-
传统皮瓣修复目的是使皮瓣成活并达到创面愈合,对于皮瓣受区形态和功能的恢复,尤其是皮瓣供区损伤问题,没有给予足够重视[1]。自杨果凡等[2]于1981年首次报道前臂皮瓣并应用于头颈部软组织修复后,其一度成为头颈部修复重建的主要手段[3-4]。然而,前臂皮瓣尚存在较为明显的缺陷,如牺牲测量桡动脉血管、需要开辟第二供区进行创面植皮、供区瘢痕明显且影响功能等[5-8]。1989年KOSHIMA等[9]报道以腹壁下动脉为蒂的下腹部皮瓣用于修复口底以及腹股沟缺损,被视为穿支皮瓣的研究开端。近年来,随着修复重建外科的不断发展,在保证修复重建效果的同时,尽可能减少供体区域损害已逐渐成为修复重建外科医生的共识[10]。以腹壁浅动脉和旋髂浅动脉为蒂的下腹部浅动脉穿支皮瓣,因其不涉及腹壁肌层和主干血管,可行“双组手术”以及供区并发症较少等优势,逐渐应用于口腔颌面部软组织缺损的修复重建[11-13]。本研究选择下腹部浅动脉穿支皮瓣与前臂皮瓣各15例,对两者供区远期并发症进行回顾性分析,探讨前者在临床应用中的价值与优势。现作报道。
-
选取2018年7月至2020年1月我科行游离下腹部浅动脉穿支皮瓣修复口腔癌术后软组织缺损的病人15例作为观察组,其中男9例,女6例;年龄24~75岁。选取2018年8月至2019年10月同期行前臂皮瓣修复病人15例作为对照组,其中男8例,女7例,年龄35~76岁。2组病人年龄和性别均具有可比性。
-
通过主观评价与客观检查两种方式对供区的远期并发症和功能恢复进行评估。供区远期并发症主要有感觉异常、瘢痕增生以及色素沉着等。
-
通过复诊,电话随访以及问卷调查等形式询问病人对于供区状态的满意程度,包括下腹部(或前臂)力量有无减退、有无感觉异常以及对供区外观是否不满意。同时咨询病人对于瘢痕位置的倾向性选择。
-
从供区功能与供区外观两方面进行。其中供区功能通过感觉功能与肌力检查进行评估,手术区和非手术区均进行检查。(1)感觉功能检测[14]:供区评估部位主要包括前臂皮瓣为前臂掌背侧的下三分之一、下腹部浅动脉穿支皮瓣为髂前上棘与脐连线的中下三分之一。采用Semmes-Weinstein单丝试验测定病人的感觉功能,检测时病人闭眼,单丝由轻到重依次进行,若单丝弯曲且病人有感觉,则举手示意,同时检测两侧相同部位,对每个区域进行三次检测,感觉不一致则为感觉异常。(2)肌力检查:①下腹部手动肌肉功能测定[15],病人仰卧于检查台,双臂交叉在胸前,检查者将双腿抬高至90°,膝盖伸直。病人被要求在不弯曲膝盖的情况下将双腿放低到检查台上,检查者将一只手放在病人髂后上棘,根据失去骨盆后倾时所对应的角度对病人进行分级。②桡侧腕屈肌肌力检查,要求病人屈腕及外展,检查者给予阻力,并于桡腕关节处触摸紧张的肌腱。③旋前圆肌肌力检查,要求病人伸直前臂,并使前臂由旋后位做旋前动作,检查者给予阻力,测知其肌力。④肱桡肌肌力检查,病人前臂取旋前旋后中立位,然后嘱其屈肘,检查者给以阻力,同时触摸病人前臂收缩的肌肉[16]。2组肌力测定结果根据Lovett分级法[17]简化为减退和无影响。(3)供区外观包括瘢痕增生及色素沉着检查:采用温哥华瘢痕量表(Vancouver scar scale, VSS)[18]评估瘢痕增生和色素沉着。该量表从色泽、厚度、血管分布和柔软度4个指标对瘢痕增生和色素沉着进行描述性评估,量表总分15分, 评分越高表示瘢痕增生和色素沉着越严重。
-
采用t检验、χ2检验和Fisher′s确切概率法。
-
观察组15例中14例皮瓣全部存活,1例术后72 h皮瓣颜色变紫,及时手术探查发现静脉回流受阻,去除吻合口栓子后,静脉血流速减慢,重新吻合通畅,皮瓣颜色未见明显好转,术后第10天,皮瓣部分坏死,创面延期愈合;供区创面经潜行分离后,均直接拉拢缝合,平均复查时间为7个月(术后3~15个月)。对照组15例皮瓣全部存活,供区创面均植皮修复,平均复查时间为8个月(术后3~15个月)。
-
2组病人主观评价中肌力减退情况差异无统计学意义(P>0.05),观察组感觉异常、供区外观主观评价情况均明显优于对照组(P < 0.01)(见表 1)。对于瘢痕位置的倾向性选择,30例回访病人中27例倾向瘢痕位于下腹部,表示无所谓的有1例,倾向于前臂的有2例。绝大部分病人表示前臂瘢痕容易暴露,影响美观。其中2例瘢痕倾向于前臂病人,均为行前臂皮瓣修复的男性病人,表示对瘢痕位置不在乎,认为其外观对生活影响不大。
分组 n 肌力减退 感觉异常 供区外观不满意 观察组 15 1(6.67) 1(6.67) 1(6.67) 对照组 15 5(33.33) 15(100.00) 11(73.33) P — >0.05△ < 0.01△ < 0.01△ △示Fisher′s确切概率法 表 1 2组病人供区功能主观评价情况比较[n;百分率(%)]
-
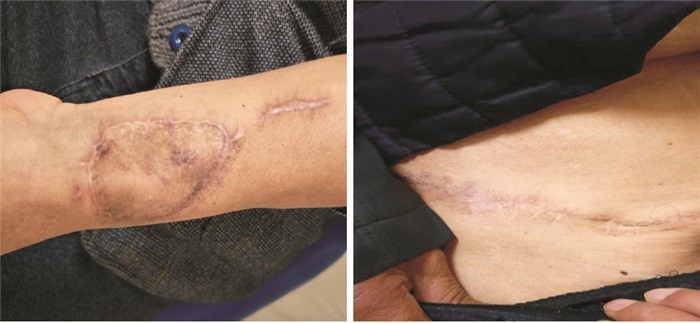
2组病人供区感觉与功能的客观检查中,观察组肌力减退、感觉异常情况均优于对照组(P < 0.05和P < 0.01)(见表 2)。供区外观客观检查结果显示,观察组病人瘢痕色泽、厚度、血管分布、柔韧度和总分均明显优于对照组(P < 0.01)(见表 3)。增生瘢痕及色素沉着典型病例见图 1。
分组 n 肌力减退 感觉异常 观察组 15 0(0.00) 1(6.67) 对照组 15 5(33.33) 15(100.00) P — < 0.05△ < 0.01△ △示Fisher′s确切概率法 表 2 供区功能客观检查情况比较[n;百分率(%)]
分组 n 色泽 厚度 血管分布 柔韧度 总分 观察组 15 0.73±0.70 0.87±0.64 1.00±0.66 1.07±0.59 3.67±1.45 对照组 15 2.40±0.63 2.60±0.63 2.13±0.64 2.47±0.74 9.60±1.40 t — 6.87 7.46 4.76 5.73 11.39 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 表 3 2组病人供区外观VSS量表评分比较(x±s;分)
-
近年来,前臂皮瓣由于供区损伤较大以及瘢痕容易暴露等缺陷,在临床应用中有下降趋势[7]。然而前臂皮瓣具有血管恒定、组织量适中、制备相对简单等优点,适用于唇、舌、口底等部位的修复,在口腔颌面外科领域仍起着重要的作用[19-20]。随着生活水平的不断提高,人们对生活质量及美的需求日益强烈,一方面要求受区创面的修复可以获得最佳外形与功能;另一方面又希望尽可能减小皮瓣供区的损害[1, 21]。穿支皮瓣技术的出现,为此奠定了基础。在综合考虑所需皮瓣的外观及功能的前提下,修复重建外科医生更多地关注选择哪里的供区最为隐蔽同时又对美观影响最小。四肢近端比远端隐蔽,而躯干又比四肢隐蔽,因此,身体最为隐蔽的区域为下腹部、腹股沟部、臀部、大腿近端,而此区域恰是泳裤可以覆盖到的地方,被称之为“泳裤供区”[10]。下腹部浅动脉穿支皮瓣位于下腹部,具有瘢痕隐蔽、供区美观影响小等优点,是一个符合“泳裤供区”理念的皮瓣。
本研究结果显示,采用下腹部浅动脉穿支皮瓣重建的病人有更好的供区感觉和对外观的满意度。有报道显示,前臂皮瓣的制取会导致供区皮神经的损伤,从而增加感觉异常出现的风险[22-23],而制取下腹部浅动脉穿支皮瓣时,由于切取层次位于腹壁深筋膜浅面,不涉及腹壁肌肉且未损伤相关神经[24]。因此,下腹部浅动脉穿支皮瓣发生感觉异常的风险小于前臂皮瓣,同样病人主观感受也有较为明显的差异。对于瘢痕位置的倾向性选择中,绝大多数病人(90%)更愿意选择下腹部作为皮瓣的供区,认为前臂瘢痕不易遮蔽,影响美观,而选择前臂的2例病人则是考虑到前臂皮瓣制备更加容易、技术要求低、风险较小。不难发现由于前臂皮瓣术后瘢痕容易外露,会对病人术后的自我感受与社交能力产生负面影响,而下腹部供区隐蔽,也更容易被病人所接受。
结合供区外观客观检查结果分析,2组皮瓣瘢痕增生与色素沉着差异均有统计学意义。前臂皮瓣表现出更为明显的瘢痕增生和色素沉着,传统的前臂皮瓣获取后,供区缺损常不能拉拢缝合且需行中厚或全厚皮片植皮修复[25],由于植皮后供区的颜色、质地和周围邻近皮肤有较为明显的差异,植皮部位愈合后往往会出现局部组织凹陷畸形和明显的色素沉着。ITO等[26]报道23例行前臂皮瓣修复的病人中,有9例(39.1%)病人植皮区存在较为明显的色素沉着,16例(69.7%)病人出现局部组织凹陷畸形。ORLIK等[27]报道了移植皮片坏死脱落导致前臂肌腱外露、植皮区麻木、瘢痕粗大等不良后果。相反,下腹部浅动脉穿支皮瓣供区可直接缝合,无需增加新的术区,明显减小供区并发症,而且下腹部供区遗留的瘢痕由于部位隐蔽, 对外观损害更小, 病人更容易接受。然而该皮瓣尚存在着血管变异较大、管径较小、制备要求相对较高等不足[28],为临床手术操作增加了难度。
综上所述,对比前臂皮瓣,下腹部浅动脉穿支皮瓣有着供区创口可直接拉拢缝合,并发症相对较少、主客观感觉异常相对较少、瘢痕隐蔽增生不明显、术后供区外观满意度高等优点,是口腔颌面部软组织缺损修复的较好选择。
下腹部浅动脉穿支皮瓣与前臂皮瓣供区远期功能恢复的比较
Comparison of the long-term functional recovery of the donor site between the superficial inferior abdominal artery perforator flap and forearm flap
-
摘要:
目的比较口腔癌病人同期应用下腹部浅动脉穿支皮瓣和前臂皮瓣供区术后远期并发症,评价下腹部浅动脉穿支皮瓣在临床应用中的价值。 方法回顾性分析因病灶扩大切除而行游离下腹部浅动脉穿支皮瓣(腹壁浅动脉穿支皮瓣或旋髂浅动脉穿支皮瓣)修复的口腔癌病人15例(观察组)临床资料,以及同期行前臂皮瓣修复的口腔颌面软组织缺损病人15例(对照组),比较2组病人术后供区远期并发症发生情况,包括感觉异常、瘢痕增生以及色素沉着等,并评估供区远期功能恢复情况。 结果观察组病人供区创面经潜行分离后,直接拉拢缝合,术后仅遗留线形瘢痕,对美观和功能影响较小;对照组病人供区创面均植皮修复,术后供区瘢痕增生和色素沉着较明显。病人皮瓣术后供区主观感受比较显示,2组肌力减退情况差异无统计学意义(P>0.05),观察组感觉异常、供区外观主观评价情况均明显优于对照组(P<0.01)。2组病人供区感觉与功能、外观的客观检查中,观察组肌力减退、感觉异常情况均优于对照组(P<0.05和P<0.01),瘢痕色泽、厚度、血管分布、柔韧度和总分亦均明显优于对照组(P<0.01)。 结论应用下腹部浅动脉穿支皮瓣修复,供区并发症少,对供区美观、功能影响小,是口腔颌面部软组织缺损修复的较好选择。 Abstract:ObjectiveTo evaluate the clinical value of the superficial inferior abdominal artery perforator flap in oral cancer patients by comparing the long-term complications of the donor site between the superficial inferior abdominal artery perforator flap and forearm flap. MethodsThe clinical data of 15 oral cancer patients(observation group) treated with free superficial inferior abdominal artery perforator flaps(superficial inferior epigastric artery perforator flaps or superficial circumflex iliac artery perforator flaps) for extensive resection of lesions and 15 oral and maxillofacial soft tissue defect patients(control group) treated with forearm flaps to repair at the same time were retrospectively analyzed.The long-term complications of the donor site(including paresthesia, hyperplasia of scar and pigmentation) were compared between two groups, and the long-term functional recovery of the donor site was evaluated in two groups. ResultsIn the observation group, the donor wound was directly pulled and sutured after stealth separation, and only linear scar was left after surgery, which had little effect on aesthetics and function.In the control group, the skin grafting was performed on the donor wounds, and the postoperative hyperplasia and hyperpigmentation of scars were obvious.The comparison results of the subjective feelings of patients in the donor site after skin flap surgery showed that there was no statistical significance in the decrease of muscle strength between two groups(P>0.05), and the paresthesia and subjective evaluation of the donor site appearance in observation group was significantly better than those in control group(P < 0.01).In the objective examination of the sensation, function and appearance of the donor site of patients in two groups, the muscle strength decreasing and paresthesia in observation group were better than those in control group(P < 0.05 and P < 0.01), and the color, thickness, vascular distribution, flexibility and total score of scar in observation group were also significantly better than those in control group(P < 0.01). ConclusionsThe superficial inferior abdominal artery perforator flap is a good choice for the repair of oral and maxillofacial soft tissue defects, which has less complications at the donor site and less influence on the appearance and function of the donor site. -
表 1 2组病人供区功能主观评价情况比较[n;百分率(%)]
分组 n 肌力减退 感觉异常 供区外观不满意 观察组 15 1(6.67) 1(6.67) 1(6.67) 对照组 15 5(33.33) 15(100.00) 11(73.33) P — >0.05△ < 0.01△ < 0.01△ △示Fisher′s确切概率法 表 2 供区功能客观检查情况比较[n;百分率(%)]
分组 n 肌力减退 感觉异常 观察组 15 0(0.00) 1(6.67) 对照组 15 5(33.33) 15(100.00) P — < 0.05△ < 0.01△ △示Fisher′s确切概率法 表 3 2组病人供区外观VSS量表评分比较(x±s;分)
分组 n 色泽 厚度 血管分布 柔韧度 总分 观察组 15 0.73±0.70 0.87±0.64 1.00±0.66 1.07±0.59 3.67±1.45 对照组 15 2.40±0.63 2.60±0.63 2.13±0.64 2.47±0.74 9.60±1.40 t — 6.87 7.46 4.76 5.73 11.39 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 -
[1] 唐举玉, 汪华侨, HALLOCK GG, 等. 关注皮瓣供区问题——减少皮瓣供区损害专家共识[J]. 中华显微外科杂志, 2018, 41(1): 3. doi: 10.3760/cma.j.issn.1001-2036.2018.01.001 [2] 杨果凡, 陈宝驹, 高玉智. 前臂皮瓣游离移植术(附56例报告)[J]. 中华医学杂志, 1981, 61(3): 139. doi: 10.3760/j:issn:0376-2491.1981.03.007 [3] ORANGES CM, LING B, TREMP M, et al. Comparison of anterolateral thigh and radial forearm free flaps in head and neck reconstruction[J]. In Vivo, 2018, 32(4): 893. doi: 10.21873/invivo.11325 [4] KIM MS, OH KH, CHO JG, et al. Assessment of chronological volume changes in radial forearm free flaps for tongue cancer[J]. ORL J Otorhinolaryngol Relat Spec, 2020, 6: 1. [5] KRANE NA, MOWERY A, AZZI J, et al. Reconstructing forearm free flap donor sites using full-thickness skin grafts harvested from the ipsilateral arm[J]. Otolaryngol Head Neck Surg, 2020, 162(3): 277. doi: 10.1177/0194599819901124 [6] PIRLICH M, HORN IS, MOZET C, et al. Functional and cosmetic donorsite morbidity of the radial forearm-free flap: comparison of two different coverage techniques[J]. Eur Arch Otorhinolaryngol, 2018, 275(5): 1219. doi: 10.1007/s00405-018-4908-5 [7] 姚麟, 郭萌萌, 邓璋, 等. 对偶三角瓣联合原位小面积全厚皮片修复前臂游离皮瓣供区缺损[J]. 中国口腔颌面外科杂志, 2020, 18(1): 64. [8] 洪鹏宇, 高陆, 邱冠华, 等. 前臂皮瓣与股前外侧皮瓣修复口腔癌术后缺损临床研究[J]. 口腔医学研究, 2019, 35(1): 46. [9] KOSHIMA I, SOEDA S. Inferior epigastric artery skin flaps without rectus abdominis muscle[J]. Br J Plas Surg, 1989, 42(6): 645. doi: 10.1016/0007-1226(89)90075-1 [10] 张敬良. 努力追求创面修复的"泳裤供区"理念[J]. 中华显微外科杂志, 2020, 43(1): 3. doi: 10.3760/cma.j.issn.1001-2036.2020.01.002 [11] 王宏伟, 郭兵, 马春跃, 等. 腹壁浅动脉穿支皮瓣修复口腔颌面部软组织缺损3例报道[J]. 中国口腔颌面外科杂志, 2018, 16(1): 78. [12] 王栋, 刘亮, 杨东昆, 等. 腹壁浅动脉穿支皮瓣一期修复口腔癌术后软组织缺损三例[J]. 中华显微外科杂志, 2019, 42(6): 579. doi: 10.3760/cma.j.issn.1001-2036.2019.06.016 [13] 阮敏, 马春跃, 周辉红, 等. 旋髂浅动脉穿支皮瓣修复颊癌术后缺损的临床应用[J]. 口腔医学研究, 2017, 33(9): 966. [14] 张铁柱, 毛驰, 姜颖, 等. 修复口腔缺损常用游离皮瓣供区表面感觉的研究[J]. 现代口腔医学杂志, 2007, 21(6): 573. doi: 10.3969/j.issn.1003-7632.2007.06.005 [15] SELBER JC, NELSON J, FOSNOT J, et al. A prospective study comparing the functional impact of SIEA, DIEP, and muscle-sparing free TRAM flaps on the abdominal wall: part Ⅰ. unilateral reconstruction[J]. Plast Reconstr Surg, 2010, 126(4): 1142. doi: 10.1097/PRS.0b013e3181f02520 [16] 崔秋菊, 毛驰, 栾修文, 等. 腓肠内侧动脉穿支皮瓣和前臂皮瓣的术后供区影响对比[J]. 口腔疾病防治, 2018, 26(8): 514. [17] 孔燕, 刘志华, 崔应麟. 延续综合护理及康复训练联合高压氧治疗对急性缺血性脑卒中病人Lovett肌力分级及NIHSS评分的影响[J]. 中国老年学杂志, 2018, 38(4): 793. doi: 10.3969/j.issn.1005-9202.2018.04.011 [18] 刘海兵, 唐丹, 曹海燕, 等. 温哥华瘢痕量表的信度研究[J]. 中国康复医学杂志, 2006, 21(3): 240. doi: 10.3969/j.issn.1001-1242.2006.03.015 [19] 刘亮, 张凯, 李建成, 等. 个性化前臂皮瓣在口腔颌面部缺损修复的临床观察[J]. 中华显微外科杂志, 2017, 40(1): 30. doi: 10.3760/cma.j.issn.1001-2036.2017.01.010 [20] 陈永锋, 张凯, 李建成, 等. 前臂皮瓣联合邻近组织瓣修复腭及上颌组织缺损早期疗效[J]. 中国修复重建外科杂志, 2011, 25(9): 1051. [21] 刘元波, 朱珊, 臧梦青, 等. 穿支皮瓣研究领域的新技术、新方法[J]. 中华整形外科杂志, 2019, 35(9): 835. doi: 10.3760/cma.j.issn.1009-4598.2019.09.001 [22] KANSY K, HOFFMANN J, ALHALABI O, et al. Long-term donor site morbidity in head and neck cancer patients and its impact on quality of life: a cross-sectional study[J]. Int J Oral Maxillofac Surg, 2019, 48(7): 875. doi: 10.1016/j.ijom.2019.01.009 [23] WANG F, DING X, ZHANG J, et al. Somatosensory changes at forearm donor sites following three different surgical flap techniques[J]. Int J Surg, 2018, 53: 326. doi: 10.1016/j.ijsu.2018.04.008 [24] 张凯, 王栋, 高廷益, 等. 彩色多普勒超声辅助下腹部浅动脉供血皮瓣修复颌面部软组织缺损[J]. 中华整形外科杂志, 2019, 35(12): 1200. doi: 10.3760/cma.j.issn.1009-4598.2019.12.007 [25] CHANG EI, LIU J. Prospective comparison of donor site morbidity following radial forearm and ulnar artery perforator flap harvest[J]. Plast Reconstr Surg, 2020, 145(5): 1267. doi: 10.1097/PRS.0000000000006790 [26] ITO O, IGAWA HH, SUZUKI S, et al. Evaluation of the donor site in patients who underwent reconstruction with a free radial forearm flap[J]. J Reconstr Microsurg, 2005, 21(2): 113. doi: 10.1055/s-2005-864844 [27] ORLIK JR, HORWICH P, BARTLETT C, et al. Long-term functional donor site morbidity of the free radial forearm flap in head and neck cancer survivors[J]. J Otolaryngol Head Neck Surg, 2014, 43(1): 1. doi: 10.1186/1916-0216-43-1 [28] 王晓敏, 张凯, 马士崟, 等. 腹壁浅动脉皮瓣的应用解剖研究[J]. 中国修复重建外科杂志, 2010, 24(11): 1357. -





 下载:
下载: