified, and the excellent and good rate of which was 87.50%. ConclusionsThe the expanded percutaneous endoscopic foraminal plasty in the treatment of high lumbar spinal stenosis is safe and effective. -
表 1 病人手术前后不同时点VAS评分、JOA评分和ODI指数比较(n=8;x±s;分)
时间 VAS评分 JOA评分 ODI指数 术前 6.86±2.80 12.13±6.89 2.88±1.25 出院时 2.25±1.16** 22.00±6.89* 1.38±0.74* 术后3个月 2.50±1.60** 20.88±6.81* 1.63±0.74* 术后6个月 3.25±1.04** 23.75±6.14* 1.75±0.71* F 11.42 4.79 4.47 P <0.01 <0.01 <0.05 MS组内 3.207 44.755 0.791 q检验:与术前比较*P<0.05,**P<0.01 -
[1] ISSACK PS,CUNNINGHAM ME,PUMBERGER M,et al.Degenerative lumbar spinal stenosis:Evaluation and management[J].J Am Acad Orthop Surg,2012,20(8):527. doi: 10.5435/JAAOS-20-08-527 [2] REUL J.Treatment of lumbar disc herniations by interventional fluoroscopy-guided endoscopy[J].Interv Neuroradiol,2014,20(5):538. doi: 10.15274/INR-2014-10081 [3] 王德明.后路扩大减压椎体间融合治疗高位腰椎间盘突出症[J].山东医学高等专科学校学报,2018,40(3):234. doi: 10.3969/j.issn.1674-0947.2018.03.031 [4] 张西峰,张琳.脊柱内镜技术的历史、现状与发展[J].中国疼痛医学杂志,2015,21(2):81. doi: 10.3969/j.issn.1006-9852.2015.02.001 [5] 谢江,吐尔洪江·阿布都热西提,孟禅玉,等.上位腰椎不稳合并下段腰椎管狭窄后路手术治疗疗效分析[J].新疆医学,2014,44(11):26. [6] 易泽洪,肖波,杨国奇,等.后路减压经椎间孔椎间融合术治疗钙化型高位腰椎间盘突出症的临床研究[J].四川医学,2014,35(11):1427. [7] 吴俊龙,张超,周跃.微创脊柱内镜技术的发展现状与展望[J].骨科,2016,7(1):65. [8] 罗啸,黄异飞.腰椎管狭窄症的诊断与治疗现况[J].新疆医学,2015,45(10):1527. [9] 丁宇,乔晋琳,崔洪鹏,等.腰椎椎间孔镜微创手术中的区域定位原则及临床疗效观察[J].颈腰痛杂志,2015,5(36):347. [10] YEOM KS,CHOI YS.Full endoscopic contralateral transforaminal discectomy for distally migrated lumbar disc herniation[J].J Orthop Sci,2011,16(3):263. -




 下载:
下载: