-
慢性心力衰竭(CHF)是心血管疾病常见的晚期改变,是与衰老有关的慢性疾病之一。近年来虽然CHF在治疗上有一定的进展,但其发病率及死亡率仍处于上升趋势[1]。CHF现治疗上主要从改变神经激素环境抑制交感神经兴奋、肾素-血管紧张素-醛固酮系统活性来降低心肌重构[2],从而延缓心力衰竭进展和降低死亡率。目前许多文章报道心血管疾病中的氧化应激会导致线粒体功能受损,导致心肌细胞能量供应不足,影响心肌细胞正常收缩功能,加快心力衰竭进展[3]。线粒体融合蛋白-2(Mfn2)位于线粒体外膜,能调节线粒体融合和分裂的蛋白质,所以对维持线粒体正常功能起着重要作用[4]。同样乙醛脱氢酶2(ALDH2)是能够抑制机体氧化应激,维持正常线粒体功能的关键酶,能够调节心肌细胞凋亡、纤维化来延缓心力衰竭进展[5]。临床研究中关于Mfn2、ALDH2与CHF病人的相关性研究尚不明确。本文针对Mfn2、ALDH2与CHF病人的相关性研究进行研究,为CHF的诊断及治疗探索提供参考。
-
选择2018年10月至2019年10月在我院心血管内科入院的CHF病人180例(CHF组),纳入标准:(1)所有病人均符合《中国心力衰竭诊断和治疗指南2018》;(2)所有病程≥3个月;(3)符合美国纽约心脏病协会(NYHA)分级在Ⅱ~Ⅳ级间;(4)临床资料完整。排除标准:急性ST段抬高型心肌梗死、急性创伤、肺栓塞、缩窄性心包炎、心肌炎,先天性心脏病,瓣膜性心脏病,风湿性心脏病,合并有肝、肾系统损伤、恶性肿瘤等严重原发性疾病病人。将收集的CHF病人180例按照NYHA分级标准进行分组,包括Ⅱ级46例,Ⅲ级63例,Ⅳ级71例。另外选取同期在我院门诊健康体检者40名为对照组,均无任何心血管疾病。本次研究已通过我院伦理委员会的审核。所有研究对象均对本次研究知情同意。
-
Mfn2、ALDH2水平检测均采用酶联免疫吸附法(ELISA),试剂盒(ELISA Kit-上海羽朵)。N末端B型利钠肽原(NT-proBNP)、白细胞、丙氨酸氨基转移酶、天门冬氨酸氨基转移酶、血肌酐等生化标志物和左心室射血分数(LVEF)、左心室舒张末期内径(LVEDD)分别在我院检验科和心脏超声室完成。同时收集并比较所有研究对象的一般资料,包括性别、年龄等基本情况。
-
采用t(或t′)检验、χ2检验、方差分析和q检验,Pearson相关性分析,采用受试者工作特征(ROC)曲线分析进行诊断实验的评价。
-
2组研究对象的性别、年龄、天门冬氨酸氨基转移酶、三酰甘油等生化标志比较差异均无统计学意义(P>0.05);CHF组白细胞水平高于对照组, 丙氨酸氨基转移酶和血肌酐低于对照组,差异均有统计学意义(P < 0.05~P < 0.01)(见表 1)。
分组 n 男 女 年龄/岁 白细胞/(×109/L) 丙氨酸氨基转移酶/(U/L) 天门冬氨酸转移酶/(U/L) 三酰甘油/(mmol/L) 血肌酐/(μmol /L) 对照组 40 21 19 69.50±1.59 6.98±0.28 31.13±2.06 32.90±1.42 1.48±0.12 74.28±1.81 CHF组 180 97 83 69.07±0.93 7.47±2.84 29.41±1.37 32.54±1.47 1.51±0.06 73.21±1.37 t — 0.03* 1.65* 2.27* 5.04* 1.41 1.54* 3.52* P — >0.05 >0.05 < 0.05 < 0.01 >0.05 >0.05 < 0.01 *示t′值 表 1 2组病人一般资料比较(x±s)
-
与对照组比较,Mfn2、ALDH2、LVEF在CHF组中降低,NT-proBNP、LVEDD在CHF组中增高,差异均有统计学意义(P < 0.01)。CHF心功能Ⅱ级、Ⅲ级、Ⅳ级病人组间比较,Mfn2、ALDH2随着心功能降低而降低,NT-proBNP、LVEDD逐级增高,差异均有统计学意义(P < 0.01)(见表 2)。
分组 n Mfn2/(ng/mL) ALDH2/(U/L) NT-proBNP/(pg/mL) LVEF/% LVEDD/mm 对照组 40 8.11±0.30 112.45±3.77 33.85±2.27 56.73±1.11 48.40±0.34 CHF心功能Ⅱ级组 46 6.47±0.16** 95.26±2.50** 2 724.92±632.58** 48.65±1.62** 52.41±1.50** CHF心功能Ⅲ级组 63 5.91±0.15**△△ 78.58±2.45**△△ 4 803.33±593.0**△△ 42.38±1.71**△△ 56.21±1.26**△△ CHF心功能Ⅳ级组 71 5.46±0.14**△△## 75.52±1.96**△△## 7 111.02±1 027.25**△△## 42.85±1.23**△△ 57.04±1.20*△△## F — 1 860.63 2 089.74 898.43 1 018.59 547.52 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 MS组内 — 0.034 6.836 526 280.11 2.098 1.412 q检验:与对照组比较*P < 0.05, **P < 0.01;与心功能Ⅱ级组比较△△P < 0.01;与心功能Ⅲ级组##P < 0.01 表 2 2组研究对象的血清Mfn2、ALDH2水平及相关指标比较(x±s)
-
CHF组中,LVEF≤40%病人为72例,LVEF>40%病人为108例; LVEF≤40%病人组Mfn2、ALDH2低于LVEF>40%病人,NT-proBNP、LVEDD高于LVEF>40%病人,差异均有统计学意义(P < 0.05~P < 0.01)(表 3)。
分组 n Mfn2/(ng/mL) ALDH2/(U/L) NT-proBN/(pg/mL) LVEDD/mm LVEF≤40%组 72 5.450±1.23 76.54±17.70 6 825.42±960.58 63.26±1.11 LVEF>40%组 108 6.16±1.18 85.03±19.85 4 087.11±505.82 50.44±0.67 t — 3.91 2.93 2.52 9.83 P — < 0.01 < 0.01 < 0.05 < 0.01 表 3 LVEF下降和保留的CHF病人的各项检测指标比较(x±s)
-
经Pearson相关分析,CHF组中,Mfn2与LVEDD呈负相关(P < 0.01),与LVEF呈正相关(P < 0.01),与NT-proBNP无相关性;ALDH2与LVEF呈正相关(P < 0.01),与NT-proBNP、LVEDD无相关性(见表 4)。
指标 MFN2 ALDH2 r P r P NT-proBNP -0.034 >0.05 -0.141 >0.05 LVEF 0.196 < 0.01 0.282 < 0.01 LVEDD -0.212 < 0.01 -0.124 >0.05 表 4 Mfn2、ALDH2与NT-proBNP、LVEFLVEF和LVEDD的相关性分析
-
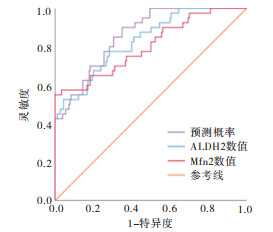
通过ROC曲线分析,ALDH2诊断CHF的ROC曲线下面积为0.831,95%CI为0.762~0.900(P < 0.05), 当ALDH2取值48.710 U/L时,敏感度为1.00,特异度为1.00。Mfn2诊断CHF的ROC曲线下面积为0.803,95%CI为0.719~0.887(P < 0.05), 当Mfn2取值2.377 ng/mL时,敏感度为1.00,特异度为1.00。将Mfn2、ALDH2两者联合起来诊断得到预测概率,其诊断CHF的ROC曲线下面积为0.891,95%CI为0.823~0.958(P < 0.05)(见图 1)。
-
CHF是一种顽固性疾病,近年来死亡率和发病率都在稳步上升,在世界范围内伴随着巨大的经济损失[6]。在心力衰竭发病机制中心肌细胞凋亡、心室重构起着至关重要的作用。目前研究机制发现心肌细胞的能量供应不足及利用障碍会使存活心肌储备减少,进一步心室收缩功能减退,进而发展或加重心力衰竭[7]。大约有三分之一的心肌细胞具有线粒体用于提供心肌收缩功能所需ATP,因此线粒体在心肌细胞生长和心肌细胞正常功能上起着至关重要的作用[7]。有研究[7]发现Mfn2、ALDH2能通过抑制氧化应激来保护线粒体,完成心肌细胞正常能量供应。此外还能通过调节自噬等方面减少细胞凋亡,以及抑制心肌重构来延缓心力衰竭进展[8-9]。本次试验中在对照组中Mfn2、ALDH2水平高于CHF组,且随着CHF心功能减退,Mfn2、ALDH2逐渐降低,所以Mfn2、ALDH2可能参与慢性心力衰竭的发生及发展。
Mfn2通过介导融合蛋白和分裂蛋白的平衡,参与线粒体形态和功能的调控,维持正常线粒体正常功能[10]。SEIDLMAYER等[1]在Mfn2基因敲除小鼠中发现其不能通过IP3介导线粒体在生理条件下维持心肌细胞ATP水平。张磊[11]在KLF9敲除的小鼠中发现Mfn2水平降低,心肌线粒体形态异常及功能也降低,不能合成足够的ATP维持心肌正常收缩功能,随着小鼠心室腔变大,心力衰竭逐渐发生。Mfn2可以通过调节AKt信号通路和Ca2+途径调节心肌细胞凋亡。当Mfn2降低时会使Akt磷酸化降低,Bcl家族中的Bax表达增多,激活capase-3促进心肌细胞凋亡,存活心肌细胞丢失逐渐导致心力衰竭发展及加重[12]。Mfn2还参与介导Ca2+从线粒体外膜释放到细胞基质过程,当Mfn2表达缺陷可引起Ca2+转运异常来促进心肌细胞凋亡[13]。HU等[14]对糖尿病心肌病的小鼠进行Mfn2的重组发现心功能LVEF和左心室缩短率的增加。同样在心肌重构方面,YU等[15]在体外培养的心肌细胞经血管紧张素Ⅱ (Ang Ⅱ)处理后,Mfn2基因表达受到抑制,会使心肌肥厚和蛋白质合成增加,从而加重心肌重构发生。本次研究中我们发现随着心功能分级增加,Mfn2水平逐步降低,特别在心功能Ⅱ级与Ⅳ级之间有统计学意义(P < 0.05)。在CHF中随着LVEF降低,Mfn2水平也减少,且Mfn2与LVEDD呈负相关,与LVEF呈正相关。Mfn2在延缓心力衰竭进展可能起到积极作用,但在维持线粒体正常功能、减少心肌细胞凋亡等方面作用仍需进一步论证。
ALDH2是一种非细胞色素P450线粒体醛氧化酶[16],能够抑制氧化应激时活性氧(ROS)的生成,以及对氧化应激时的产物醛有解毒作用,减少对线粒体损害,维持线粒体正常形态和能量供应[17]。谷小雨[18]用体外培养心室肌细胞在ALDH2激动剂剂组中发现ROS释放水平及细胞凋亡率均明显降低,证实ALDH2在减少心肌细胞凋亡中有保护意义。此外ALDH2也通过调节自噬功能,自噬心肌细胞凋亡时产生的异常蛋白的沉积,减轻心室壁僵硬度,减轻心肌纤维化,维持心室正常弹性力和收缩功能[19]。LI等[3]在ALDH2敲除的小鼠中发现心肌纤维化和心功能障碍加重,同时在8周时LVEF低于正常值。ALDH2在调节线粒体功能外,还可增强心肌细胞对内质网应激诱导的细胞毒性和凋亡的抵抗,减少细胞凋亡[20]。胡艺川[21]在使用ALDH2抑制发现心肌细胞ROS水平的增加,同时诱导的丝裂原活化蛋白激酶(MAPK)信号转导途径的活化,促进心肌细胞凋亡。在心肌重构方面,ALDH2可通过P38MAP通路降低心脏局部AngⅡ水平来减轻心肌细胞重构,保障正常心肌收缩功能[22]。正如HUA等[17]用ALDH2激动剂处理心肌梗死后的CHF大鼠中发现能够明显提高心脏LVEF值。本次研究发现在对照组中ALDH2高于CHF组,且随着CHF心功能减退,ALDH2水平逐渐降低。在LVEF≤40%的CHF组中ALDH2水平低于LVEF>40%,且与LVEF呈正相关。说明ALDH2在心力衰竭进展可能起到积极保护意义,特别在抑制氧化应激来减少心肌细胞凋亡方面有独特的价值,但需要今后更多临床实践论证。
目前在心力衰竭诊断方面,BNP及NT-proBNP从心脏压力负荷方面反应心力衰竭严重程度及预后评估指标,同时可溶性ST2、半乳糖凝集素3从心肌纤维化、炎症方面反映心力衰竭程度[23]。本次研究中ALDH2、Mfn2诊断CHF的ROC曲线下面积均>0.8,ALDH2、Mfn2与CHF的发生及发展有一定关系,故ALDH2、Mfn2可从氧化应激、细胞凋亡方面对CHF进行诊断及预后评估。
综上所述,本次实验中血清Mfn2、ALDH2水平在CHF病人中降低,并随着心功能减退而减低,说明Mfn2、ALDH2在CHF发生及发展中可能发挥一定保护作用。虽目前有研究指出Mfn2、ALDH2可通过调节线粒体功能受损、减少心肌细胞凋亡、抑制心肌细胞肥厚等方面延缓心力衰竭进展,但具体作用机制仍需大量临床实验。
血清线粒体融合蛋白-2和乙醛脱氢酶2与慢性心力衰竭的相关性研究
Study on the correlation between serum levels of mitochondrial fusion protein-2, acetaldehyde dehydrogenase 2 and chronic heart failure
-
摘要:
目的探讨线粒体融合蛋白-2(Mfn2)、乙醛脱氢酶2(ALDH2)与慢性心力衰竭(CHF)病人的相关性研究。 方法入选CHF病人180例和健康体检人(对照组)40名。其中CHF病人按NYHA心功能分级标准将病人分为Ⅱ级46例、Ⅲ级63例、Ⅳ级71例。入院后完善NT-proBNP、心脏彩超等结果,并留取血清检测Mfn2、ALDH2水平,分析Mfn2、ALDH2与CHF病人相关性。 结果与对照组比较,Mfn2、ALDH2、LVEF在CHF组中降低,NT-proBNP、LVEDD在CHF组中增高,差异均有统计学意义(P 0.01)。CHF心功能Ⅱ级、Ⅲ级、Ⅳ级病人组间比较,Mfn2、ALDH2随着心功能降低而降低,NT-proBNP、LVEDD逐级增高,差异均有统计学意义(P < 0.01)。按照左心室射血分数(LVEF)分级发现,LVEF≤40%病人组Mfn2、ALDH2低于LVEF>40%病人,NT-proBNP、LVEDD高于LVEF>40%病人,差异均有统计学意义(P < 0.05~P < 0.01);经Pearson相关分析,CHF组中,Mfn2与LVEDD呈负相关关系(P < 0.01),与LVEF呈正相关关系(P < 0.01),ALDH2与LVEF呈正相关关系(P < 0.01);与进一步分析Mfn2、ALDH2以及联合诊断CHF的受试者工作特征曲线下面积分别为0.803、0.831、0.891(P < 0.05)。 结论CHF病人随着心功能减退,血清中的Mfn2、ALDH2水平随着减低;Mfn2、ALDH2与CHF相关指标具有相关性,从而对临床评估病情及诊断可能有重要作用。 Abstract:ObjectiveTo investigate the correlation between the levels of mitochondrial fusion protein-2(Mfn2), acetaldehyde dehydrogenase 2(ALDH2) and chronic heart failure(CHF). MethodsOne hundred and eighty CHF patients and 40 healthy people(control group) were investigated.According to the NYHA heart function classification standard, the CHF patients were divided into the class Ⅱ in 46 cases, class Ⅲ in 63 cases and class Ⅳ in 71 cases.After admission, the results of NT-proBNP and cardiac color Doppler ultrasound were improved, the serum levels of Mfn2 and ALDH2 were detected, and the correlation between Mfn2, ALDH2 and CHF was analyzed. ResultsCompared with the control group, the serum levels of Mfn2, ALDH2 and LVEF decreased, the serum levels of NT-proBNP and LVEDD increased in the CHF group, and the differences of which were statistically significant(P < 0.01).Among the class Ⅱ, Ⅲ and Ⅳ heart function groups, the serum levels of Mfn2 and ALDH2 decreased with the decreasing of heart function, the serum levels of NT-proBNP and LVEDD increased with the increasing of heart function, and the differences of which were statistically significant(P < 0.01).According to the LVEF classification, the serum levels of Mfn2 and ALDH2 in patients with LVEF ≤ 40% were lower than those in patents with LVEF>40%, and the levels of NT-proBNP and LVED in patients with LVEF ≤ 40% were higher than those in patents with LVEF>40%(P < 0.05 to P < 0.01).The results of Pearson correlation analysis showed that the level of Mfn2 was negatively correlated with LVEDD(P < 0.01), and positively correlated with LVEF(P < 0.01), while the level of ALDH2 was positively correlated with LVEF(P < 0.01).The area under ROC curve of Mfn2, ALDH2 and both combination in the diagnosis of CHF were 0.803, 0.831 and 0.891(P < 0.05). ConclusionsWith the decreasing of cardiac function in CHF patients, the serum levels of Mfn2 and ALDH2 decrease.The Serum levels of Mfn2, ALDH2 are related to the CHF, which may play an important role in clinical assessment and diagnosis. -
表 1 2组病人一般资料比较(x±s)
分组 n 男 女 年龄/岁 白细胞/(×109/L) 丙氨酸氨基转移酶/(U/L) 天门冬氨酸转移酶/(U/L) 三酰甘油/(mmol/L) 血肌酐/(μmol /L) 对照组 40 21 19 69.50±1.59 6.98±0.28 31.13±2.06 32.90±1.42 1.48±0.12 74.28±1.81 CHF组 180 97 83 69.07±0.93 7.47±2.84 29.41±1.37 32.54±1.47 1.51±0.06 73.21±1.37 t — 0.03* 1.65* 2.27* 5.04* 1.41 1.54* 3.52* P — >0.05 >0.05 < 0.05 < 0.01 >0.05 >0.05 < 0.01 *示t′值 表 2 2组研究对象的血清Mfn2、ALDH2水平及相关指标比较(x±s)
分组 n Mfn2/(ng/mL) ALDH2/(U/L) NT-proBNP/(pg/mL) LVEF/% LVEDD/mm 对照组 40 8.11±0.30 112.45±3.77 33.85±2.27 56.73±1.11 48.40±0.34 CHF心功能Ⅱ级组 46 6.47±0.16** 95.26±2.50** 2 724.92±632.58** 48.65±1.62** 52.41±1.50** CHF心功能Ⅲ级组 63 5.91±0.15**△△ 78.58±2.45**△△ 4 803.33±593.0**△△ 42.38±1.71**△△ 56.21±1.26**△△ CHF心功能Ⅳ级组 71 5.46±0.14**△△## 75.52±1.96**△△## 7 111.02±1 027.25**△△## 42.85±1.23**△△ 57.04±1.20*△△## F — 1 860.63 2 089.74 898.43 1 018.59 547.52 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 MS组内 — 0.034 6.836 526 280.11 2.098 1.412 q检验:与对照组比较*P < 0.05, **P < 0.01;与心功能Ⅱ级组比较△△P < 0.01;与心功能Ⅲ级组##P < 0.01 表 3 LVEF下降和保留的CHF病人的各项检测指标比较(x±s)
分组 n Mfn2/(ng/mL) ALDH2/(U/L) NT-proBN/(pg/mL) LVEDD/mm LVEF≤40%组 72 5.450±1.23 76.54±17.70 6 825.42±960.58 63.26±1.11 LVEF>40%组 108 6.16±1.18 85.03±19.85 4 087.11±505.82 50.44±0.67 t — 3.91 2.93 2.52 9.83 P — < 0.01 < 0.01 < 0.05 < 0.01 表 4 Mfn2、ALDH2与NT-proBNP、LVEFLVEF和LVEDD的相关性分析
指标 MFN2 ALDH2 r P r P NT-proBNP -0.034 >0.05 -0.141 >0.05 LVEF 0.196 < 0.01 0.282 < 0.01 LVEDD -0.212 < 0.01 -0.124 >0.05 -
[1] SEIDLMAYER LK, MAGES C, BERBNER A, et al. Mitofusin 2 Is Essential for IP-Mediated SR/Mitochondria Metabolic Feedback in Ventricular Myocytes[J]. Front Physiol, 2019, 10: 733. doi: 10.3389/fphys.2019.00733 [2] 中华医学会心血管病学分会心力衰竭学组, 中国医师协会心力衰竭专业委员会, 中华心血管病杂志编辑委员会. 中国心力衰竭诊断和治疗指南2018[J]. 中华心血管病杂志, 2018, 46(10): 760. [3] 唐碧, 康品方, 郭建路, 等. 线粒体ALDH2对高糖处理的乳鼠心肌成纤维细胞中自噬相关蛋白影响[J]. 南方医科大学学报, 2019, 39(5): 523. [4] CHEN L, GONG Q, STICE JP, et al. Mitochondrial OPA1, apoptosis, and heart failure[J]. Cardiovasc Res, 2009, 84(1): 91. doi: 10.1093/cvr/cvp181 [5] LI X, WENG X, SHI H, et al. Acetaldehyde dehydrogenase 2 deficiency exacerbates cardiac fibrosis by promoting mobilization and homing of bone marrow fibroblast progenitor cells[J]. J Mol Cell Cardiol, 2019, 137: 107. doi: 10.1016/j.yjmcc.2019.10.006 [6] ZHANG Y, ZHANG L, ZHANG Y, et al. YiQiFuMai powder injection attenuates coronary artery ligation-induced heart failure through improving mitochondrial function via regulating ROS generation and CaMKII signaling pathways[J]. Front Pharmacol, 2019, 10: 381. doi: 10.3389/fphar.2019.00381 [7] XIA CL, CHU P, LIU YX, et al. ALDH2 rs671 polymorphism and the risk of heart failure with preserved ejection fraction (HFpEF) in patients with cardiovascular diseases[J]. J Hum Hypertens, 2020, 34(1): 16. doi: 10.1038/s41371-019-0182-2 [8] 关飞, 方克伟. 线粒体融合蛋白-2生物学功能及其在疾病中作用的研究进展[J]. 山东医药, 2017, 57(38): 106. [9] CHEN CH, FERREIRA JCB, MOCHLY-ROSEN D. ALDH2 and cardiovascular disease[J]. Adv Exp Med Biol, 2019, 1193: 53. [10] SAMANGOUEI P, CRESPO-AVILAN GE, CABRERA-FUENTES H, et al. MiD49 and MiD51: New mediators of mitochondrial fission and novel targets for cardioprotection[J]. Cond Med, 2018, 1(5): 239. [11] 张磊. KLF9调节心脏线粒体代谢功能的分子机制研究[D]. 北京: 北京协和医学院, 2018. [12] 严凌. 线粒体融合蛋白-2与心血管疾病[J]. 心管病学进展, 2011(32): 276. [13] ZHAO N, ZHANG Y, LIU Q, et al. Mfn2 Affects Embryo Development via Mitochondrial Dysfunction and Apoptosis[J]. PLoS One, 2015, 10(5): e0125680. doi: 10.1371/journal.pone.0125680 [14] HU L, DING M, TANG D, et al. Targeting mitochondrial dynamics by regulating Mfn2 for he rapeutic interventionindiabetic cardiomyopathy[J]. Theranostics, 2019, 9(13): 3687. doi: 10.7150/thno.33684 [15] YU H, GUO Y, MI L, et al. Mitofusin 2 inhibits angiotensin II-induced myocardial hypertrophy[J]. J Cardiovasc Pharmacol Ther, 2011, 16(2): 205. doi: 10.1177/1074248410385683 [16] MA S, CAO F. Targeting ALDH2 in atherosclerosis: molecular mechanisms and therapeutic opportunities[J]. Adv Exp Med Biol, 2019, 1193: 211. [17] HUA Y, CHEN H, ZHAO X, et al. Alda-1, an aldehyde dehydrogenase-2 agonist, improves long-term survival in rats with chronic heart failure following myocardial infarction[J]. Mol Med Rep, 2018, 18(3): 3159. [18] 谷小雨. ALDH2对高糖诱导的心肌成纤维细胞损伤及MMP-14/TIMP-4蛋白的影响[D]. 蚌埠: 蚌埠医学院, 2017. [19] 刘敏. ALDH2对1型糖尿病致心肌损伤的保护作用及其机制研究[D]. 西安: 第四军医大学, 2015. [20] LIAO J, SUN A, XIE Y, et al. Aldehyde dehydrogenase-2 deficiency aggravates cardiac dysfunction elicited by endoplasmic reticulum stress induction[J]. Mol Med, 2012, 18(1): 785. [21] 胡艺川. 乙醛脱氢酶2可减少氧化损伤诱导的心肌细胞凋亡[J]. 基因组学与应用生物学, 2019, 38(3): 1417. [22] 刘宝山. 乙醛脱氢酶2(ALDH2)的心肌保护作用及调控机制研究[D]. 济南: 山东大学, 2018. [23] 徐晓晓, 贾如意, 王涛, 等. 半乳糖凝集素-3、可溶性基质溶素-2检测对心力衰竭诊断的相关性研究[J]. 中国循环杂志; 2016, 31(9): 866. -





 下载:
下载: