-
随着社会发展,人民生活水平飞速提高,生活方式不断变革,男性乳腺疾病的发病率与女性一样,几乎每年都在提高。其中,最常发生的2种疾病分别是恶性病变中的乳腺癌,以及良性病变中的男性乳腺发育症。男性乳腺癌的发病率仅占男性癌症的1%,约占全球所有乳腺癌的1%,且男性乳腺癌病人在公众意识和合理治疗决策方面落后于女性,乳腺癌文献、研究、临床试验和开发新的治疗方案主要侧重于女性乳腺癌,而男性与女性的生理结构方面有很大差异,所以这些以女性乳腺癌为对象的研究结果,并不能完全适用于男性乳腺癌[1-2]。故本研究收集了经全数字化乳腺钼靶摄影(full-field digital mammography,FFDM)检查并经病理证实的男性乳腺疾病21例及同时期女性乳腺癌65例,回顾性分析其临床、病理及FFDM检查资料,旨在为男性乳腺疾病的诊断提供一定依据。
-
收集2018年7月至2021年10月我院收治并取得病理结果(经穿刺或手术获得)的男性乳腺病变24例、女性乳腺癌68例。纳入标准:(1) 在获取病理结果前4周内行乳腺X线检查(所有病人均使用同一台设备检查);(2)病理结果完整且明确。排除标准:患侧乳腺的病变区域进行X线检查前有手术或放、化疗史;图像质量不佳或病灶显示不明确。严格按照标准筛选入组病例,本研究最终纳入21例男性乳腺病变及65例女性乳腺癌。
-
所有病人乳腺X线摄片均使用同一台,Siemens Mammomat Inspiration乳腺X线机。双侧乳腺均采用两种基本体位:头尾位(craniocaudol,CC)及内外斜位(mediolateral oblique,MLO)。
-
由2名放射诊断医生(均具备10年以上工作经验)在不知病理结果的情况下阅片,根据2013版美国放射学会(American College of Radiology,ACR)乳腺影像报告和数据系统(breast imaging reporting and data system,BI-RADS)标准,评价内容包括:病灶是否表现为肿块、局灶不对称影、结构扭曲、有无可疑恶性钙化、有无乳头凹陷、有无周围血管增粗(或增多)等;并将BI-RADS分类中,结果为3及4a类的病例设为阴性组(即良性倾向),将结果为4b、4c及5类的病例设为阳性组(即恶性倾向)。
-
采用t(或t′)检验、矫正χ2检验和确切概率法。
-
21例男性乳腺病变病人年龄34~88岁,平均(64.48±15.55)岁。其中良性病变组13例,年龄34~85岁,平均(59.62±15.48)岁;恶性病变组8例,年龄48~88岁,平均(72.38±12.84)岁。男性病人良恶性病变2组间的发病年龄比较,差异无统计学意义(P>0.05)。
65例女性病人年龄26~74岁,平均(50.46±9.96)岁,均为恶性病变。男性乳腺癌与女性乳腺癌2组间发病年龄比较,差异有统计学意义(t′=3.88,P < 0.01)。
-
21例男性乳腺病变中,良性13例,其中男性乳腺增生性病变7例,慢性炎症3例,乳头状瘤、脂肪瘤及良性叶状肿瘤各1例;恶性8例,均为浸润性导管癌,其中Luminal-A型3例,Luminal-B型2例,另3例未取得免疫组化结果。65例女性乳腺癌均为浸润性导管癌,其中Luminal-A型18例,Luminal-B型23例,非Luminal型24例。
-
男性乳腺恶性病变组病灶肿块以及有无周围血管增粗(或增多)发生率均高于良性病变组,局灶不对称影发生率低于良性病变组,差异均有统计学意义(P < 0.05);2组结构扭曲、乳头凹陷发生率比较,差异均无统计学意义(P>0.05)(见表 1)。
分组 n 肿块 局灶不对称影 血管增粗(或增多) 结构扭曲 乳头凹陷 恶性病变组 8 5(62.50) 3(37.50) 6(75.00) 4(50.00) 3(37.50) 良性病变组 13 1(7.69) 12(92.31) 2(15.38) 4(30.77) 4(30.77) P — 0.014* 0.014* 0.018* 0.645* 1.000* *示确切概率法 表 1 男性乳腺良恶性病变2组病人的FFDM图像特征比较[n; 百分率(%)]
-
男性乳腺癌组乳头凹陷发生率高于女性乳腺癌组,可疑恶性钙化发生率低于女性乳腺癌组,差异均有统计学意义(P < 0.05);2组肿块、局灶不对称影、周围血管增粗(或增多)、结构扭曲、肿块边缘模糊和肿块毛刺征发生率比较,差异均无统计学意义(P>0.05)(见表 2)。
分组 n 肿块 局灶不对称影 血管增粗(或增多) 结构扭曲 乳头凹陷 可疑恶性钙化 肿块边缘模糊 肿块毛刺征 男性乳腺癌组 8 5(62.50) 3(37.50) 6(75.00) 4(50.00) 3(37.50) 0(0.00) 1(12.50) 1(12.50) 女性乳腺癌组 65 37(56.92) 25(38.46) 23(35.38) 19(29.23) 5(7.69) 28(43.08) 30(46.15) 15(23.08) χ2 — 0.01* 0.01* 3.16* 0.62* — 3.92* 2.07* 0.05* P — >0.05 >0.05 >0.05 >0.05 0.04# < 0.05 >0.05 >0.05 *示矫正χ2值;#示确切概率法 表 2 男性乳腺癌与女性乳腺癌2组病人的FFDM图像特征比较[n; 百分率(%)]
-
ROC曲线下面积(AUC)为0.885、敏感度100%、特异性76.9%、符合率85.7%、阳性预测值72.7%、阴性预测值100%(见图 1)。
-
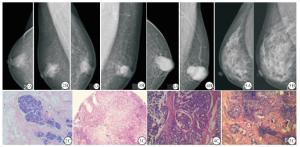
病人1,男,62岁,因右乳肿胀增大就诊,FFDM图像示右乳晕后区斑片样腺体影,术后病理男性乳腺发育(见图 2);病人2,男性,52岁,自觉左乳肿块伴疼痛不适,FFDM图像示左乳晕后区局灶不对称影,伴乳头轻度凹陷,术后病理乳腺慢性炎症(见图 3);病人3,男性,75岁,左乳质硬肿块数月,FFDM图像示左乳晕后区高密度肿块,形态不规则,边界较清伴明显分叶,周围血管增粗,术后病理浸润性乳腺癌(见图 4);病人4,女性,43岁,体检超声提示右乳结节,FFDM图像示右乳外上象限局灶不对称影,术后病理示浸润性乳腺癌(见图 5)。
-
男性因乳腺增大或乳腺区包块而就诊,大部分可能为良性病变,其中男性乳腺发育症最常见,其他良性病变还包括男性乳腺慢性炎症、脂肪瘤、导管内乳头状瘤等[3-5]。男性乳腺发育症,往往因为体内雌雄激素的比例不协调,或者因为乳腺组织对体内雌激素的敏感度增加,从而引起乳腺体和脂肪组织的发育异常或增生,是男性乳腺最普遍的良性疾病[6]。男性乳腺发育症在FFDM上多表现为乳腺体积增大、乳晕后的局灶不对称影,常分三型:树枝型、结节型和弥漫型。若双乳同时发生肿大、临床未触及明确肿块或触及肿块较柔软、活动度好,则有助于诊断。本研究中7例男性乳腺发育症,均为病人自觉单侧乳腺肿块,其中2例弥漫型及3例树枝型影像表现典型、诊断结果与病理一致,2例结节型表现类似于乳腺内占位性病变,尤其1例边缘可见分叶,且伴同侧乳腺血管影增多, 与乳腺癌表现较难以鉴别。
男性乳腺慢性炎性病变多源于毒力不强的细胞内感染,缺乏急性炎症典型的临床表现,病程较长、病情隐匿,常可伴不同程度的压痛表现,FFDM大多表现为局灶不对称影,如果局部伴有结构扭曲表现,或累及邻近皮肤、乳头形成凹陷,则仅从影像表现上与乳腺癌鉴别困难,易发生误诊。发生于乳腺区域的脂肪瘤因典型的脂肪样低密度特征,与其他乳腺病变所表现的等或高密度病灶有较显著差异,结合临床触诊扪及的质地柔软且常为扁圆形肿块表现,容易诊断。男性导管内乳头状瘤极罕见,国内文献也仅见于一些个案报道[7-8],其发生部位往往更贴近乳晕下,可表现为肿块或结节样,若临床出现血性溢液则更有助于本病的诊断。本研究中乳头状瘤1例,临床无溢液,FFDM表现为乳晕后区局灶不对称影伴有散在点状钙化,及轻度结构扭曲表现。乳腺叶状肿瘤是一种少见肿瘤,纤维上皮来源、生物学行为复杂,根据分化不同,可分良性、交界性及恶性。本研究中1例良性叶状肿瘤,FFDM表现为类圆形高密度肿块、边界较清、且直径 < 3 cm,与韦明珠等[9]的研究结果一致,而恶性或交界性叶状肿瘤多表现为形态不规则的分叶状肿块,边界大部分清楚或局部模糊,其表现与乳腺黏液癌等不易鉴别。
男性乳腺组织罕见小叶单元,主要为导管系统,因此男性乳腺癌更常见于导管类型[10],主要是浸润性导管癌,本研究中8例均为此型。男性乳腺癌发病率虽然很低,但是发病分期晚,无论组织学等级高或者低,其预后往往比女性乳腺癌都差[11-12],非常需要引起临床和大众的重视。
本研究中,男性乳腺癌病人发病年龄常较女性更大,平均发病、就诊的年龄要比女性乳腺癌病人迟约10年,这与男性乳腺生理与激素水平与高龄且绝经女性更接近的客观因素有关,也与男性对于乳腺癌的认识不足并羞于就医的社会心理原因有着一定的关系。
肿块是乳腺癌影像诊断中最常见的征象,由于肿瘤呈现浸润性的生长方式,且肿瘤各部分生长速度不一致,导致形态多不规则,边缘较模糊,部分可见毛刺。男性乳腺内没有丰富的纤维腺体组织作为背景,在低密度的脂肪组织的衬托下,男性乳腺癌肿块的境界往往显示得更清晰,边缘分叶征也更容易显示,本研究中5例男性乳腺癌可见肿块、形态不规则,边缘伴多个分叶,其中1例边缘毛刺征可见。与女性乳腺癌病人肿块边缘大多较模糊或者仅表现为局灶不对称影不同,男性乳腺的FFDM图像中即使所见肿块的境界清晰,诊断为乳腺癌的可能性仍然较大。
对于女性乳腺癌来说,可疑恶性钙化是仅次于肿块的另一主要诊断依据。最常出现在导管原位癌或原位癌伴浸润的病例中,同时在HER-2过表达型乳腺癌中的出现率也比较高。然而,男性乳腺癌主要分子亚型为Luminal型,大多表现为ER阳性、HER-2阴性[13-14]。相较于女性病人,男性病人病灶中钙化的发生比例并不高[15],且出现的钙化大多为良性表现,质地粗糙,数量少,分布散在,很少见线样或细杆状钙化。本研究中仅2例男性乳腺癌影像中可见钙化,均为典型良性表现,1例为散在分布粗糙颗粒钙化,另1例为集群分布点状钙化。
乳腺癌大多为富血供肿瘤,因此患侧乳腺、尤其是病灶周围会出现血管影的增粗(或增多),在不同性别的乳腺癌病人中均可见此征象,而病灶的大小与血供增加程度是否具有正相关性目前尚存在较大分歧。本研究中8例男性乳腺癌病人的FFDM图像有6例出现了不同程度的血管影增粗(或增多)的表现,病灶大小与血管影增粗(或增多)的程度尚无正相关性;而7例男性乳腺发育症病人图像中仅1例可见血管影增粗(或增多)的表现,另有1例男性乳腺慢性炎性病变可见此征象。由此可见,病变区血管影增粗(或增多)虽然常常提示恶性可能,但并非乳腺癌诊断的特有征象,它在男性乳腺癌与男性乳腺发育症的鉴别时往往有较大价值。患侧乳腺乳头凹陷常为病理原因所致,也可以是先天发育异常,男性乳腺癌病人出现乳头凹陷征象的概率显著高于女性病人,同时,此征象在男性乳腺良性病变中的发生率也并不低,这可能与男性乳腺体积小、病变与乳头、乳晕距离较近密切相关。
FFDM是目前应用最广泛的诊断乳腺疾病的影像检查方法,并成为早期发现乳腺癌的常规筛查方法[16]。美国放射学会对于常规体检不能明确良恶性的男性乳腺疾病病人,或者可疑乳腺癌的病人,均优先推荐乳腺X线摄影检查[17]。本研究结果也充分显示了FFDM在男性乳腺疾病诊断中具有良好的诊断效能,尤其在诊断男性乳腺癌时有较高的敏感度,与曾辉等[18]研究结果相符。
当然,本研究仍有局限性,如回顾性分析研究可能存在一定的偏倚性,且病例收集数量偏少。下一步我们不仅要扩大样本量,更要细化研究方向。
综上,FFDM能较清晰的显示出男性乳腺内的病变,良性病变中的脂肪瘤、良性叶状肿瘤及典型的男性乳腺发育症较易诊断,慢性炎性病变若邻近软组织受累出现结构扭曲表现,则病变性质常常不易判断。男性乳腺癌在诊断时应充分结合临床,尽量避免漏诊、误诊、延误病人的治疗。
全数字化乳腺钼靶摄影对男性乳腺病变良恶性的鉴别诊断
Value of the full-field digital mammography in the differential diagnosis of benign and malignant male breast lesion
-
摘要:
目的探讨全数字化乳腺钼靶摄影(full-field digital mammography,FFDM)对男性乳腺病变良恶性的鉴别诊断价值。 方法收集2018年7月至2021年10月经FFDM检查并取得病理结果的21例男性乳腺肿块病人及65例女性乳腺癌病人资料。回顾性分析其临床及影像学特征并进行比较,采用受试者工作特征性(ROC)曲线下面积(AUC)来评估FFDM对男性乳腺病变的诊断效能。 结果21例男性乳腺病变中良性13例,恶性8例。男性乳腺恶性病变组肿块以及有无周围血管增粗(或增多)发生率均高于良性病变组,局灶不对称影发生率低于良性病变组,差异均有统计学意义(P < 0.05);2组结构扭曲、乳头凹陷发生率比较,差异均无统计学意义(P>0.05)。男性乳腺癌组乳头凹陷发生率高于女性乳腺癌组,可疑恶性钙化发生率低于女性乳腺癌组,差异均有统计学意义(P < 0.05);2组肿块、局灶不对称影、周围血管增粗(或增多)、结构扭曲、肿块边缘模糊和肿块毛刺征发生率比较,差异均无统计学意义(P>0.05)。FFDM对于男性乳腺疾病诊断的AUC为0.885,敏感度100%,特异度76.9%,符合率85.7%,阳性预测值72.7%,阴性预测值100%。 结论FFDM对男性乳腺良恶性病变具有较好地诊断价值,肿块及周围血管增粗(或增多)是诊断男性乳腺癌最重要的影像表现,良性病变以男性乳腺发育最常见,多表现为局灶不对称影。 -
关键词:
- 全数字化乳腺钼靶摄影 /
- 乳腺病变 /
- 男性 /
- 鉴别诊断
Abstract:ObjectiveTo evaluate the value of full-field digital mammography(FFDM) in the differential diagnosis of benign and malignant male breast lesions. MethodsTwenty-one male patients with breast mass and 65 female breast cancer patients detected by FFDM and pathology from July 2018 to October 2021 were investigated.The clinical and radiographic features of all cases were retrospectively analyzed.The area under the receiver operating characteristic curve(AUC) was used to evaluate the differential diagnosis efficacy of FFDM for benign and malignant breast lesions. ResultsAmong the 21 cases, 13 cases were benign, and 8 cases were malignant.The incidence rates of mass and peripheral vascular thickening(or increase) in the male breast malignant lesions groups were higher than those in the benign lesions group, and the incidence rate of focal asymmetric shadow of which was lower than that in the benign lesions group(P < 0.05).There was no statistical significance in the incidence rate of structural distortion and nipple depression between two groups(P>0.05).The incidence rate of nipple depression in male breast cancer group was higher than that in female breast cancer group, and the incidence rate of suspected malignant calcification of which was lower than that in female breast cancer group(P < 0.05).The differences of the incidence rates of the mass, focal asymmetric shadow, peripheral vascular thickening(or increase), structural distortion, blurred mass margin and mass burr features between two groups were not statistically significant(P>0.05).The AUC of FFDM for the diagnosis of male breast disease was 0.885, and the sensitivity, specificity, incidence rate, positive predictive value and negative predictive value were 100%, 76.9%, 85.7%, 72.7% and 100%, respectively. ConclusionsFFDM has a good diagnostic value for benign and malignant male breast lesions.The mass and thickening(or increase) of peripheral blood vessels are the most important imaging findings in the diagnosis of male breast cancer.Male mammary gland development was the most common benign lesion, and the benign lesions are mostly manifested as focal asymmetric shadows. -
Key words:
- full-field digital mammography /
- breast lesion /
- male /
- differential diagnosis
-
表 1 男性乳腺良恶性病变2组病人的FFDM图像特征比较[n; 百分率(%)]
分组 n 肿块 局灶不对称影 血管增粗(或增多) 结构扭曲 乳头凹陷 恶性病变组 8 5(62.50) 3(37.50) 6(75.00) 4(50.00) 3(37.50) 良性病变组 13 1(7.69) 12(92.31) 2(15.38) 4(30.77) 4(30.77) P — 0.014* 0.014* 0.018* 0.645* 1.000* *示确切概率法 表 2 男性乳腺癌与女性乳腺癌2组病人的FFDM图像特征比较[n; 百分率(%)]
分组 n 肿块 局灶不对称影 血管增粗(或增多) 结构扭曲 乳头凹陷 可疑恶性钙化 肿块边缘模糊 肿块毛刺征 男性乳腺癌组 8 5(62.50) 3(37.50) 6(75.00) 4(50.00) 3(37.50) 0(0.00) 1(12.50) 1(12.50) 女性乳腺癌组 65 37(56.92) 25(38.46) 23(35.38) 19(29.23) 5(7.69) 28(43.08) 30(46.15) 15(23.08) χ2 — 0.01* 0.01* 3.16* 0.62* — 3.92* 2.07* 0.05* P — >0.05 >0.05 >0.05 >0.05 0.04# < 0.05 >0.05 >0.05 *示矫正χ2值;#示确切概率法 -
[1] GUCALP A, TRAINA TA, EISNER JR, et al. Male breast cancer: a disease distinct from female breast cancer[J]. Breast Cancer Res Treat, 2019, 173(1): 37. [2] FENTIMAN IS. The endocrinology of male breast cancer[J]. Endocr Relat Cancer, 2018, 25(6): R365. [3] 白佳媛, 何之彦. 男性乳腺肿块的乳腺X线分析及其临床意义[J]. 中国医学计算机成像杂志, 2014, 20(4): 321. doi: 10.3969/j.issn.1006-5741.2014.04.005 [4] 黄琰, 肖勤, 孙轶群, 等. 乳腺MRI鉴别诊断男性乳腺良恶性病变的价值[J]. 中华放射学杂志, 2021, 55(1): 48. doi: 10.3760/cma.j.cn112149-20200228-00286 [5] 刘畅, 于韬, 邬晓明, 等. 男性乳腺肿块的超声诊断及其临床意义[J]. 现代肿瘤医学, 2018, 26(18): 2956. doi: 10.3969/j.issn.1672-4992.2018.18.032 [6] ZAVLIN D, JUBBAL KT, FRIEDMAN JD, et al. Complications and outcomes after gynecomastia surgery: Analysis of 204 pediatric and 1 583 adult cases from a National Multi center Database[J]. Aesthet Plast Surg, 2017, 41(4): 761. [7] 薛双峰, 段秀庆. 男性乳腺导管内乳头状瘤伴不典型增生1例[J]. 临床普外科电子杂志, 2013(2): 62. [8] 唐鹤文, 朱庆莉, 姜玉新. 男性乳腺导管内乳头状瘤超声表现一例[J/CD]. 中华医学超声杂志(电子版), 2017, 14(9): 719. [9] 韦明珠, 顾雅佳, 肖勤, 等. 不同病理类型的乳腺分叶状肿瘤影像特征分析[J]. 中国医学计算机成像杂志, 2013, 19(3): 217. doi: 10.3969/j.issn.1006-5741.2013.03.007 [10] JYLLING AMB, JENSEN V, LELKAITIS G, et al. Male breast cancer: clinicopathological characterization of a National Danish cohort 1980-2009[J]. Breast Cancer, 2020, 27(4): 683. [11] 李玉胜, 许磊, 孙岩峰, 等. 男性乳腺癌与女性乳腺癌的预后影响因素探讨[J]. 蚌埠医学院学报, 2019, 44(5): 610. [12] WANG X, LIU S, XUE Y. Clinicopathological features and prognosis of male breast cancer[J]. J Int Med Res, 2021, 49(10): 3000605211049977. [13] KHAN NAJ, TIRONA M. An updated review of epidemiology, risk factors, and management of male breast cancer[J]. Med Oncol, 2021, 38(4): 39. [14] CARDOSO F, BARTLETT JMS, SLAETS L, et al. Characterization of male breast cancer results of the EORTC 10085/TBCRC/BIG/NABCG international male breast cancer program[J]. Ann Oncol, 2018, 29(2): 405. [15] 张晓东, 陈卉品, 张凤, 等. 男性乳腺癌超声及临床病理学表现[J]. 中国医学影像技术, 2021, 37(8): 1173. [16] JIANG X, ZOU X, SUN J, et al. A nomogram based on radiomics with mammography texture analysis for the prognostic prediction in patients with triple-negative breast cancer[J]. Contrast Media Mol Imaging, 2020, 2020: 5418364. [17] MAINIERO BI, LOURENCO AP, BARKE LD, et al. ACR appropriateness criteria evaluation of the symptomatic male breast[J]. J Am Coll Radiol, 2018, 15(11S): S313. [18] 曾辉, 徐泽园, 曾凤霞, 等. 数字乳腺X线摄影: 男性乳腺疾病诊断的推荐检查可行性分析[J]. 医学影像学杂志, 2022, 32(1): 42. -





 下载:
下载: