-
脑脊液由侧脑室的脉络丛不断产生,并通过脑室系统及蛛网膜下腔形成一个动态的、具有复杂的转运及吸收机制的循环过程。近年来,磁共振相衬成像(phase-contrast magnetic resonance imaging, PC-MRI)作为一项新兴非侵入性检查在脑脊液流动评价中有所应用,推动了脑脊液循环的病理生理学研究,并拓宽了对其流动机制的认识[1]。ChiariⅠ型畸形(Chiari malformation type Ⅰ, CMⅠ)是一组临床表现与枕骨大孔区脑脊液循环受阻严重程度密切相关的疾病,其中50%~70%病人合并脊髓空洞症[2]。后颅窝减压是其主要治疗方式,有研究[3]表明病人颅颈区脑脊液的双向流动与正常人对比具有较大差异,其术后临床症状的缓解与脑脊液循环的改善及枕大池扩大密切相关。本研究通过比较健康志愿者及CMⅠ伴脊髓空洞症病人手术前后脑脊液流动特点,并结合芝加哥Chiari畸形预后量表(Chicago Chiari outcome scale, CCOS)进一步分析PC-MRI技术在其临床诊断治疗和预后评估中的应用价值。现作报道。
-
选取2018年9月至2019年10月入住我科的CMⅠ伴脊髓空洞症病人17例,均行后颅窝手术减压。其中男6例,女11例,年龄41~66岁,手术前和术后12个月均行PC-MRI检查。纳入标准:CMⅠ诊断明确,头痛加重、症状影响日常生活且伴随脊髓空洞症存在,满足手术减压指征。排除伴有脑积水、心律不齐以及既往有CMⅠ手术减压史病人。所有病人均进行术前病史、体检、颅脑和脊髓的常规磁共振及仰卧位颅颈交界区的磁共振电影成像检查。同期招募正常志愿者16名作为对照组,男8名,女8名,年龄40~70岁。所有检查均获取被检者知情同意且通过机构伦理委员会审批。
-
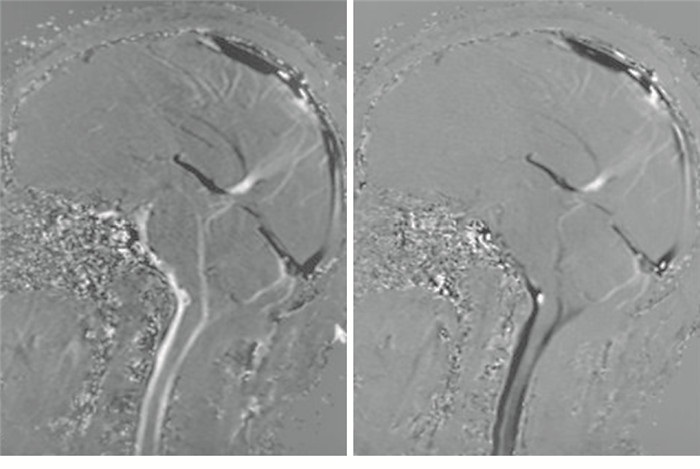
针对病人分别于术前4~8 d及减压后12个月行PC-MRI检查,对照组中每个志愿者仅接受一次PC-MRI检查。应用飞利浦MR Intera 3.0T设备进行扫描,被检者安静休息后呼吸、心率及脉搏平稳时,以后颅窝及颅颈交界区为中心,仰卧位应用快速自旋回波序列(CSF_DRIVE)对其进行T2W1成像作为参照定位,扫描参数如下:TR/TE 1 600/200 ms,视野230 mm×230 ms,矩阵420×393,层厚1 mm。于指脉门控下再行矢状位PC-MRI序列扫描观测脑脊液动态变化,扫描参数:TR/TE 21/7.8 ms(视病人心率对TR进行微调),视野250 mm×226 mm,矩阵248×172,层厚4 mm,翻转角度10°,编码方向为由头至足,主要针对中脑导水管中央段、第四脑室出口段及第二颈椎水平进行扫描,编码流速分别设定为10 cm/s、5 cm/s、15 cm/s。在相衬图像中,高信号表示脑脊液的足向运动,而低信号表示头向脑脊液流动,信号强度代表脑脊液的流动速度(见图 1),经Extended MR WorkSpace R2.6.3.1中MRV Qflow软件由神经放射科医师对感兴趣区(region of interest, ROI)进行勾画,生成相应区域的脑脊液流速、流量等资料,主要进行分析记录的数据包括中脑导水管中央段脑脊液净流量、一个心动周期内脑脊液流经ROI的总流量(冲程流量)、收缩期峰流速、舒张期峰流速、脑脊液流速到达收缩期峰值时间所占一个完整心动周期时间的比值(时间比),以及第四脑室出口段、第二颈椎水平腹侧脑脊液收缩期及舒张期峰流速。
-
采用t(或t′)检验。
-
CMⅠ组病人中脑导水管中央段脑脊液净流量和冲程流量均明显低于对照组(P < 0.01),此处收缩期脑脊液流速到达最大值时间较对照组明显延迟(P < 0.01),三处脑脊液收缩期及舒张期峰值流速均高于对照组(P < 0.05~P < 0.01)(见表 1)。
分组 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) CMⅠ组 17 2.24±0.75 55.71±12.28 5.69±0.79 34.44±5.49 6.83±0.69 1.79±0.24 1.93±0.33 4.30±1.19 8.98±2.16 对照组 16 9.06±2.02 74.38±12.64 5.05±0.89 29.19±3.78 6.07±0.61 1.48±0.34 1.48±0.36 3.43±1.16 6.73±2.08 t — 12.71* 4.30 2.19 3.18 3.34 3.04 3.75 2.12 3.04 P — < 0.01 < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 < 0.01 < 0.05 < 0.01 *示t′值 表 1 CMⅠ组与对照组脑脊液流动参数比较(x±s)
-
PC-MRI提示,CMⅠ病人术后中脑导水管处脑脊液净流量及冲程流量均较术前明显上升(P < 0.01),导水管处脑脊液到达处收缩期峰值时间明显缩短(P < 0.01),且各处脑脊液收缩期及舒张期最大流速较术前明显降低(P < 0.01)(见表 2)。
时间 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) 术前 17 2.24±0.75 55.71±12.28 5.69±0.79 34.44±5.49 6.83±0.69 1.79±0.24 1.93±0.33 4.30±1.19 8.98±2.16 术后 17 6.94±2.33 80.41±14.92 4.60±0.82 30.28±5.97 5.52±0.62 1.26±0.22 1.41±0.30 3.00±1.00 6.63±1.68 t — 7.92* 5.27 3.95 2.11 5.82 6.71 4.81 3.45 3.54 P — < 0.01 < 0.01 < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 *示t′值 表 2 CMⅠ病人手术前后脑脊液流动各项参数比较(x±s)
-
根据CCOS评分对CMⅠ病人预后进行评估,以10分为分界点[4]将病人分为预后较好组(CCOS评分>10分)12例和预后较差组(CCOS≤10分)5例。预后较好病人中脑导水管中段脑脊液术后净流量及冲程流量较术前增加量均明显高于预后较差者(P < 0.01),此处脑脊液到达收缩期峰值时间也较预后较差者明显缩短(P < 0.01),中脑导水管中段、第二颈椎腹侧脑脊液收缩期及舒张期峰流速均明显低于预后较差者(P < 0.05~P < 0.01),而2组四脑室出口段脑脊液峰流速差异无统计学意义(P>0.05)(见表 3)。
CCOS评分/分 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) >10 12 6.00±0.95 32.17±7.71 4.23±0.65 26.72±2.12 5.22±0.45 1.20±0.22 1.36±0.31 2.66±0.89 5.97±1.28 ≤10 5 1.60±1.14 6.80±3.96 5.48±0.41 38.83±0.94 6.24±0.31 1.41±0.15 1.54±0.28 3.83±0.82 8.22±1.52 t — 8.23 6.90 3.94 12.11 4.59 1.94 1.12 2.52 3.14 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 >0.05 >0.05 < 0.05 < 0.01 表 3 不同预后病人脑脊液流动各项参数比较(x±s)
-
PC-MRI作为一项新兴技术,可通过对脑脊液运动速度及方向进行测量分析,实现对其流动特点的定量研究。检查与测量中的影响因素众多,包括编码速度的差异,测量层面的选择,不同测量者对ROI的绘制误差,受检者的脑组织顺应性及其呼吸、血压、心率的影响。为保证稳定性,对于能够配合的人,在安静休息后,平静呼吸状态下完成扫描,不能配合者则先予以药物镇静再进行扫描。针对ROI的绘制,在幅度图像的选择上应注意流出道中脑脊液与周围组织的对比度和脑脊液流出信号强度,找出最佳截断面,绘制ROI面积时应尽量贴近流出道管腔壁,同时需避免过度紧靠引起误差。由于ROI面积对流量具有较大影响,而对于第四脑室下端,第二颈椎腹侧的ROI面积绘制存在较大差异,因此本研究中未对第四脑室下端及第二颈椎腹侧水平脑脊液流量进行定量分析。流速编码是磁共振电影检查的一个关键参数,它直接限制了最大编码速度,预设值偏低会引起信号混杂,导致测量结果不准确,而速度编码过高会导致从流动中获取的信号和信噪比降低,因此,预设的编码速度通常应略高于被研究流体的真实流速,采取牺牲小部分的信噪比来保证测量结果的准确性。研究[5]发现,正常人枕骨大孔区脑脊液平均峰流速约为3.6 cm/s,有研究[1]建议在枕骨大孔区脑脊液的速度编码值设定为10 cm/s,脑脊液通过中脑导水管的速度编码值设定为8 cm/s,在某些病理条件下,如中导水管狭窄时,由于狭窄区流速较高,则需要选择高于一般情况下的流速编码值。国内报道[6]研究正常人C2~3椎间盘水平脑脊液流动特点,建议针对颈椎椎管内脑脊液流速的测量,编码流速设置在15~20 cm/s最为适宜。本研究中,中脑导水管中央段、第四脑室出口段及第二颈椎水平进行扫描,编码流速分别设定为10、5、15 cm/s。
对于CMⅠ病人,脑脊液动力学监测可为其病理生理、发病机制的探索提供更直观的证据,其脑脊液在颅颈区仍呈双向性流动,但具有较大的差异,且前后流动不均衡,而由于该区域脑脊液流出道狭窄引起的管道效应使得脑脊液平均峰流速明显高于正常人,但仍难以代偿受挤压缩窄的横截面积,因此脑脊液的流出量依旧是降低的[7]。对于症状严重的病人,枕下开颅减压可有效改善脑脊液循环并阻止病情进展,相衬磁共振成像的应用通常也作为评估CMⅠ病人手术效果的手段之一[8]。QUON等[3]通过对比研究18例CMⅠ病人术前术后脑脊液动力学变化,发现临床症状的缓解与枕大池的扩大以及脑脊液循环改善具有相关性。对于伴有脊髓空洞症的病人,最常见于C2~3、C3~4椎间盘处。LINGE等[9]研究推测其引起脊髓空洞的主要原因在于该颈椎间盘水平脑脊液压力梯度相差最大。陆笑非等[10]通过探索30例CMⅠ伴脊髓空洞症的病人枕大池成形手术前后脑脊液动力学改变,发现解除小脑扁桃体对硬膜的压迫后,不仅临床症状得到改善,脊髓空洞明显变小,且脑脊液流速较术前明显降低且流量增加,特别是C2~3水平。据此推断,枕骨大孔区的不完全阻塞是脊髓空洞形成的重要病因。在本次研究中,病人脑脊液在中脑导水管中央段、四脑室出口段及第二颈椎腹侧的流动总体呈双向性,四脑室处脑脊液流动复杂多变,推测可能与湍流形成有关,测得各处平均峰流速均明显高于正常志愿者,且脑脊液流出量降低,术后病人的脑脊液流速及流量较术前存在明显改善,在之后的随访中,将预后结局不同的病人根据CCOS评分进行分组后发现,12例CCOS评分较高的病人术后症状明显改善,脊髓空洞也同样较术前缩小,5例评分较低者仍存在头痛、感觉障碍等症状,脊髓空洞改变均不明显,而PC-MRI检查中,预后较好的病人其术后及术前的脑脊液流量差值总体较预后不佳的病人明显高,且中脑导水管中央段、第二颈椎腹侧脑脊液峰流速也较后者有着更为显著的改善,这与CCOS评分结果具有一致性,进一步证实了脑脊液动力学的改善与临床结局具有很强的相关性,可与CCOS评分协同评估病人预后。但对于四脑室出口处脑脊液流动,预后不同的病人并无明显差异,这可能受限于研究中随访的病例数量,有待多诊疗中心大数据进一步验证。
脑脊液循环是一个动态的且具有复杂的转运及吸收机制的过程,依然是目前研究的热点主题,PC-MRI的应用对CMⅠ的疾病特点、诊断治疗及预后评估具有开创性意义,且随着三维相衬技术的出现,可显示出脑脊液多方向的运动,具有更高的空间分辨率,存在巨大的潜在应用价值,在经过大量研究反复验证之后,必将进一步推动脑脊液循环动力学研究,在临床上为病人制定最佳的诊疗方案提供可靠依据。
应用磁共振相衬技术对ChiariⅠ型畸形合并脊髓空洞症的脑脊液动力学研究
Study on the applicaton value of the PC-MRI on the cerebrospinal fluid dynamics in Chiari malformation type Ⅰ complicated with syringomyelia
-
摘要:
目的应用磁共振相衬技术评估脑脊液动力学改变对ChiariⅠ型畸形脑脊液动力学的影响。 方法选取ChiariⅠ型畸形合并脊髓空洞症病人17例(CMⅠ组)和同期健康志愿者16名(对照组)为研究对象,病人均行后颅窝减压术,并于术前及术后12个月分别针对颅颈交界区行磁共振相衬技术检查,志愿者仅检查一次,分析中脑导水管中央段、第四脑室出口段及第二颈椎水平脑脊液流速、流量等参数的改变。 结果与对照组比较,CMⅠ组病人各被检处脑脊液峰流速均增快(P < 0.05~P < 0.01),且总体流量减少(P < 0.01)。病人术后各处流速较术前明显变缓(P < 0.01),流量增加(P < 0.01)。不同预后病人的中脑导水管中段脑脊液流量、流速和第二颈椎腹侧脑脊液流速差异均有统计学意义(P < 0.05~P < 0.01)。 结论Chiari畸形Ⅰ型伴脊髓空洞症病人存在脑脊动力学变化,表现为脑脊液流动受阻,而脑脊液动力学的改善与病人预后具有相关性,应用磁共振相衬技术监测脑脊液动力学变化有助于评估病人预后。 -
关键词:
- Chiari畸形Ⅰ型 /
- 脊髓空洞症 /
- 磁共振相衬技术 /
- 脑脊液动力学
Abstract:ObjectiveTo explore the effects of the cine phase-contrast magnetic resonance imaging(PC-MRI) in evaluating the change of dynamics of cerebrospinal fluid(CSF) on the CSF dynamics in patients with Chiari malformation type Ⅰ(CMⅠ). MethodsSixteen healthy volunteers and 17 CMⅠ and syringomyelia patients were divided into the control goup and CMⅠgroup, respectively.The region between canium and neck of CMⅠ group was detected using PC-MRI scans before and after 12 months of operation, and the control group was checked only once.The changes of CSF velocity and flow at the central segment of midbrain aqueduct, exit segment of the fourth ventricle and second cervical spine level were analyzed. ResultsCompared with the control group, the peak flow velocity of CSF in each examined site in CMⅠ group increased(P < 0.05 to P < 0.01), and the overall flow decreased(P < 0.01).After operation, the peak velocity of CSF in CMⅠ group slowed significantly down(P < 0.01), and the flow increased(P < 0.01).The differences of the peak flow velocity and flow of CSF between the central segment of midbrain aqueduct and second cervical spine level among different prognosis patients were statistically significant(P < 0.05 to P < 0.01). ConclusionsThe improvement of CSF dynamics is related to the prognosis of patients.The application of PC-MRI in monitoring the dynamics of CSF is helpful to evaluate the prognosis of patients with CMⅠ complicated with syringomyelia. -
表 1 CMⅠ组与对照组脑脊液流动参数比较(x±s)
分组 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) CMⅠ组 17 2.24±0.75 55.71±12.28 5.69±0.79 34.44±5.49 6.83±0.69 1.79±0.24 1.93±0.33 4.30±1.19 8.98±2.16 对照组 16 9.06±2.02 74.38±12.64 5.05±0.89 29.19±3.78 6.07±0.61 1.48±0.34 1.48±0.36 3.43±1.16 6.73±2.08 t — 12.71* 4.30 2.19 3.18 3.34 3.04 3.75 2.12 3.04 P — < 0.01 < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 < 0.01 < 0.05 < 0.01 *示t′值 表 2 CMⅠ病人手术前后脑脊液流动各项参数比较(x±s)
时间 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) 术前 17 2.24±0.75 55.71±12.28 5.69±0.79 34.44±5.49 6.83±0.69 1.79±0.24 1.93±0.33 4.30±1.19 8.98±2.16 术后 17 6.94±2.33 80.41±14.92 4.60±0.82 30.28±5.97 5.52±0.62 1.26±0.22 1.41±0.30 3.00±1.00 6.63±1.68 t — 7.92* 5.27 3.95 2.11 5.82 6.71 4.81 3.45 3.54 P — < 0.01 < 0.01 < 0.01 < 0.05 < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 *示t′值 表 3 不同预后病人脑脊液流动各项参数比较(x±s)
CCOS评分/分 n 中脑导水管中央段 四脑室出口段 第二颈椎腹侧 净流量/μL 冲程流量/μL 收缩期峰流速/(cm/s) 时间比/% 舒张期峰流速/(cm/s) 收缩期峰流速/(cm/s) 舒张期峰流速/(cm/s) 收缩期峰流速(cm/s) 舒张期峰流速/(cm/s) >10 12 6.00±0.95 32.17±7.71 4.23±0.65 26.72±2.12 5.22±0.45 1.20±0.22 1.36±0.31 2.66±0.89 5.97±1.28 ≤10 5 1.60±1.14 6.80±3.96 5.48±0.41 38.83±0.94 6.24±0.31 1.41±0.15 1.54±0.28 3.83±0.82 8.22±1.52 t — 8.23 6.90 3.94 12.11 4.59 1.94 1.12 2.52 3.14 P — < 0.01 < 0.01 < 0.01 < 0.01 < 0.01 >0.05 >0.05 < 0.05 < 0.01 -
[1] KORBECKI A, ZIMNY A, PODGÓRSKI P, et al. Imaging of cerebrospinal fluid flow: fundamentals, techniques, and clinical applications of phase-contrast magnetic resonance imaging[J]. Pol J Radiol, 2019, 84: e240. doi: 10.5114/pjr.2019.86881 [2] HOFKES SK, ISKANDAR BJ, TURSKI PA, et al. Differentiation between symptomatic Chiari Ⅰ malformation and asymptomatic tonsilar ectopia by using cerebrospinal fluid flow imaging: initial estimate of imaging accuracy[J]. Radiology, 2007, 245(2): 532. doi: 10.1148/radiol.2452061096 [3] QUON JL, GRANT RA, DILUNA ML. Multimodal evaluation of CSF dynamics following extradural decompression for Chiari malformation type Ⅰ[J]. J Neurosurg Spine, 2015, 22(6): 622. doi: 10.3171/2014.10.SPINE1433 [4] LOE ML, VIVAS-BUITRAGO T, DOMINGO RA, et al. Prognostic significance of C1-C2 facet malalignment after surgical decompression in adult Chiari malformation type Ⅰ: a pilot study based on the Chicago Chiari Outcome Scale[J]. J Neurosurg Spine, 2020, 6: 1. [5] STRUCK AF, HAUGHTON VM. Idiopathic syringomyelia: phase-contrast MR of cerebrospinal fluid flow dynamics at level of foramen magnum[J]. Radiology, 2009, 253(1): 184. doi: 10.1148/radiol.2531082135 [6] 尚华, 刘怀军, 闫乐卡, 等. 电影相位对比成像定量研究不同年龄颈椎管内脑脊液运动[J]. 中国医学影像技术, 2011, 27(3): 491. [7] FAKHRI A, SHAH MN, GOYAL MS. Advanced imaging of Chiari Ⅰ malformations[J]. Neurosurg Clin N Am, 2015, 26(4): 519. doi: 10.1016/j.nec.2015.06.012 [8] D'URSO PI. Minimally invasive posterior fossa decompression in Chiari Ⅰ malformation[J]. Surg Neurol Int, 2019, 10: 138. doi: 10.25259/SNI-347-2019 [9] LINGE SO, MARDAL KA, HELGELAND A, et al. Effect of craniovertebral decompression on CSF dynamics in Chiari malformation type Ⅰ studied with computational fluid dynamics: Laboratory investigation[J]. J Neurosurg, 2014, 21(4): 559. [10] 陆笑非, 舒建, 杨述根, 等. PC-MRI在Ⅰ型Chiari畸形伴脊髓空洞症患者枕大池成形术中的应用[J]. 中国医学影像技术, 2017, 33(5): 688. -





 下载:
下载: