-
中枢神经系感染是小儿常见病和多发病,尤其以病毒性脑炎多见,严重的患儿会遗留不同程度的中枢神经系统损伤, 对日后的生活及学习能力产生严重影响,因此早期诊断和治疗非常重要。研究[1]显示脑脊液基质金属蛋白酶(MMPs)可改变血脑屏障通透性,增加致病菌或其他有害物质对脑组织损害风险,在病毒性脑炎的发生和发展过程中起到了关键的作用。本研究将临床收治的病毒性脑炎患儿,根据脑脊液检验结果分为脑脊液异常组和脑脊液正常组,留取急性期(入院72 h内)和恢复期(治疗1周后)的脑脊液和静脉血,检测MMP-2和MMP-9水平,通过与脑脊液细胞数相关性分析,来判断脑脊液和静脉血MMPs数值对临床诊断的影响。现作报道。
-
选取2018年10月至2020年11月我科住院40例病毒性脑炎患儿,根据诸福棠实用儿科学第九版诊断标准纳入本研究。年龄1~14岁。所有入组患儿入院时均有不同程度的发热、呕吐、头痛以及伴有惊厥和嗜睡甚至昏迷等意识障碍表现,脑电图均有典型的慢波表现。根据脑脊液检验结果分为脑脊液异常组和脑脊液正常组,各20例,其中异常组男13例,女7例;正常组男10例,女10例。其中脑脊液异常组中重症患儿3例,惊厥患儿8例,其中1例持续惊厥状态,嗜睡患儿7例;脑脊液正常组惊厥患儿3例,嗜睡患儿5例。所有入院患儿于入院72 h内采集脑脊液和外周血,并完善血常规、生化常规、C反应蛋白(CRP)检查。
-
脑脊液异常组患儿于病毒性脑炎急性期(入院72 h内)和恢复期(治疗1周后)留取脑脊液1 mL和外周血2 mL,脑脊液正常组患儿于病毒性脑炎急性期(入院72 h内)留取脑脊液1 mL和外周血2 mL,室温下分别于3 000 r/min离心15 min后留取上清液冻存于-20 ℃医用冰箱。同时记录患儿入院前3 d体温,送检72 h内血常规、生化常规、CRP以及1周后血常规、生化常规、CRP,并记录住院时间。
-
脑脊液和血清于室温下解冻后使用双抗夹心ELISA试剂盒(美国R&D)检测MMP-2和MMP-9水平, 按照试剂盒提供的说明书进行严格操作。
-
采用t检验、Pearson相关分析和ROC曲线分析。
-
2组年龄、性别、血常规、生化常规、CRP等一般资料差异无统计学意义(P>0.05),2组脑脊液中的白细胞数和乳酸差异均有统计学意义(P < 0.01)。且2组住院时间差异亦有统计学意义(P < 0.05)。而进一步对脑脊液和外周血中的MMPs蛋白分析发现,2组外周血和脑脊液中的MMP-2、MMP-9差异均有统计学意义(P < 0.05~P < 0.01)(见表 1)。
一般资料 脑脊液异常组
(n=20)脑脊液正常组
(n=20)t P 年龄/岁 5.75±3.37 5.46±4.97 0.22 >0.05 男 13 10 0.92# >0.05 脑脊液白细胞数/(个/毫升) 82.20±61.55 3.35±3.15 5.72 < 0.01 脑脊液乳酸/(mmol/L) 1.81±0.55 1.34±0.27 3.43* < 0.01 脑脊液白蛋白/(g/L) 0.36±0.21 0.32±0.30 0.49 >0.05 体温/℃ D1 37.93±0.85 37.80±1.16 0.40 >0.05 D2 37.71±0.84 37.52±0.88 0.70 >0.05 D3 37.22±0.55 37.11±0.49 0.67 >0.05 降钙素原/(ng/mL) 0.23±0.27 0.45±0.63 1.02 >0.05 CRP/(mg/L) 6.54±9.59 16.40±21.30 1.89 >0.05 外周血白蛋白/(g/L) 41.72±2.62 40.46±5.31 0.95* >0.05 血肌酐/(μmol/L) 39.79±10.78 35.00±12.94 1.27 >0.05 血尿素氮/(mmol/L) 3.33±0.94 3.74±1.03 1.31 >0.05 丙氨酸氨基转移酶/(U/L) 18.85±8.23 23.20±14.98 1.14* >0.05 天门冬氨酸氨基转移酶/(U/L) 36.65±26.95 36.10±17.34 0.08 >0.05 住院时间/d 16.45±13.61 9.10±3.31 2.35* < 0.05 外周血MMP-2/(μg/L) 871.80±137.69 675.30±143.08 4.43 < 0.01 外周血MMP-9/(μg/L) 245.35±52.36 202.05±52.49 2.61 < 0.05 脑脊液MMP-2/(μg/L) 103.70±13.15 72.15±14.17 7.30 < 0.01 脑脊液MMP-9/(μg/L) 74.15±7.58 52.30±8.57 8.54 < 0.01 *示t′值;#示χ2值 表 1 2组一般资料比较(x±s)
-
结果显示, 外周血中的MMP-2、MMP-9和脑脊液WBC呈明显正相关关系(r=0.732、0.695, P < 0.01)。脑脊液MMP-2、MMP-9和脑脊液WBC呈明显正相关关系(r=0.827、0.775, P < 0.01)。
-
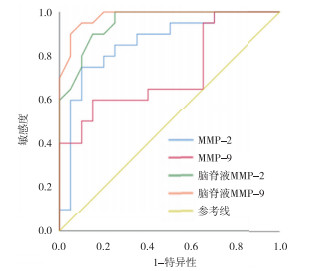
外周血中的MMP-2、MMP-9对脑脊液细胞数的灵敏度和特异度分析显示,ROC曲线下面积(AUC)分别为0.860和0.725(P < 0.01和P < 0.05);脑脊液MMP-2、脑脊液MMP-9对脑脊液细胞数的灵敏度和特异度分析显示,AUC分别为0.950和0.980(P < 0.01)(见表 2、图 1)。
指标 AUC P 灵敏度 特异度 cutoff值 阳性预测值/% 阴性预测值/% 外周血 MMP-2 0.860 < 0.01 0.75 0.90 778.5 88.24 78.26 MMP-9 0.725 < 0.05 0.60 0.85 252.0 80.00 68.00 脑脊液 MMP-2 0.950 < 0.01 0.90 0.85 97.0 92.86 73.08 MMP-9 0.980 < 0.01 0.90 0.95 65.5 94.74 90.48 表 2 外周血和脑脊液中MMP2/MMP-9对脑脊液细胞数的灵敏度和特异度分析
-
中枢神经系统感染中的病毒性脑炎临床上分为脑膜炎和脑炎[2],因为感染的病毒种属不同及个体差异轻重程度不一,疾病的急性期由普通的头疼呕吐到高热抽搐昏迷以及恢复期重症,患儿会遗留不同程度的神经系统后遗症,如癫痫、瘫痪、智力水平下降等[3]。
该病对临床的早期识别和诊断提出了很高的要求,脑脊液检查对确诊及鉴别诊断有重要意义,尤其是早期及时完善腰椎穿刺检查[4]。典型病毒性脑炎患儿的脑脊液白细胞数轻度增高,分类以淋巴细胞为主,蛋白轻度升高或正常,糖和氯化物通常正常[5]。但因为重症患儿对穿刺的耐受性降低以及急性期患儿因显著颅内压增高,会增加脑疝的风险,加之家属的配合程度降低,使得临床及时完善腰穿检查比较困难。
国外很多关于中枢神经系统感染的研究都把目光对准了MMPs[6],在动物实验[7]和临床研究[8]中均发现MMPs与中枢神经系统感染密切相关,可能是因为MMPs能降解血管基底膜的Ⅳ型胶原蛋白,破坏血脑屏障,使T细胞顺利通过血脑屏障到达大脑[9]。MMPs具有修复、重建、促进局部血管形成等作用,且可激活颅内炎症反应[10-11]。根据作用底物和片段同源性将MMPs分为6类,临床最常用的是MMP-2和MMP-9。脑脊液中MMP-2和MMP-9已经被认为是作为中枢神经系统感染的炎症标志物[12-14]。
本研究结果显示,2组外周血和脑脊液中MMP-2、MMP-9之间均存在差异。国外已有临床实验结果表明,病毒感染导致脑炎后脑脊液中MMP-2和MMP-9的表达上调[1-2]。本研究和国外研究结果一致。随着疾病进展,病毒性脑炎组患儿血清MMP-2和MMP-9水平显著高于正常组,本研究数据也印证了该观点。我们进一步分析发现,外周血中MMP-2、MMP-9和脑脊液白细胞数呈正相关关系。脑脊液中的MMP-2、MMP-9和脑脊液白细胞数也呈正相关关系。使用外周血MMP-2、MMP-9来判断脑脊液的感染程度,进一步分析外周血中MMP-2、MMP-9对脑脊液细胞数的灵敏度和特异度发现外周血MMP-2、MMP-9水平可以反映脑脊液中MMP-2、MMP-9水平。这为临床早期诊断和识别病毒性脑炎提供了一条新的思路。
基质金属蛋白酶水平对病毒性脑炎患儿早期诊断的临床价值
Clinical value of the matrix metalloproteinase level in early diagnosis of viral encephalitis in children
-
摘要:
目的通过分析病毒性脑炎患儿脑脊液和血清基质金属蛋白酶(MMPs)水平与脑脊液白细胞的相关性来预测MMPs在病毒性脑炎早期诊断的价值。 方法选择确诊为病毒性脑炎的住院患儿40例,通过ELISA法检测脑脊液细胞数异常患儿(20例)和脑脊液细胞数正常患儿(20例)血清和脑脊液中MMP-2和MMP-9水平。 结果2组外周血和脑脊液中的MMP-2、MMP-9差异有统计学意义(P < 0.05~P < 0.01)。外周血中的MMP-2、MMP-9和脑脊液白细胞数呈明显正相关关系(P < 0.01)。脑脊液中的MMP-2、MMP-9和脑脊液白细胞数亦呈明显正相关关系(P < 0.01)。外周血中的MMP-2、MMP-9对脑脊液细胞数的灵敏度和特异度分析显示,曲线下面积分别为0.860和0.725(P < 0.01和P < 0.05);脑脊液中的MMP-2、MMP-9对脑脊液细胞数的灵敏度和特异度分析显示,曲线下面积分别为0.950和0.980(P < 0.01)。 结论外周血的MMP-2、MMP-9水平可以反映脑脊液中MMP-2、MMP-9水平,可以作为病毒性脑炎的生物标志物,成为早期诊断的预测因子。 Abstract:ObjectiveTo predict the value of matrix metalloproteinases(MMPs) in the early diagnosis of viral encephalitis by analyzing the correlation between the serum levels of MMPs and white blood cells in cerebrospinal fluid(CSF) of children with viral encephalitis. MethodsForty hospitalized children with viral encephalitis were selected.The serum and CSF levels of MMP-2 and MMP-9 were detected by ELISA in 20 children with abnormal CSF cell count and 20 children with normal CSF cell count. ResultsThe differences of the levels of MMP-2 and MMP-9 in peripheral blood and CSF between two groups were statistically significantly(P < 0.05 to P < 0.01).The serum levels of MMP-2 and MMP-9 in peripheral blood were positively correlated with the number of white blood cells in CSF(P < 0.01).The levels of MMP-2 and MMP-9 in CSF were positively correlated with the number of white blood cells in CSF(P < 0.01).The sensitivity and specificity of MMP-2 and MMP-9 in peripheral blood to the number of CSF cells showed that the area under the curve was 0.860 and 0.725, respectively(P < 0.01 and P < 0.05).The sensitivity and specificity analysis of MMP-2 and MMP-9 in CSF to the number of CSF cells showed that the area under the curve was 0.950 and 0.980, respectively(P < 0.01). ConclusionsThe levels of MMP-2 and MMP-9 in peripheral blood can reflect the concentrations of MMP-2 and MMP-9 in CSF, which can be used as biomarkers of viral encephalitis and predictors of early diagnosis. -
Key words:
- viral encephalitis /
- matrix metalloproteinases /
- cerebrospinal fluid
-
表 1 2组一般资料比较(x±s)
一般资料 脑脊液异常组
(n=20)脑脊液正常组
(n=20)t P 年龄/岁 5.75±3.37 5.46±4.97 0.22 >0.05 男 13 10 0.92# >0.05 脑脊液白细胞数/(个/毫升) 82.20±61.55 3.35±3.15 5.72 < 0.01 脑脊液乳酸/(mmol/L) 1.81±0.55 1.34±0.27 3.43* < 0.01 脑脊液白蛋白/(g/L) 0.36±0.21 0.32±0.30 0.49 >0.05 体温/℃ D1 37.93±0.85 37.80±1.16 0.40 >0.05 D2 37.71±0.84 37.52±0.88 0.70 >0.05 D3 37.22±0.55 37.11±0.49 0.67 >0.05 降钙素原/(ng/mL) 0.23±0.27 0.45±0.63 1.02 >0.05 CRP/(mg/L) 6.54±9.59 16.40±21.30 1.89 >0.05 外周血白蛋白/(g/L) 41.72±2.62 40.46±5.31 0.95* >0.05 血肌酐/(μmol/L) 39.79±10.78 35.00±12.94 1.27 >0.05 血尿素氮/(mmol/L) 3.33±0.94 3.74±1.03 1.31 >0.05 丙氨酸氨基转移酶/(U/L) 18.85±8.23 23.20±14.98 1.14* >0.05 天门冬氨酸氨基转移酶/(U/L) 36.65±26.95 36.10±17.34 0.08 >0.05 住院时间/d 16.45±13.61 9.10±3.31 2.35* < 0.05 外周血MMP-2/(μg/L) 871.80±137.69 675.30±143.08 4.43 < 0.01 外周血MMP-9/(μg/L) 245.35±52.36 202.05±52.49 2.61 < 0.05 脑脊液MMP-2/(μg/L) 103.70±13.15 72.15±14.17 7.30 < 0.01 脑脊液MMP-9/(μg/L) 74.15±7.58 52.30±8.57 8.54 < 0.01 *示t′值;#示χ2值 表 2 外周血和脑脊液中MMP2/MMP-9对脑脊液细胞数的灵敏度和特异度分析
指标 AUC P 灵敏度 特异度 cutoff值 阳性预测值/% 阴性预测值/% 外周血 MMP-2 0.860 < 0.01 0.75 0.90 778.5 88.24 78.26 MMP-9 0.725 < 0.05 0.60 0.85 252.0 80.00 68.00 脑脊液 MMP-2 0.950 < 0.01 0.90 0.85 97.0 92.86 73.08 MMP-9 0.980 < 0.01 0.90 0.95 65.5 94.74 90.48 -
[1] KOLB SA, LAHRTZ F, PAUL R, et al. Matrix metalloproteinases and tissue inhibitors of metalloproteinases in viral meningitis: upregulation of MMP-9 and TIMP-1 in cerebrospinal fluid[J]. J Neuroimmunol, 1998, 84(2): 143. doi: 10.1016/S0165-5728(97)00247-6 [2] COSTA BKD, SATO DK. Viral encephalitis: a practical review on diagnostic approach and treatment[J]. J Pediatr(Rio J), 2020, 96(1): 12. [3] SUN SZ, WANG L, WU YE, et al. Aciclovir CSF concentration in children with viral encephalitis: is it adequate?[J]. J Antimicrob Chemother, 2018, 73(9): 2582. doi: 10.1093/jac/dky217 [4] VENKATESAN A, MURPHY OC. Viral encephalitis[J]. Neurol Clin, 2018, 36(4): 705. doi: 10.1016/j.ncl.2018.07.001 [5] AI J, XIE Z, LIU G, et al. Etiology and prognosis of acute viral encephalitis and meningitis in Chinese children: a multicentre prospective study[J]. BMC Infect Dis, 2017, 17(1): 494. doi: 10.1186/s12879-017-2572-9 [6] LIND L, ERIKSSON K, GRAHN A. Chemokines and matrix metalloproteinases in cerebrospinal fluid of patients with central nervous system complications caused by varicella-zoster virus[J]. J Neuroinflammation, 2019, 16(1): 42. doi: 10.1186/s12974-019-1428-1 [7] TOFT-HANSEN H, BABCOCK AA, MILLWARD JM, et al. Downregulation of membrane type-matrix metalloproteinases in the inflamed or injured central nervous system[J]. J Neuroinflammation, 2007, 4(20): 24. [8] SULIK A, WOJTKOWSKA M, OLDAK E. Elevated levels of MMP-9 and TIMP-1 in the cerebrospinal fluid of children with echovirus type 30 and mumps meningitis[J]. Scand J Immunol, 2010, 68(3): 323. [9] KARAMANOS NK, THEOCHARIS AD, NEILL T, et al. Matrix modeling and remodeling: a biological interplay regulating tissue homeostasis and diseases[J]. Matrix Biol, 2019, 75(76): 1. [10] HANNOCKS MJ, ZHANG X, GERWIEN H, et al. The gelatinases, MMP-2 and MMP-9, as fine tuners of neuroinflammatory processes[J]. Matrix Biol, 2019, 75(76): 102. [11] VAFADARI B, SALAMIAN A, KACZMAREK L. MMP-9 in translation: from molecule to brain physiology, pathology, and therapy[J]. J Neurochem, 2016, 139(2): 91. [12] SONG J, WU C, KORPOS E, et al. Focal MMP-2 and MMP-9 activity at the blood-brain barrier promotes chemokine-induced leukocyte migration[J]. Cell Rep, 2015, 10(7): 1040. [13] GERWIEN H, HERMANN S, ZHANG X, et al. Imaging matrix metalloproteinase activity in multiple sclerosis as a specific marker of leukocyte penetration of the blood-brain barrier[J]. Sci Transl Med, 2016, 8(364): 364ra152. [14] IVAN DC, WALTHERT S, BERVE K, et al. Dwellers and trespassers: mononuclear phagocytes at the borders of the central nervous system[J]. Front Immunol, 2021, 11(5): 609921. -





 下载:
下载: