-
众所周知,深Ⅱ度烧伤可对皮肤真皮层造成损伤,易引发全身感染,增加创面脓毒症几率,且创面恢复后易留瘢痕,除了外观影响外,还可能影响肢体功能,给病人身心带来伤害,甚至致残或自杀[1]。为此,采取何种方式修复创面一直为烧伤干预重点。目前创面修复不仅要治愈创面,而且要求减少瘢痕形成,改善创面外观。近年来表皮生长因子凝胶制剂等外源性细胞因子在烧伤创面修复中应用较多,可促上皮细胞再生、增殖,加速创面愈合[2-3]。但深Ⅱ度烧伤创面溶痂为细菌繁殖创造条件,易感染,而外源性细胞因子抗感染能力不足。为此,对深Ⅱ度烧伤创面建议联合抗感染药物干预[4]。纳米银具有广谱抗菌作用,抗菌作用强,将其作为敷料用于烧伤创面治疗能快速释放纳米银离子,快速杀灭创面细菌、真菌等,控制感染的同时能止痛,且能增强外源性表皮生长因子的作用,减少创面愈合时间。本研究对深Ⅱ度烧伤病人创面行纳米银敷料联合表皮生长因子凝胶制剂治疗,效果较为理想。现作报道。
-
选择我院2016年3月至2018年3月住院治疗的深Ⅱ度烧伤病人,纳入标准:(1)符合《烧伤治疗学》中深Ⅱ度烧伤诊断标准[5],面积6%~10%体表总面积(TBSA),深Ⅱ度;(2)年龄1~80岁;(3)烧伤后2 d内治疗;(4)热烧伤;(5)创面均未自行治疗。排除标准:(1)电烧伤、化学性烧伤;(2)孕妇、母乳喂养者;(3)过敏体质;(4)明显营养不良、重要脏器损伤、严重全身感染;(5)入组前有用药史;(6)糖尿病;(7)严重合并伤。剔除与纳入标准不符、可能影响疗效评估、不依从的病人。因不良事件、相关指标显著异常而停药者、其他原因影响疗效评估或中途退出者予以脱组处理。最终入组病人156例。按随机数字表法将病人分为观察组与对照组,各78例。观察组中男50例,女28例;年龄(30.00±5.02)岁;深Ⅱ度烧伤面积(7.54±1.10)%TBSA;其中热水烫伤55例,火焰烧伤23例。对照组男45例,女33例;年龄(31.15±4.76)岁;深Ⅱ度烧伤面积(8.54±0.97)%TBSA;其中热水烫伤51例,火焰烧伤27例。2组病人一般资料具有可比性。本研究经我院伦理委员会审核通过,病人均签署知情同意书。
-
2组病人入院后均接受补液抗感染、抗休克等对症处理,所有病人均接受0.5%聚维酮碘、灭菌注射用水清创消毒。对照组病人清创后对创面行重组人表皮生长因子凝胶(桂林华诺威基因药业有限公司,批号201509077A、201603001A)涂抹,厚度1 mm左右,涂抹完成后无菌纱布包扎,一般间隔1 d更换药物1次。观察组病人清创后对创面涂抹纳米银敷料(深圳市爱杰特医药科技有限公司,批号160101、170302)联合重组人表皮生长因子凝胶,两者按1:1比例混匀,涂抹均匀,厚度1 mm左右,无菌纱布包扎,一般间隔1 d更换药物1次。治疗1周、2周、3周、4周观察2组病人创面情况。
-
(1) 换药时观察对2组病人创面情况;(2)治疗前、治疗结束后1周通过视觉模拟评分(VAS)评价2组病人创面疼痛情况,采取自评形式,0~10分,分数越高表示越疼痛;(3)记录2组治疗1周、2周、3周、4周创面溶痂率[方格纸法计算,更换药物前经由透明方格纸顺着创面痂皮边缘对创面大小描绘,借助方格数对痂皮面积计算,即(1-治疗后/治疗前痂皮面积)×100%]、完全溶痂时间(创面坏死组织溶解,基底颜色鲜红即完全溶痂)、创面愈合时间(按照创面愈合95%评估);(4)治疗1周、2周、3周、4周换药前采集2组病人创面分泌物,进行细菌培养,检出细菌判断为阳性,统计2组创面细菌阳性率;(5)治疗前、治疗2周采集病人创面边缘组织标本,通过免疫组织化学法测定创面基质金属蛋白酶(MMP)-1、MMP-2表达,计算积分吸光度值。(6)观察2组病人治疗前后相关不良反应发生情况。
-
采用t检验和χ2检验。
-
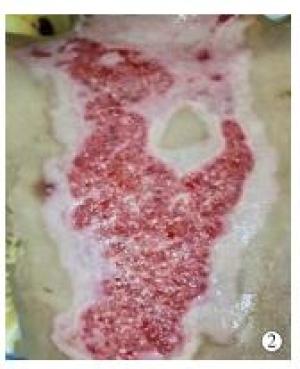
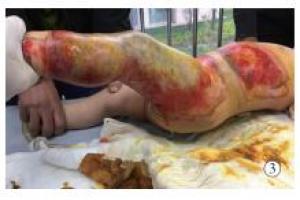
观察组治疗4 d创面痂皮慢慢变软,和基底相接的纤维条索变少;治疗6 d大多数痂壳慢慢脱落;治疗8 d病人创面痂皮基本溶解,基底鲜红色,深层肉芽组织快速增多,创缘附近上皮化明显。典型病例图片见图 1、2。对照组治疗4 d创面和基底坏死组织形成干痂;治疗6 d病人创面比较干燥,部分黄白色坏死组织变成黄黑色,坏死组织尚未脱落;治疗8 d病人创面干痂慢慢软化;治疗10 d可见基底肉芽组织生长,干痂慢慢脱落。典型病例图片见图 3、4。
-
治疗前,2组病人VAS评分差异无统计学意义(P>0.05);治疗后2组VAS评分明显低于治疗前(P < 0.01),且观察组明显低于对照组(P < 0.01)(见表 1)。
分组 n 治疗前 治疗后 t P 观察组 78 7.55±1.24 2.15±0.60 51.84 < 0.01 对照组 78 7.49±1.31 4.03±0.75 29.67 < 0.01 t — 0.29 17.29 — — P — >0.05 < 0.01 — — 表 1 2组病人治疗前后VAS评分比较($\overline x \pm s$;分)
-
观察组治疗1周、2周创面溶痂率均明显高于对照组(P < 0.01)(见表 2);2组病人治疗3周、4周创面溶痂率均100%。
分组 n 治疗1周 治疗2周 观察组 78 76.45±7.12 96.72±3.05 对照组 78 60.00±8.13 87.35±6.24 t — 13.44 11.92 P — < 0.01 < 0.01 表 2 2组病人创面溶痂率比较($\overline x \pm s$;%)
-
观察组完全溶痂时间、创面愈合时间均明显短于对照组(P < 0.01)(见表 3)。
分组 n 完全溶痂时间 创面愈合时间 观察组 78 8.00±2.93 19.35±3.08 对照组 78 12.56±3.60 23.84±4.76 t — 8.68 7.00 P — < 0.01 < 0.01 表 3 2组病人完全溶痂时间、创面愈合时间比较($\overline x \pm s$;d)
-
观察组创面细菌阳性率为11.54%,低于对照组的24.36%(χ2=4.35,P < 0.05)。共28例病人创面细菌阳性,主要为铜绿假单胞菌、金黄色葡萄球菌、大肠埃希菌(见表 4)。
菌株 菌株数/株 构成比/% 铜绿假单胞菌 10 30.30 金黄色葡萄球菌 8 24.24 大肠埃希菌 6 18.18 鲍曼不动杆菌 5 15.15 其他 4 12.12 合计 33 100.00 表 4 28例细菌阳性病人菌株分布情况
-
治疗前2组病人创面MMP-1、MMP-2表达水平比较差异无统计学意义(P>0.05);与治疗前比较,治疗2周2组病人MMP-1、MMP-2表达水平均明显下降,且观察组均明显低于对照组(P < 0.01)(见表 5)。
分组 n MMP-1 MMP-2 治疗前 观察组 78 4 493.50±251.00 2 760.10±213.45 对照组 78 4 500.00±264.72 2 752.50±256.34 t — 0.16 0.20 P — >0.05 >0.05 治疗2周 观察组 78 1 650.00±168.30** 1 500.00±150.25** 对照组 78 3 012.50±203.34** 1 998.47±168.98** t — 45.59 19.47 P — < 0.01 < 0.01 组内配对t检验:**P < 0.01 表 5 2组病人治疗前后创面MMP-1、MMP-2光密度值比较($\overline x \pm s$)
-
对照组病人主观感觉到烧灼感1例,30 min后自行缓解,2组病人均无过敏反应出现。2组病人血常规检查未发现与药物相关的不良反应。
-
深Ⅱ度烧伤治疗重点在于避免感染,促进残留皮肤组织修复或再生[6]。烧伤创面愈合需多种细胞因子参与,其中促进多种细胞有丝分裂的表皮生长因子发挥重要作用。重组人表皮生长因子凝胶制剂由基因重组技术研制而成,不仅可促细胞增殖、分裂,而且能促肉芽组织生长、创面再上皮化,在瘢痕修复等医学美容方面应用较广泛[7-8]。但重组人表皮生长因子凝胶制剂抗菌效果有限,而对烧伤病人治疗须兼顾抗菌处理。目前关于重组人表皮生长因子联合抗菌药物治疗烧伤创面报道较多,如联合磺胺嘧啶锌[9]、联合银花解毒散[10]等。另外,不同研究设计不同,李烨等[11]以纳米银敷料为对照,观察其联合重组人表皮生长因子凝胶治疗效果。周忠志等[12]以磺胺嘧啶银为对照,分析重组人表皮生长因子+纳米银治疗的效果。本研究选择研究药物中的重组人表皮生长因子凝胶制剂单药为对照,体现药物单用与联合抗菌药物的治疗效果。
纳米银直径小而表面积大,除了渗透性强外,其抗菌能力相比传统银离子更强。纳米银结合无菌纱布干预,接触创面后能快速释放银离子,抗菌作用起效快且持续时间较长。焦建强等[13]研究发现纳米银敷料联合重组人表皮生长因子能明显缩短创面愈合时间,增强烧伤后美观度。本研究发现纳米银敷料联合重组人表皮生长因子凝胶治疗能明显减轻烧伤病人创面疼痛,这可能与纳米银敷料抗炎、重组人表皮生长因子凝胶修复创面,协同减轻疼痛有关。本研究结果显示,与单用重组人表皮生长因子凝胶制剂相比,纳米银敷料联合重组人表皮生长因子凝胶治疗烧伤,其治疗1周、2周创面溶痂率均明显提高,完全溶痂时间及创面愈合时间均明显缩短,这与纳米银发挥抗菌作用、表皮生长因子促细胞增殖、分裂、肉芽组织生长、创面再上皮化等作用有关[14]。其中纳米银可能作用机制为:银颗粒遇水后形成银离子,有杀菌作用,且银颗粒可在病原微生物表面吸附,让微生物凹陷,同时结合病原体内特定蛋白基团,最终造成病原体死亡[15];纳米银还能通过和细菌DNA直接结合,影响细胞结构,致细胞死亡[16-17]。可见纳米银敷料联合重组人表皮生长因子治疗不仅能满足烧伤抗感染的基础,而且可促进创面修复,加快创面愈合速度。有研究[18-19]发现纳米银还能促重组人表皮生长因子更好地发挥修复创面的作用,加快创面上皮再生及肉芽组织形成,进而缩短愈合时间。同时,本研究发现细菌培养阳性病人中,检出细菌株数比病人例数多,提示深Ⅱ度烧伤创面感染的病人有多种细菌定植,其中以铜绿假单胞菌最多,其次是金黄色葡萄球菌,为临床抗菌药物使用提供参考。但受样本例数较少的影响,本研究未对照分析2组菌株数及药物对不同细菌的干预效果。
MMPs和细胞外基质降解有关,在创面胶原降解中发挥重要作用[20]。本研究结果显示观察组治疗2周创面MMP-1、MMP-2表达水平均明显低于对照组,提示纳米银敷料联合表皮生长因子凝胶制剂可能通过抑制创面组织MMP-1、MMP-2表达,以控制创面胶原降解,避免创面胶原蛋白流失,促进创面愈合。安全性方面,本研究发现仅对照组1例病人出现烧灼感,但30 min后消失,提示纳米银敷料联合重组人表皮生长因子治疗烧伤病人较为安全。
综上所述,纳米银敷料联合表皮生长因子凝胶制剂治疗深Ⅱ度烧伤创面具有溶痂率高、完全溶痂时间和创面愈合时间短、细菌清除率高等特点,且安全性高,其促创面愈合机制可能与下调MMP-1、MMP-2表达有关。
纳米银敷料联合表皮生长因子凝胶制剂对深Ⅱ度烧伤创面溶痂及愈合的影响
Effect of nanometer silver dressing combined with epidermal growth factor gel on the wound dissolved scab and healing of deep Ⅱ degree burn
-
摘要:
目的 分析纳米银敷料联合表皮生长因子凝胶制剂在深Ⅱ度烧伤创面治疗中的应用效果。 方法 按随机数字表法将156例深Ⅱ度烧伤病人分为观察组与对照组,各78例。观察组病人清创后给予纳米银敷料联合表皮生长因子凝胶制剂治疗,对照组病人清创后给予表皮生长因子凝胶制剂治疗。换药时观察创面情况。比较2组病人治疗前、治疗后1周创面视觉模拟评分(VAS)、治疗1周、2周、3周、4周创面溶痂率、细菌培养阳性率及完全溶痂时间、创面愈合时间,治疗前、治疗2周通过免疫组织化学法测定基质金属蛋白酶(MMP)-1、MMP-2表达,并记录治疗前后相关不良反应发生情况。 结果 观察组治疗4 d创面痂皮变软,6 d大部分痂壳脱落,8 d创面痂皮基本溶解;对照组治疗4 d创面干痂形成,6 d创面干燥,部分坏死组织呈黄黑色,但尚未脱落,8 d干痂逐渐软化,10 d干痂逐渐脱落,基底肉芽组织生长。治疗后2组VAS评分明显低于治疗前(P < 0.01),且观察组明显低于对照组(P < 0.01)。观察组治疗1周、2周创面溶痂率均明显高于对照组(P < 0.01)。观察组完全溶痂时间、创面愈合时间均明显短于对照组(P < 0.01)。观察组创面细菌阳性率为11.54%,低于对照组的24.36%(P < 0.05)。与治疗前比较,治疗2周2组病人MMP-1、MMP-2表达水平均明显下降,且观察组均明显低于对照组(P < 0.01)。 结论 纳米银敷料联合表皮生长因子凝胶制剂治疗深Ⅱ度烧伤创面溶痂率高,创面愈合时间较短,其机制可能与抑制创面MMP-1、MMP-2表达相关。 -
关键词:
- 烧伤 /
- 纳米银敷料 /
- 表皮生长因子凝胶制剂 /
- 溶痂
Abstract:Objective To analyze the effects of nanometer silver dressing combined with epidermal growth factor gel on the wound treatment of deep Ⅱ degree burn. Methods One hundred and fifty-six patients with deep Ⅱ degree burn were randomly divided into the observation group and control group by digital table method (78 cases in each group).After the debridement, the observation group was treated with nanometer silver dressing combined with epidermal growth factor gel, and the control group was treated with epidermal growth factor gel.The wound surface condition was observed at changing the dressing.The visual analogue scale (VAS) of wound before and after 1 week of treatment, scab solubility of wound surface after 1, 2, 3 and 4 weeks of treatment, positive rate of bacterial culture, time of completing dissolution and healing time of wound were compared between two groups.The expression levels of matrix metalloproteinase-1 and 2 (MMP-1 and MMP-2) in two groups before and after 2 weeks of treatment were detected using immunohistochemistry.The incidence rates of adverse reactions before and after treatment were recorded. Results In the observation group, the wound scab skin became soft on the 4th day, most of the scab shell fell off on the 6th day, and the wound scab skin basically dissolved on the 8th day.In the control group, the dry scab wound formed on the 4th day, the wound became dry on the 6th day, some necrotic tissues were yellowish black, but not yet shed, the dry scab gradually softened on the 8th day, and the dry scab gradually fell off and basal granulation tissue grew on the 10th day.After treatment, the VAS scores in two groups were significantly lower than that before treatment (P < 0.01), and which in observation group was significantly lower than that in control group (P < 0.01).The wound dissolving rates in observation group at 1 and 2 weeks after treatment were significantly higher than that in control group (P < 0.01).The dissolution time and wound healing time in observation group were significantly shorter than those in control group (P < 0.01).The positive rate of bacteria in observation group (11.54%) was significantly lower than that in control group (24.36%) (P < 0.05).Compared with before treatment, the expression levels of MMP-1 and MMP-2 in two groups significantly decreased, and which in observation group were significantly lower than those in control group (P < 0.01). Conclusion The nanometer silver dressing combined with epidermal growth factor gel in the treatment of the wound of deep Ⅱ degree burn has high dissolving rate of scab and short wound healing time, the mechanism of which may be related to the expression inhibition of MMP-1 and MMP-2 in wounds. -
Key words:
- burn /
- nanometer silver dressing /
- epidermal growth factor gel /
- dissolved scab
-
表 1 2组病人治疗前后VAS评分比较(
$\overline x \pm s$ 分组 n 治疗前 治疗后 t P 观察组 78 7.55±1.24 2.15±0.60 51.84 < 0.01 对照组 78 7.49±1.31 4.03±0.75 29.67 < 0.01 t — 0.29 17.29 — — P — >0.05 < 0.01 — — 表 2 2组病人创面溶痂率比较(
$\overline x \pm s$ 分组 n 治疗1周 治疗2周 观察组 78 76.45±7.12 96.72±3.05 对照组 78 60.00±8.13 87.35±6.24 t — 13.44 11.92 P — < 0.01 < 0.01 表 3 2组病人完全溶痂时间、创面愈合时间比较(
$\overline x \pm s$ 分组 n 完全溶痂时间 创面愈合时间 观察组 78 8.00±2.93 19.35±3.08 对照组 78 12.56±3.60 23.84±4.76 t — 8.68 7.00 P — < 0.01 < 0.01 表 4 28例细菌阳性病人菌株分布情况
菌株 菌株数/株 构成比/% 铜绿假单胞菌 10 30.30 金黄色葡萄球菌 8 24.24 大肠埃希菌 6 18.18 鲍曼不动杆菌 5 15.15 其他 4 12.12 合计 33 100.00 表 5 2组病人治疗前后创面MMP-1、MMP-2光密度值比较(
$\overline x \pm s$ 分组 n MMP-1 MMP-2 治疗前 观察组 78 4 493.50±251.00 2 760.10±213.45 对照组 78 4 500.00±264.72 2 752.50±256.34 t — 0.16 0.20 P — >0.05 >0.05 治疗2周 观察组 78 1 650.00±168.30** 1 500.00±150.25** 对照组 78 3 012.50±203.34** 1 998.47±168.98** t — 45.59 19.47 P — < 0.01 < 0.01 组内配对t检验:**P < 0.01 -
[1] 冯启凯, 曲梅花, 季万胜, 等.冰王烧烫膏对大鼠深Ⅱ度烧伤的修复及机制研究[J].安徽医药, 2015, 19(2):236. doi: 10.3969/j.issn.1009-6469.2015.02.009 [2] 周牮, 李影学, 迟云飞, 等.表皮生长因子溶液配合负压封闭引流技术治疗深Ⅱ度烧伤创面的疗效观察[J].感染·炎症·修复, 2015, 16(1):49. [3] 王鹏, 高鹏, 张超, 等.重组人表皮生长因子凝胶在急诊创伤患者中的疗效分析[J].贵州医药, 2018, 42(3):308. doi: 10.3969/j.issn.1000-744X.2018.03.019 [4] 王强, 彭友林.表皮生长因子联合银离子敷料治疗压力性溃疡创面炎性反应的观察[J].中国美容医学, 2018, 27(6):28. [5] 杨宗城.烧伤治疗学[M].3版.北京:人民卫生出版社, 2006:5. [6] 蔡景宁, 孙玉静, 谢晓繁, 等.重组人粒细胞巨噬细胞集落刺激因子凝胶对深Ⅱ度烧伤创面溶痂的效果分析[J].中国临床医生杂志, 2017, 45(1):39. doi: 10.3969/j.issn.2095-8552.2017.01.013 [7] 蒋屏东, 孙慧, 郑渊, 等.重组人表皮生长因子在面部瘢痕修复治疗中的应用[J].现代生物医学进展, 2017, 17(33):6502. [8] 祝霞, 孙丽玲.强脉冲光联合重组人表皮生长因子凝胶治疗面部激素依赖性皮炎的疗效观察[J].中国现代医学杂志, 2017, 27(2):91. doi: 10.3969/j.issn.1005-8982.2017.02.017 [9] 韩悦, 任杰, 伍锦华, 等.重组人表皮生长因子联合磺胺嘧啶锌凝胶治疗深Ⅱ度烧伤创面的疗效观察[J].广西医科大学学报, 2017, 34(9):1354. [10] 张钒.银花解毒散配合重组人表皮生长因子对深Ⅱ度烧伤创面愈合的影响[J].现代中西医结合杂志, 2016, 25(28):3125. doi: 10.3969/j.issn.1008-8849.2016.28.015 [11] 李烨, 焦建强, 黄喆, 等.纳米银敷料联合重组人表皮生长因子凝胶对烧伤创面的安全性和有效性研究[J].中国医药导刊, 2015, 17(9):941. doi: 10.3969/j.issn.1009-0959.2015.09.040 [12] 周忠志, 黄新灵.重组人表皮生长因子凝胶联合纳米银敷料对深Ⅱ度烧伤患者创面总体细菌培养阳性率及愈合时间的影响[J].中国地方病防治杂志, 2017, 32(12):1400. [13] 焦建强, 李烨, 黄喆, 等.重组人表皮生长因子凝胶联合纳米银敷料对烧伤后瘢痕的影响[J].中国组织工程研究, 2015, 19(25):4007. doi: 10.3969/j.issn.2095-4344.2015.25.014 [14] 蒋琪霞, 刘玉秀, 李晓华, 等.177例慢性伤口应用纳米银敷料的效果研究[J].中华护理杂志, 2015, 50(8):932. doi: 10.3761/j.issn.0254-1769.2015.08.008 [15] 占卫兵.纳米银敷料与重组人表皮生长因子联合治疗Ⅱ度烧伤的疗效分析[J].中华全科医学, 2015, 13(6):926. [16] AKGVL EA, KARAKAYA J, AYDIN S.Role of comorbidities as limiting factors to the effect of hyperbaric oxygen in diabetic foot patients:a retrospective analysis[J].Diabetes Ther, 2014, 5(2):535. [17] DOGGEN K, VAN ACKER K, BEELE H, et al.Implementation of a quality improvement initiative in Belgian diabetic foot clinics:feasibility and initial results[J].Diabetes Metab Res Rev, 2014, 30(5):137. [18] TUGULEA AM, BÉRUBÉ D, GIDDINGS M, et al.Nano-silver in drinking water and drinking water sources:stability and influences on disinfection by-product formation[J].Environ Sci Pollut Res Int, 2014, 21(20):11823. doi: 10.1007/s11356-014-2508-5 [19] PALANIAPPAN P, SATHISHKUMAR G, SANKAR R.Fabrication of nano-silver particles using Cymodocea serrulata and its cytotoxicity effect against human lung cancer A549 cells line[J].Spectrochim Acta A Mol Biomol Spectrosc, 2015, 138(2015):885. [20] JEONG HS, LEE BH, LEE HK, et al.Negative pressure wound therapy of chronically infected wounds using 1% acetic acid irrigation[J].Arch Plast Surg, 2015, 42(1):59. -





 下载:
下载: