-
先天性唇裂是一种常见的口腔颌面部畸形,我国发病率为1.66%~1.82%,其发病原因尚不完全明确,据报道[1]多由基因和环境因素共同作用所致。其畸形表现多样,单侧Ⅲ度唇裂为其中一种,从外观看主要表现为单侧唇及鼻基底的裂隙,包括鼻唇正常结构的发育畸形和偏移,因其常伴有牙槽的错位及上颚裂隙的问题,故手术的难度及不确定性均较大。单纯唇裂修复手术的中心思想为打断鼻唇部原有的异常解剖结构,重建其肌肉的连续性,从而建立正常的解剖结构、功能以及提高鼻唇部对称性[2-3]。近年来,因传统Millard术式对Ⅲ度唇裂修复的局限性,从而衍生出各种改良术式,本研究以改良Millard术式为手术方法对单侧Ⅲ度唇裂进行修复, 并以几何学原理评估其修复效果及稳定性。现作报道。
-
选取2018年10月至2020年7月就诊于我治疗中心的唇裂患儿中,改良Millard法修复的单侧Ⅲ度唇裂病人40例,其中男23例,女17例,年龄3~12个月,其中左侧24例,右侧16例。为尽可能减小因施术者技术的不同所产生的误差,所选患儿的手术均由同一位医师采用该术式完成,所有照片和数据的采集及处理过程由另外一名医务人员统一完成。
纳入标准:(1)告知患儿家属进行该测量研究的目的意义以及测量时需要配合的注意事项,并征得同意后,再进行测量; (2)除Ⅲ度唇腭裂外无其他先天性畸形; (3)鼻唇部无外伤史及手术史; (4)术前行血常规、生化常规、免疫过筛、凝血功能、心电图、胸片等检查,均无明显手术禁忌证。排除标准: (1)有先天性心脏病及各种严重器官系统疾病无法手术者; (2)其他类型的唇腭裂病人; (3)鼻唇部有皮肤病者。
-
照片采集的时间点选择为术前(T1)、术后1周(T2)、术后1年(T3)以上,采集过程如下:将患儿转移至水平桌面上,以平卧位将患儿的头部固定在头部固定枕上,待患儿安静后,在其面部正上方,垂直以固定距离用专业数码相机进行拍摄,确保拍摄参数及影响因素一致;限于患儿配合程度及疫情原因,术后1年的照片以上述同标准采集较困难,最终从同标准采集成功的患儿中选取21例,进行后续分析。
-
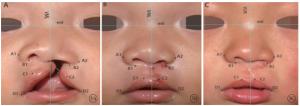
将图片导入Photoshop软件中,并以双侧内眦点水平为据,对图片进行矫正,矫正完毕后以内眦间距的均数为标准将各患儿的照片进行等比例的放大及缩小从而实现内眦间距点的等距化处理(以减少因各患儿面部发育的差异所带来的影响),为排除面部形态对于操作者对照片处理及定位的影响,对原照片以矩形范围进行截取,尽可能只保留内眦、鼻、唇在内[4],以Farkas定点法[5]为基础,其中包括2线构成的参照系:患儿双眼内眦点连线及其延长线(enl)、患儿双眼内眦点连线中点的中垂线(VML)及8个待分析的测量点:双侧鼻翼点、双侧鼻翼基部点、双侧唇峰点、双侧口角点,健侧各点依次记为A1、B1、C1、D1、患侧各点依次记为A2、B2、C2、D2(见图 1)。确定VML及enl,两线确定完毕后,以两线交点为新原点,将Photoshop坐标轴与新原点进行重合,从而实现参照系的重建。以新坐标系为参考,在Photoshop软件内进行各测量点的坐标记录,为减小误差,每个坐标点均进行三次不做标记的定点记录后取三次坐标数据的均数作为待测点坐标,计算术前、术后1周及术后1年各测量点所在坐标围成的面积,手术时间点分别记为T1、T2、T3,并将健、病人各测量点所在的坐标面积进行比较(以面积较小者比上面积较大者),经百分化后称之为对称率;第二次对称性分析,除对比术前、术后1周各测量点对称率的变化外。对术后1年健、患侧各测量点坐标面积进行比较,初步评估对称性,同时将术后1年时的颜面部各点对称率与术后1周时进行对称率比较,以此来评估面部各亚单位的对称率的稳定性。同时对病人在1年的时间里,正常发育生长下健侧颜面部改变情况及患侧颜面部改变情况进行分析,以此来判断修复术后的稳定性以及远期稳定性。术前及术后1周因内眦间距短时间不会发生变化,当以同一患儿内眦间距为标准时,各项指标在进行比较时误差较小,随患儿生长发育速度不同,术后1年,各患儿内眦间距已发生不同程度的改变,以对称率为参考标准可以很好的缩小因生长发育的差异所带来的误差。
-
采用配对t检验、方差分析和q检验。
-
40例患儿术前的鼻翼点(A)、鼻翼基部点(B)、唇峰点(C)、口角点(D)的健侧坐标点面积均小于患侧(P < 0.01),术后1周时,B点的健、患侧坐标面积差异均无统计学意义(P>0.05),A、C、D点健侧面积仍小于患侧(P < 0.01)(见表 1)。
位置 n A点 B点 C点 D点 T1 T2 T1 T2 T1 T2 T1 T2 健侧 40 238.53±8.94 231.14±8.62 201.55±11.84 177.25±6.89 281.2±24.40 145.16±8.01 571.04±26.70 508.00±20.04 患侧 40 276.70±12.32 254.25±9.14 255.52±14.25 180.67±10.12 329.07±14.30 154.97±14.32 632.17±31.42 533.69±27.10 t — 19.19 11.26 20.95 1.74 9.97 3.80 9.30 5.56 P — < 0.01 < 0.01 < 0.01 >0.05 < 0.01 < 0.01 < 0.01 < 0.01 表 1 术前、术后1周面部健、患侧各测量点坐标面积比较(x ± s; mm2)
-
因疫情等因素影响,最终选取21例患儿进行比较,以下21例患儿的术前和术后1周的二维对比结果(见表 2)与此前以40例患儿为样本来源时结果一致。21例患儿术前的A、B、C、D的健侧坐标点面积均小于患侧(P < 0.01);术后1周时,B点的健、患侧坐标面积差异无统计学意义(P>0.05),A、C、D点健侧面积仍小于患侧(P < 0.01);术后1年,B、C、D点健、患侧差异无统计学意义(P>0.05),仅A点健侧面积仍小于患侧(P < 0.01)(见表 2)。
位置 A点 B点 T1 T2 T3 T1 T2 T3 健侧 240.23±6.12 233.51±8.33 246.63±12.36 197.54±7.66 178.11±5.49 188.52±7.79 患侧 273.46±8.38 256.66±5.12 260.42±8.71 253.31±10.27 181.67±9.32 192.43±10.06 t 13.94 9.92 4.29 17.78 1.46 1.38 P < 0.01 < 0.01 < 0.01 < 0.01 >0.05 >0.05 位置 C点 D点 T1 T2 T3 T1 T2 T3 健侧 282.97±18.37 144.70±10.41 152.37±8.16 586.67±16.72 516.32±17.44 551.66±20.04 患侧 331.58±11.09 151.96±9.56 154.41±9.33 639.55±22.48 545.69±19.80 560.17±17.10 t 10.40 2.14 1.12 8.80 5.25 1.53 P < 0.01 < 0.05 >0.05 < 0.01 < 0.01 >0.05 表 2 术前、术后1周、及术后1年面部健、患侧各测量点坐标面积比较(x ± s;mm2)
-
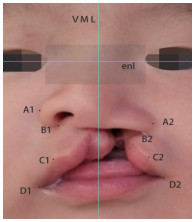
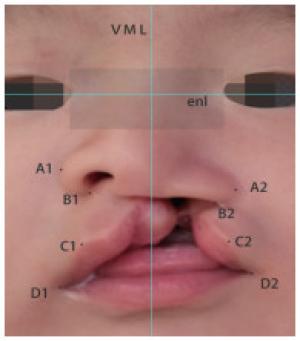
21例患儿术后1周和术后1年健、患侧各测量点对称率均高于术前(P < 0.01),术后1年的A点和D点的对称率高于术后1周(P < 0.01)(见图 2、3、表 3)。
测量点 n 对称率 F P MS组内 T1 T2 T3 A点 21 86.20±1.03 90.98±0.91** 94.70±0.77**△△ 504.03 < 0.01 13.777 B点 21 78.87±2.26 98.04±0.37** 97.97±0.46** 1 316.56 < 0.01 88.671 C点 21 85.45±3.74 95.22±1.03** 95.58±0.86** 128.44 < 0.01 28.863 D点 21 90.33±3.48 94.61±1.31** 96.69±0.72**△△ 53.24 < 0.01 12.319 注:与T1时比较*P<0.05, **P<0.01;与T2时比较△P<0.05, △△P< 0.01 表 3 术前、术后1周及术后1年面部各测量点对称率比较[x ± s;百分率(%)]
-
唇腭裂作为人类面部常见畸形之一,常导致患儿颜面部外观皮肤、皮下组织及肌肉等结构的连续性中断,表现为颜面部失对称性改变,此外患儿的语音功能及心理发育也深受影响,因此,唇腭裂手术意义重大。对其解剖结构及功能的重建一直以来都备受国内外学者的关注。对于Ⅲ度唇裂,以往常采用传统Millard术式进行修复,近年来随着研究的不断深入以及对手术方式的不断改进[6-7],手术方法多样,但仍未能发现一种完美的修复方法,而改良Millard术式仍是目前较为主流的修复方法[8-9],其优势主要表现为该手术的灵活性较高,虽设计简单,但具体手术过程需据病人自身情况而定,此法可于术中灵活调整患侧唇峰点及健侧鼻小柱基底点定位,牺牲唇宽弥补唇高下降的不足,必要时也可于患侧上唇分出等腰“三尖瓣”辅助下降唇高,或达到平衡唇宽与唇高的目的。在红唇缝合时,如发现红唇连续性不佳、形态不够饱满等,亦可从患侧红唇分出“三角瓣”,插入健侧红唇切口内,以预防因张力及缝合因素造成的红唇凹陷,使术后唇部外形更为饱满以及干湿唇线弧度更为自然[10]。又因其切除的组织量较少,故而术后切口的张力较小,可一定程度上减轻瘢痕的形成,存余组织量还可以有效地辅助鼻基底的封闭[2]以及鼻槛的重建,可在腭裂修复前,为病人语音功能的建立及生理功能的恢复奠定基础。
本研究以改良Millard法对Ⅲ度唇裂进行修复,术后以面部形态学测量即照片测量法[11]为基础进行定点测量及分析,有研究证明照片测量法具有高度的可重复性,且性价比极高, 在科技十分发达的今天,照片测量法依然在国内外被广泛的应用于医学研究[12-14]。由照片测量法数据可知,术前A、B点的健、患侧坐标面积差异较大,对称率分别86.2%、78.87%,经手术修复后1周,A点健、患侧坐标面积虽然仍有差异,但其对称率达90.98%,与术前86.2%相比得到了明显提升,而B点经修复后健、患侧坐标面积已近乎相等,其对称率高达98.04%,较术前78.87%提升更为明显,这或与术中将患侧鼻翼基部向内上适度旋转后缝合固定有关,结合大量研究报道[15-17],并以我科在近年来修复唇裂的经验及数据来看[18-19],患儿在2岁以前,鼻的发育处在其特定生长期内,因此过早过多的对鼻畸形进行整复,其后果不可估量,为尽可能减少唇裂术后继发鼻畸形的影响因素,不主张同期过多矫正鼻部畸形,故未对病人鼻翼进行整复,我科常于术后建议患儿家属对患儿予硅胶鼻撑进行辅助塑形[20],维持至少6个月以上,术后1年A点健、患侧坐标面积虽然仍有差异,但其对称率94.7%较术后1周时90.98%再次得到显著提升。虽然B点对称率97.97%较术后1周时98.04%略有下降,但差异并无统计学意义,其对称率得到了较好的维持;鼻作为颜面部最为突出的亚单位,其立体感较强,如只强调二维对称率或不能实现准确的评估,通过大量对Ⅲ度唇裂患儿的治疗经验来看,二期手术时,鼻的整复依然是重中之重,但一期手术对鼻的二维对称性的改善及维持,对颜面部整体对称性而言意义重大,为病人后期的鼻畸形修复奠定了一定的基础。
相关研究[21]表明,正常上唇的纵向生长发育程度有限,因此更强调初次手术对唇高的精确调整,但此特性于术后的生长发育阶段或有益于唇峰对称性的维持,本次研究数据C点经改良Millard法修复后,在术后1周及术后1年时对称率分别为95.22%、95.58%,与术前85.45%相比提升均较显著,且于术后1年的生长发育阶段依然保持稳定,C点对称性恢复良好且得到了较好的维持,与叶向阳等[20]研究具有一致性。而唇的横向生长幅度较纵向而言具有优势,D点间距在0~12岁存在4个相对的快速生成期[22],且据大量的唇裂术后随访报道表明[23],D点的对称性常能够因唇部解剖结构的重建,进行自我调整,于后期达到接近正常水平,本研究中D点经过1年的调整,其健、患侧坐标面积已无明显差异,对称率达96.69%,较术后1周时94.61%具有一定程度提升。
综上所述,改良Millard法对Ⅲ度唇裂患儿颜面部各亚单位的对称性改善显著,于术后1周及术后1年时的对称率均在90%以上,较术前明显改善,在术后1周至术后1年的生长发育阶段,仅B点对称率有所下降,但差异无统计学意义,其余各点仍有不同程度的改善,因此该术式可明显改善颜面部的对称性,同时能维持较好的稳定性。本研究因随访时间限制,无法进行更远期的效果分析,后期仍需进一步深入研究。
运用几何学原理评估改良Millard法对单侧Ⅲ度唇裂的修复效果
Study on the effects of modified Millard′s method in the reconstruction of unilateral degree Ⅲ cleft lip evaluated by geometric principles
-
摘要:
目的评估改良Millard法修复单侧Ⅲ度唇裂术后唇鼻畸形改善情况及其稳定性。 方法选取自2018年10月至2020年7月就诊的单侧Ⅲ度唇裂患儿40例,采用改良Millard法进行唇裂修复。按照同一标准将患儿术前、术后1周及术后1年作为时间点进行照片采集。对所采集照片以同一标准进行坐标系的构建。健、患侧的鼻翼点(A)、鼻翼基部点(B)、唇峰点(C)及口角点(D)进行定位测量。计算各测量点坐标面积及对称率。比较各时间点健、患两侧面积差异;评估对称率随时间的整体变化情况;分析两两时间点之间的对称率变化情况,以评估手术改善情况及稳定性。 结果健、患侧坐标面积之间比较,术前A、B、C、D点健、患侧差异较大(P < 0.01)。经改良Millard法手术修复,于术后1周时,A、C、D点差异仍有统计学意义(P < 0.01),仅B点两侧差异无统计学意义(P>0.05)。术后1年时,A点两侧差异有统计学意义(P < 0.01),但B、C、D点两侧差异无统计学意义(P>0.05)。在比较对称率的变化时发现,术后1周和术后1年各测量点对称率均高于术前(P < 0.01),术后1年的A和D点的对称率高于术后1周(P < 0.01)。 结论运用改良Millard法修复单侧Ⅲ度唇裂,唇鼻畸形改善明显,对称性改善较好且具有良好的稳定性。 -
关键词:
- 唇裂 /
- 改良Millard法 /
- 对称率
Abstract:ObjectiveTo evaluate the improvement and stability of the modified Millard′s method in the reconstruction of lip-nasal deformity after unilateral degree Ⅲ cleft lip surgery. Methods Forty children with unilateral degree Ⅲ cleft lip treated with the modified Millard′s method from October 2018 to July 2020 were investigated.According to the same standard, the photos were collected before surgery, after 1 week and 1 year of operation.The coordinate system was constructed according to the same standard for the photos collected, the alar point(A), alar base point(B), lip peak point(C) and front cut point(D) of the healthy and affected sides were measured, and the coordinate area and symmetry rate of each measuring point were calculated.The difference analysis was made by comparing the area of healthy and affected sides at each time point, the overall change of symmetry rate over time was evaluated and the changes of symmetry rate between two time points were analyzed to assess the surgical improvement and stability. ResultsThe differences of the coordinate area at A, B, C and D points between the healthy side and affected side before operation were statistically significant(P < 0.01).After the modified Millard′s method surgery, the differences of the A, C and D points between the healthy side and affected side after 1 week of operation were statistically significant(P < 0.01), and the difference of which in B point was not statistically significant(P>0.05).After 1 year of operation, the difference of the coordinate area at A point between the healthy side and affected side was statistically significant(P < 0.01), but the differences of which at B, C and D points were not statistically significant(P>0.05).The symmetry rate of each measurement point after 1 week and 1 year of operation was higher than that before surgery(P < 0.01), and the symmetry rates of A and D points after 1 year of operation were higher than that after 1 week of operation(P < 0.01). ConclusionsThe modified Millard′s method in the reconstruction of unilateral degree Ⅲ cleft lip can significantly improve the lip-nasal deformity, and make the symmetry and stability better. -
Key words:
- cleft lip /
- modified Millard′s method /
- symmetry rate
-
表 1 术前、术后1周面部健、患侧各测量点坐标面积比较(x ± s; mm2)
位置 n A点 B点 C点 D点 T1 T2 T1 T2 T1 T2 T1 T2 健侧 40 238.53±8.94 231.14±8.62 201.55±11.84 177.25±6.89 281.2±24.40 145.16±8.01 571.04±26.70 508.00±20.04 患侧 40 276.70±12.32 254.25±9.14 255.52±14.25 180.67±10.12 329.07±14.30 154.97±14.32 632.17±31.42 533.69±27.10 t — 19.19 11.26 20.95 1.74 9.97 3.80 9.30 5.56 P — < 0.01 < 0.01 < 0.01 >0.05 < 0.01 < 0.01 < 0.01 < 0.01 表 2 术前、术后1周、及术后1年面部健、患侧各测量点坐标面积比较(x ± s;mm2)
位置 A点 B点 T1 T2 T3 T1 T2 T3 健侧 240.23±6.12 233.51±8.33 246.63±12.36 197.54±7.66 178.11±5.49 188.52±7.79 患侧 273.46±8.38 256.66±5.12 260.42±8.71 253.31±10.27 181.67±9.32 192.43±10.06 t 13.94 9.92 4.29 17.78 1.46 1.38 P < 0.01 < 0.01 < 0.01 < 0.01 >0.05 >0.05 位置 C点 D点 T1 T2 T3 T1 T2 T3 健侧 282.97±18.37 144.70±10.41 152.37±8.16 586.67±16.72 516.32±17.44 551.66±20.04 患侧 331.58±11.09 151.96±9.56 154.41±9.33 639.55±22.48 545.69±19.80 560.17±17.10 t 10.40 2.14 1.12 8.80 5.25 1.53 P < 0.01 < 0.05 >0.05 < 0.01 < 0.01 >0.05 表 3 术前、术后1周及术后1年面部各测量点对称率比较[x ± s;百分率(%)]
测量点 n 对称率 F P MS组内 T1 T2 T3 A点 21 86.20±1.03 90.98±0.91** 94.70±0.77**△△ 504.03 < 0.01 13.777 B点 21 78.87±2.26 98.04±0.37** 97.97±0.46** 1 316.56 < 0.01 88.671 C点 21 85.45±3.74 95.22±1.03** 95.58±0.86** 128.44 < 0.01 28.863 D点 21 90.33±3.48 94.61±1.31** 96.69±0.72**△△ 53.24 < 0.01 12.319 注:与T1时比较*P<0.05, **P<0.01;与T2时比较△P<0.05, △△P< 0.01 -
[1] 马坚, 胡晨, 翟堃, 等. 宁夏1 482例先天性唇腭裂特征分析[J]. 宁夏医科大学学报, 2019, 41(10): 1042. [2] 李海鹏, 王予江, 宁文杰, 等. 单侧完全性唇裂鼻底修复的临床研究进展[J]. 国际口腔医学杂志, 2016, 43(1): 95. [3] 李承浩, 李业平, 石冰. 唇裂鼻畸形整复核心问题之华西观点[J]. 国际口腔医学杂志, 2019, 46(4): 383. [4] ALTU AT. Presurgical nasoalveolar molding of bilateral cleft lip and palate infants: an orthodontist′s point of view [J]. Turk J Orthod, 2017, 30(4): 118. doi: 10.5152/TurkJOrthod.2017.17045 [5] FARKAS LG. Anthropometry of the head and face[J]. Ann Occupat Hyg, 1994, 52(4): 773. [6] 李怡君. 改良Tennison-Randall术式在单侧唇裂患者中的应用及其术后效果评价[D]. 重庆: 重庆医科大学, 2018. [7] 方绍伟, 池朝玲, 朱光辉. 改良Tajima切口修复单侧唇裂术后继发鼻畸形[J]. 解放军预防医学杂志, 2017, 35(5): 474. [8] 高廷益, 张凯, 杨东昆, 等. 两种改良Millard法修复单侧唇裂的临床对比效果观察[J]. 口腔医学, 2017, 37(12): 1095. [9] 董文. 改良Millard法修复单侧完全性唇裂术后鼻部对称性的变化[D]. 银川: 宁夏医科大学, 2015. [10] GASSLING V, KOOS B, BIRKENFELD F, et al. Secondary cleft nose rhinoplasty: subjective and objective outcome evaluation[J]. Craniomaxillofac Surg, 2015, 43(9): 1855. doi: 10.1016/j.jcms.2015.08.012 [11] SUN BC, COU YN, JI LL, et al. Analysis of the clinical effect of 3 years after rhinoplasty in children with unilateral complete cleft lip and palate[J]. Chin J Pract Stomatol, 2016, 9(2): 93. [12] 张楠. 正畸掩饰性治疗对唇线倾斜的改善[D]. 重庆: 重庆医科大学, 2020. [13] 李一颖, 杨学财, 侯志军, 等. 口腔黏膜瓣用于非综合征型单侧完全性唇裂鼻底修复的效果评价[J]. 中国口腔颌面外科杂志, 2018, 16(5): 425. [14] LI YP, LIU RK, SHI B, et al. A new photogrammetry of nasal morphology for asian patients with unilateral secondary cleft lip nasal deformity[J]. Plast Reconstr Surg, 2019, 143(1): 244e. doi: 10.1097/PRS.0000000000005150 [15] PHILLIPS GSA, SWAN MC, SAWYER AR, et al. A Comparative study of the aesthetic outcome of two techniques for unilateral complete cleft lip repair[J]. Plast Reconstr Surg, 2017, 140(4): 757. doi: 10.1097/PRS.0000000000003685 [16] KUNA SK, SRINATH N, NAVEEN BS, et al. Comparison of outcome of modified millard's incision and delaire's functional method in primary repair of unilateral cleft lip: a prospective study[J]. J Maxillofac Oral Surg, 2016, 15(2): 221. doi: 10.1007/s12663-015-0816-z [17] 尹宁北. 中国式功能性唇裂修复术[J]. 中华口腔医学杂志, 2017, 52(4): 212. doi: 10.3760/cma.j.issn.1002-0098.2017.04.004 [18] 段志红, 徐静, 叶广春, 等. 改良Millard法结合鼻唇肌肉功能重建修复单侧唇裂21例[J]. 中国美容医学, 2020, 29(3): 75. [19] 叶广春, 李光早, 沈嬿, 等. 单侧完全性唇裂鼻唇特征的测量研究[J]. 中华全科医学, 2019, 17(6): 936. [20] 宋佳睿, 范飞. 面裂鼻畸形病因及临床诊疗的研究进展[J]. 医学综述, 2019, 25(10): 1975. doi: 10.3969/j.issn.1006-2084.2019.10.020 [21] 叶向阳, 邱林, 田晓菲, 等. 改良术式在单侧不完全性唇裂整复治疗的应用[J]. 重庆医科大学学报, 2016, 41(12): 1303. [22] 梁丽. 0-12岁汉族正常人群鼻腔形态及鼻唇发育的研究[D]. 重庆: 重庆医科大学, 2013. [23] 宋培军, 李建成, 张莉, 等. 改良Millard法修复单侧唇裂64例[J]. 实用医学杂志, 2017, 33(11): 1802. doi: 10.3969/j.issn.1006-5725.2017.11.021 -




 下载:
下载: