-
食管癌是常见的恶性肿瘤之一,其发病率及死亡率均位于恶性肿瘤的前列[1-2]。目前食管癌的治疗方式仍以手术和放化疗为主。近年来食管癌的手术方式发展迅速,逐渐由开放手术向腔镜手术转变。胃仍然是食管癌手术中最常用的替代食管的重建器官。由于全胃代食管术后胸胃综合征、反流性食管炎、肺不张、肺部感染等并发症发生率较高,对于围术期恢复及术后生活质量造成较大影响,目前已很少应用[3]。近年来切割型管状胃已广泛应用于食管癌手术中,取得很好的临床疗效,减轻了术后胸胃综合征的发生率,改善肺功能,减轻了反流性食管炎,提高改善术后生活质量[4],缺点为影响残胃静脉回流,手术操作相对耗时、复杂、术后残胃易出血,另外高值耗材用量多,加重了病人经济负担。我们改良了管状胃的制作方法,采用非切割型管状胃替代食管,观察在开放手术中治疗食管癌的短期临床效果,探讨该术式的可行性、安全性。
-
回顾性分析2016年8月至2019年12月我院胸外科手术治疗的47例食管癌病人,分为改良管状胃组(观察组)24例,传统管状胃组(对照组)23例。其中观察组男15例,女9例,年龄(66.88±8.17)岁,肿瘤位于胸中段14例,胸下段10例;对照组男11例,女12例,年龄(63.04±9.61)岁,肿瘤位于胸中段13例,胸下段10例。手术方式均采用左进胸食管癌切除术加食管残胃胸内器械吻合。手术标准:(1)术前胃镜病理明确诊断食管癌,同时术前行上消化道造影,胸部、上腹部增强CT等检查,评估手术的可行性,评估无远处脏器及无锁骨上、右喉返神经旁、腹腔淋巴结转移;(2)术前行肺功能、血气分析、心电图、肝肾功能、血常规等检查,无明显手术禁忌证;(3)无食管、胃手术史。所有病人均签署知情同意书,具有完整的临床资料及随访资料。
-
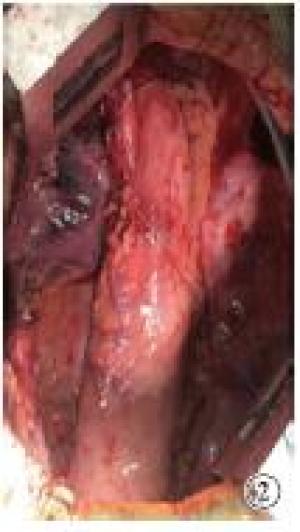
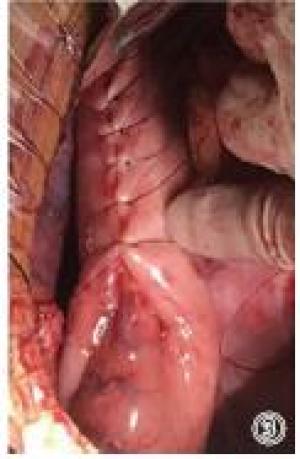
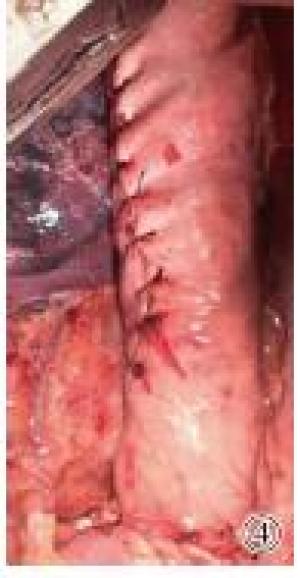
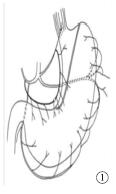
采用静吸复合麻醉,双腔气管插管,术前预置胃管、营养管至胃内。取右侧卧位,胸部垫高,左胸切口经第5或第6肋间隙逐层进胸。常规游离食管,打开膈肌游离胃,切断胃左、胃网膜左、保留胃网膜右血管。在肿瘤上方5 cm以远处做吻合位置,食管下段癌吻合口位于主动脉弓下,食管中段癌吻合口位于主动脉弓上。观察组吻合完成后,将贲门及小弯胃壁牵拉平展,用直线型切割闭合器处理贲门、胃小弯及部分胃底,切割缝合器交界及胃壁渗血处缝合加固,胃壁切缘起点及终点缝合加强后荷包包埋,间断大间距折叠浆肌层缝合包理胃壁切缘,缝合完成后残胃呈管状,管径4~5 cm。对照组在胃游离完成后吻合前制作管状胃。自胃角处离断胃右动脉,用直线型切割吻合器沿胃大弯平行方向处理,同时切除小弯侧胃壁、部分胃底及贲门后,使胃成管状,直径4~5 cm,间端缝合浆肌层,包埋小弯侧,将制作完成管状胃的上端后壁与食管行端侧器械吻合。常规清扫各组淋巴结。完成后将肠内营养管送至幽门远端15 cm左右,胃管送至管状胃中下部,并妥善固定(见图 1~4)。
-
记录2组病人手术时间、术中出血量、管状胃长度、切割缝合器使用数量、术后2 d胸腔引流总量、术后住院时间等指标;记录术后并发症的发生情况:肺部感染、吻合口瘘、残胃瘘、胸腔积液、切口感染;记录短期随访观察记录:迟发性吻合口瘘、吻合口狭窄、胸胃扩张、反流性食管炎。
-
采用t检验和χ2检验。
-
全部病人均顺利完成手术,无术中意外大出血情况等。观察组手术时间、管状胃长度与耗材用量均少于对照组的手术时间(209.17±47.19)min、管状胃长度(39.98±2.10)cm和耗材用量(3.39±0.78)个(P < 0.05~P < 0.01);2组术中出血量、术后2 d胸腔引流总量及住院时间差异均无统计学意义(P > 0.05)(见表 1)。
分组 n 手术时间/min 术中
出血量/mL管状
胃长度/cm切割缝合器
数量/个术后2 d
胸引量/mL住院时间/d 观察组 24 183.75±25.80 225.00±88.47 32.66±3.63 1.25±1.11 460.42±225.42 18.54±7.74 对照组 23 209.17±47.19 224.35±123.02 39.98±2.10 3.39±0.78 431.74±201.92 17.65±4.74 t — 2.31 0.02 8.42 7.60 0.46 0.47 P — < 0.05 > 0.05 < 0.01 < 0.01 > 0.05 > 0.05 表 1 2组病人手术观察指标比较(x ±s)
-
2组病人均未发生吻合口瘘及残胃瘘;肺部感染及胸腔积液的发生率相对于其他并发症略高,均经抗感染、引流后治愈;切口感染1例经换药后治愈。2组围术期并发症发生率差异无统计学意义(P > 0.05)(见表 2)。
分组 n 肺部
感染吻合
口瘘残胃瘘 胸腔
积液切口
感染合计
并发症χ2 P 观察组 24 4(16.67) 0(0.00) 0(0.00) 3(12.50) 1(4.17) 8(33.33) 0.17 > 0.05 对照组 23 3(13.04) 0(0.00) 0(0.00) 6(26.08) 0(0.00) 9(39.12) 合计 47 7(14.89) 0(0.00) 0(0.00) 9(19.15) 1(2.13) 17(36.17) 表 2 2组病人围术期并发症比较[n;百分率(%)]
-
2组病人短期随访并发症发生率差异无统计学意义(P > 0.05)(见表 3)。
分组 n 迟发性
吻合口瘘吻合口
狭窄胸胃
扩张反流性
食管炎合计 χ2 P 观察组 24 0(0.00) 2(8.33) 1(4.16) 3(12.49) 7(29.17) 0.51 > 0.05 对照组 23 0(0.00) 4(17.39) 0(0.00) 5(21.74) 9(39.13) 合计 47 0(0.00) 6(12.77) 1(4.35) 8(17.02) 16(34.04) 表 3 2组病人短期随访并发症比较[n;百分率(%)]
-
食管癌作为胸外科一种常见恶性肿瘤,其诊疗方式逐步多样化,但目前仍以手术和放化疗作为主要治疗手段。随着外科技术、医疗设备和器械的进步,腔镜食管癌的手术率越来越高。但由于地区经济和技术发展存在差异,各级各类医院胸外科发展情况不一,腔镜食管手术主要集中在大型医院,作为基层医院,目前仍以开放食管居多。左进胸食管癌根治对于术前评估不需要行三野淋巴结清扫的病人,仍占有很大优势,目前基层医院开展较多。术中不用更换体位,减少手术及麻醉时间;仅有胸部一个切口,术后切口感染发生率低;创伤减少,对肺功能干扰较小;胸主动脉位于左胸,暴露视野好,手术安全性高[5-6]。由于胃特有的解剖特点,消化道重建绝大部分采用胃替代食管。其优点在于胃的血供丰富,具有6条血液供应如胃左、胃右、胃短、胃后、胃网膜左及胃网膜右血管,且具有交通支;愈合能力强,浆膜、肌层及黏膜层均易愈合;可游离长度长,容积大,可塑性强,吻合重建简便等[7]。因此,左进胸胃代食管作为仍是食管癌根治术中的一种重要手术方式,目前仍具有其存在的合理性。
左进胸胸内吻合最早是由全胃替代食管进行消化道重建,手术时间短,吻合简便易推广,但随着外科技术和理念的进步,大家对全胃代食管的缺点认识越来越多。主要体现在:胸胃扩张,压迫导致肺不张,影响心肺功能;胃液反流及食管炎较重;胸胃排空障碍;特别是在吻合口瘘时,由于全胃的胃液生成多,胸内感染严重,死亡率高[8-9]。因此,现在的食管癌手术,基本淘汰了全胃代食管的手术方法。切割型管状胃由于其优点多,目前应用比较广泛。主要优点有:管状胃在解剖仿生学上与食管更加接近,对肺、心脏等周围脏器压迫轻,减少心肺功能障碍;管状胃的裁剪使胃小弯及胃大弯基本等长,吻合口与幽门成直线,不易造成排空障碍;发生吻合口瘘后,由于胃液生成的减少,降低了吻合口瘘的风险程度;塑形长度足以在颈部吻合。但其也存在不可避免的缺点:吻合口及残胃瘘的发生率仍有争议;高值耗材的使用量过高;操作步骤繁琐,手术时间长等缺点[10-13]。
我们综合研究全胃和切割型管状胃的优缺点,自2016年8月起在我院采用了非切割型管状胃替代食管进行消化道重建,与切割型管状胃进行观察比较分析后,效果满意。(1)操作简单快捷:非切割管状胃将胃完全游离后,可直接进行吻合,手术时间明显缩短,吻合完成后,用直线型切割闭合器处理贲门、胃小弯及部分胃底,间断大间距折叠浆肌层缝合包理胃壁切缘,缝合完成后残胃呈管状,制作方法较简易,长度上短于切割型管状胃,但完全能够满足弓上及胸顶吻合需要;(2)安全可靠:非切割管状胃闭合次数较管状胃大大减少,切割胃的长度大大减少,减轻了胃壁损伤,从而减少残胃出血、残胃瘘的发生率,与对照组比较,吻合口瘘及残胃瘘发生率未见明显统计学差异,考虑与目前手术技术比较成熟,手术数量较少有关;(3)术后生活质量高:非切割管状胃功能上更接近于正常胃,较好的保护了胃容纳存储功能,术后病人出现饱腹感、体质量下降等程度明显减轻;在形态上接近于食管,术后随访胸胃扩张、反流性食管炎等发生率与对照组无统计学意义,可以综合全胃和切割型管状胃的优点;(4)医疗费用控制低:避免多次切割闭合,使用75 cm切割缝合器1次可完成胃的裁剪,相比较对照组使用的数量,大大减少了手术费用给病人带来的经济负担,特别是对于基层医院的医疗费用控制具有很强的实用性[14-15]。
综上所述,非切割型管状胃适宜在食管胸中下段癌手术中应用,制作方法较简易,长度可满足弓上及胸顶吻合需要,缩短手术时间、降低耗材量,且不会增加吻合口瘘及狭窄、肺部感染、术后返酸、胸胃扩张等术后并发症,临床效果满意,适宜在基层医院推广。
改良非切割型管状胃在食管癌根治术中的应用
Application of modified uncut tubular stomach in radical resection of esophageal carcinoma
-
摘要:
目的探讨改良非切割型管状胃与传统切割型管状胃在食管癌根治术中临床应用的可行性、安全性及短期临床效果。 方法回顾性分析47例食管癌根治术病人的临床资料。所有病人术前均胃镜证实为食管癌。分为改良非切割型管状胃组24例,传统切割型管状胃组23例;分析2组病人手术时间、术中出血、管状胃长度、耗材用量及术后观察指标、出院短期随访等。 结果全部病人均顺利完成手术,无术中大出血等意外情况发生;改良非切割型管状胃组手术时间、管状胃长度与耗材用量均少于传统切割型管状胃组(P < 0.05~P < 0.01);2组术中出血、术后2 d胸腔引流总量及住院时间差异均无统计学意义(P>0.05);改良非切割型管状胃组围术期和短期随访并发症发生率与传统切割型管状胃组差异均无统计学意义(P>0.05),无严重并发症及死亡病例。 结论改良非切割型管状胃可缩短手术时间、降低耗材量,且不会增加吻合口瘘及狭窄、肺部感染、术后返酸、胸胃扩张等术后并发症。 Abstract:ObjectiveTo investigate the feasibility, safety and short-term clinical effects of the application of modified uncut tubular stomach and traditional cut tubular stomach in radical surgery of esophageal carcinoma. MethodsThe clinical data of 47 patients treated with radical surgery of esophageal carcinoma were retrospectively analyzed.All patients with esophageal cancer were confirmed by gastroscopy before surgery.The patients were divided into the modified uncut tubular stomach group(24 cases) and traditional cut tubular stomach group(23 cases).The operation time, intraoperative bleeding, length of tubular stomach, material usage, postoperative observation index and short-term follow-up after discharge in two groups were analyzed. ResultsAll operations were successfully completed, no intraoperative bleeding and other accidents occurred.The operation time, length of tubular stomach and material usage in modified uncut tubular stomach group were less than those in traditional cut tubular stomach group(P < 0.05 to P < 0.01).The differences of the intraoperative hemorrhage, postoperative 2 d thoracic drainage amount, length of hospital stay, incidence rates of complications during perioperative period and short-term follow-up between two groups were not statistically significant(P>0.05).There was no serious complication or death. ConclusionsThe modified uncut tubular stomach can shorten the operation time and reduce the material usage, and does not increase the anastomotic fistula and stenosis, pulmonary infection, postoperative acid reflux, and chest and stomach dilation. -
Key words:
- esophageal neoplasms /
- digestive tract reconstruction /
- tubular stomach
-
表 1 2组病人手术观察指标比较(x ±s)
分组 n 手术时间/min 术中
出血量/mL管状
胃长度/cm切割缝合器
数量/个术后2 d
胸引量/mL住院时间/d 观察组 24 183.75±25.80 225.00±88.47 32.66±3.63 1.25±1.11 460.42±225.42 18.54±7.74 对照组 23 209.17±47.19 224.35±123.02 39.98±2.10 3.39±0.78 431.74±201.92 17.65±4.74 t — 2.31 0.02 8.42 7.60 0.46 0.47 P — < 0.05 > 0.05 < 0.01 < 0.01 > 0.05 > 0.05 表 2 2组病人围术期并发症比较[n;百分率(%)]
分组 n 肺部
感染吻合
口瘘残胃瘘 胸腔
积液切口
感染合计
并发症χ2 P 观察组 24 4(16.67) 0(0.00) 0(0.00) 3(12.50) 1(4.17) 8(33.33) 0.17 > 0.05 对照组 23 3(13.04) 0(0.00) 0(0.00) 6(26.08) 0(0.00) 9(39.12) 合计 47 7(14.89) 0(0.00) 0(0.00) 9(19.15) 1(2.13) 17(36.17) 表 3 2组病人短期随访并发症比较[n;百分率(%)]
分组 n 迟发性
吻合口瘘吻合口
狭窄胸胃
扩张反流性
食管炎合计 χ2 P 观察组 24 0(0.00) 2(8.33) 1(4.16) 3(12.49) 7(29.17) 0.51 > 0.05 对照组 23 0(0.00) 4(17.39) 0(0.00) 5(21.74) 9(39.13) 合计 47 0(0.00) 6(12.77) 1(4.35) 8(17.02) 16(34.04) -
[1] FREDDIE B, JACQUES F, ISABELLE S, et al.Global cancer statistics 2018:GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J].CA Cancer J Clin, 2018, 68(6):394. doi: 10.3322/caac.21492 [2] ZENG RS, SUN KX, ZHANG SW, et al.Report of cancer epidemiology in China, 2015[J].Chin J Oncol, 2019, 41(1):19. [3] 陈克能.食管重建-从全胃到管胃[J].中华胃肠外科杂志, 2014, 17(9):851. [4] RAO XH, LIANG JS, ZHANG ZZ.Application of gastric tube in combined thoracoscopic-laparoscopic esophagectomy for treatment of esophageal carcinoma[J].Lingnan Modern Clin Surg, 2017, 23(6):28. [5] MA Q, LIU W, LONG H, et al.Right versus left transthoracic approach for lymph node-negative esophageal squamous cell carcinoma[J].J Cardiothorac Surg, 2015, 10:123. doi: 10.1186/s13019-015-0328-4 [6] WANG W, ZHANG B, LI X, et al.Minimally invasive esophagectomy via Sweet approach in combination with cervical mediastinoscopy for esophageal squamous cell carcinoma:a case series[J].Int J Surg Oncol(NY), 2017, 2(11):e45. doi: 10.1097/IJ9.0000000000000045 [7] CHEN KN.Managing complications I:leaks, strictures, emptying, reflux, chylothorax[J].J Thorac Dis, 2014, 6(3):S355. [8] ZHANG WX, YU DL, PENG JH, et al.Gastric-tube versus whole-stomach esophagectomy for esophageal cancer:A systematic review and meta-analysis[J].PLoS One, 2017, 12(3):e0173416. doi: 10.1371/journal.pone.0173416 [9] 韩飞, 戴天阳, 何开明, 等.改良管状胃代食管在开放手术治疗食管胸中下段癌中应用的短期效果[J].中国临床研究, 2019, 32(2):239. [10] ZHANG R, WANG P, ZHANG X, et al.Gastric tube reconstruction prevents postoperative recurrence and metastasis of esophageal cancer[J].Oncol Lett, 2016, 11(4):2507. doi: 10.3892/ol.2016.4240 [11] 喻傲, 焦子宸, 王涛.食管癌术后管状胃功能研究及应用进展[J].中国胸心血管外科临床杂志, 2019, 26(10):1032. [12] SHU YS, SUN C, SHI WP, et al.Tubular stomach or whole stomach for esophagectomy through cervico-thoraco-abdominal approach:a comparative clinical study on anastomotic leakage[J].Ir J Med Sci, 2013, 182(3):477. doi: 10.1007/s11845-013-0917-y [13] 江天, 李明, 赵梦男, 等.胃血管解剖及其在食管癌管状胃重建中的应用[J].中国肿瘤临床, 2019, 46(3):126. [14] 鲍峰, 宫为一, 于在诚.全胃代食管、缩缝胃小弯及改进管状胃代食管在食管癌术中重建消化道的效果[J].中国老年学杂志, 2017, 37(3):1452. [15] 阿曼吐尔·介恩什, 阿扎玛提·阿扎提, 伊地力斯·阿吾提.管状胃与传统缩胃手术治疗食管癌近期临床疗效对比分析[J].世界最新医学信息文摘, 2018, 18(56):17. -





 下载:
下载: